
What is a Bad Psychedelic Trip? Key Facts and Definitions
In psychedelic culture, a bad psychedelic trip is typically framed as a psychedelic experience that is distressing in some way. Usually, it is a type of experience involving prolonged distress that feels difficult to manage or a series of challenging moments that seem to outweigh the positives.
However, what many people call a bad trip can, in many contexts, be framed in less black-and-white language. These experiences may later be interpreted positively, such as meaningful, insightful, therapeutic, or cathartic. People may find it helpful to view this type of experience as difficult or challenging, rather than simply bad.
This article looks at the difference between bad trips and challenging experiences, what a bad psychedelic trip involves, the contributing factors, and what can be learned from difficult psychedelic experiences.
Bad Psychedelic Trip vs Challenging Experience: Key Differences Explained
A bad psychedelic trip is a highly distressing experience, sometimes a traumatic one, that feels unmanageable and does not resolve into a sense of meaning or insight – either during or after the experience.
A challenging psychedelic experience may also be intense, overwhelming, and characterized by fear or anxiety, but through proper support and integration, it can lead to profound personal growth. This type of experience is not typically thought of as bad in the grand scheme of things, given the value and benefit it provides. For example, a 2016 study on challenging psilocybin experiences found, “Despite difficulties, 84% endorsed benefiting from the experience.”
MycoMeditations does not use the term bad trip to describe a challenging experience, for several reasons.
Based on the distinction between bad trips and difficult experiences highlighted above, people can learn to manage challenging moments through adequate preparation and psychological support, and find positive resolutions through post-session integration.
We acknowledge that in recreational settings, poorly planned contexts, or with bad facilitation, psychedelic experiences can become extremely distressing or lead to extended emotional difficulties. When people are destabilized following these types of experiences, they may struggle, in the long term, with anxiety, depression, depersonalization, derealization, social disconnection, or existential confusion.

But with research-backed and professional preparation, support, and integration in place, classic bad psychedelic trips are rare. In carefully planned and supervised psychedelic clinical trials, participants may experience transient anxiety and the arising of painful memories, but it is uncommon for this to result in an unmanageable experience or long-term issues.
The 2016 study noted above concludes, “The incidence of risky behavior or enduring psychological distress is extremely low when psilocybin is given in laboratory studies to screened, prepared, and supported participants.” For most participants in clinical trials, adequately supported psychedelic experiences, even if they are challenging at times, result in long-term benefits, such as enhanced well-being, life satisfaction, meaning, and spirituality.
Why People Describe Some Psychedelic Experiences as Bad
A psychedelic trip may be described as bad when it feels overwhelming, unmanageable, or leads to lasting difficulties. This may stem from any of the following effects:
- Negative emotions, such as fear, anxiety, dread, panic, dysphoria, and paranoia
- Unsettling visual effects, such as the perception of negative entities
- Thought loops, where the same thought or chain of thoughts repeats over and over
- The feeling of losing one’s mind or “going crazy”
- A fearful ego-dissolving experience, resulting from psychological resistance
- The resurfacing of traumatic memories, which might feel retraumatizing
What Role Do Set and Setting Play in Bad Psychedelic Trips?
Several factors can contribute to a bad psychedelic trip, and these fall under the concept of “set and setting”, where “set” refers to mindset and “setting” refers to aspects of one’s environment.
How Mental Health and Emotional State Affect Psychedelic Trips
A user’s pre-existing emotional state can have a major influence on the quality of a psychedelic experience. For example, if someone has barely slept for one or more nights, this can lead to a more distressing experience, as sleep deprivation is associated with increased anxiety and distress.
Sleep deprivation is also linked to impairments to cognitive functions, such as memory, judgment, discrimination, reaction time, and executive functions, which may affect one’s ability to navigate altered states. Sleep deprivation could make a psychedelic experience more intense, unstable, and distressing.

Clinical researchers and reputable psychedelic clinics and retreats also have rigorous screening in place to minimize the risk of bad psychedelic trips. Exclusion criteria typically include recent suicidality and a personal or family history of psychosis, schizophrenia, or bipolar disorder. This is due to concerns about psychedelics triggering or worsening suicidality or psychotic or manic symptoms. Screening for psychiatric contraindications is a crucial aspect of minimizing the risk of a bad psychedelic trip.
Psychedelics can induce intense psychological experiences. It’s of paramount importance to have a baseline of emotional and mental stability. This should involve basic skills related to self-awareness, emotional regulation, and tolerance of discomfort. It means being able to notice when distress is beginning to worsen and to use techniques to navigate this mental spiral.
Self-awareness also involves knowledge of one’s past or trauma history and how it affects one today. Since psychedelics may lead to confrontations with events from the past, it’s vital to know that this can occur, as well as to have the willingness and ability to explore this material and its potential therapeutic value.
Why Expectations Can Shape a Psychedelic Experience
The expectations you have about an upcoming psychedelic experience, or psychedelics in general, can also affect how the journey unfolds. If you don’t know, acknowledge, or appreciate the possibility of challenging emotions or dramatic shifts in experience, distress is more likely. Expecting an easy, completely controllable experience, and one that is full of only positive emotions, is unrealistic.
It’s important to have realistic expectations around the psychedelic experience. This means understanding that it can be unpredictable, intense, or emotionally difficult at times. Without this knowledge, it’s more likely for someone to experience overwhelm, panic, or resistance to the unfolding effects.
How to Know If You’re Ready for a Psychedelic Experience
Another aspect of set is personal readiness. This encompasses not just realistic expectations but also knowledge, techniques, and skills in navigating altered states.
A 2024 study observed, “Participants differed substantially in their ability to let go of control. Some were able to surrender to the experience, reassured by their (trust in) therapists, but for others this remained challenging.” The authors add that, for some participants, “giving into the experience was challenging or even frightening due to the lack of agency or their inability to steer the experience in a specific direction, and some were unable to ask for help during difficult moments.”
Research has found that adopting an attitude of acceptance and surrender – or “trust, let go, and be open” – is associated with more positive and therapeutic experiences. This strategy may help shorten any periods of struggle, which is important since, as a 2018 paper notes, “the duration of struggle is predictive of negative outcomes.”
You can find out your level of readiness for a psychedelic experience by answering this survey based on the Psychedelic Preparedness Scale (PPS), developed by researchers at University College London (UCL).
How Environment and Setting Affect Psychedelic Trips
It is not just one’s inner landscape that shapes a psychedelic experience, but elements of the outer environment, too. Features of the setting that can increase the risk of a bad psychedelic trip include:
- A lack of psychological support in general
- Misguided psychological support, such as from a stranger, friend, or untrained or unprofessional facilitator
- Taking psychedelics around people one doesn’t know or trust
- Not fully trusting or feeling an alliance with the facilitator
- Negative interactions with, or negative responses from, other people
- Having a psychedelic experience under the supervision of an unethical facilitator
- A noisy, chaotic, or overstimulating space, such as a club, party, festival, or urban setting
- Harsh music, lighting, or smells
- A cluttered and messy indoor space
The risks of a bad psychedelic trip can be minimized when there is adequate psychological support from a trusted facilitator, the presence of nature, a calming and comfortable environment, and a carefully curated playlist.
Common Themes People Report During Difficult Psychedelic Experiences
During challenging psychedelic experiences, which don’t have to be framed as bad, people report some common themes, including:
- Intense fear or anxiety, which may center around the feeling of losing control or going insane
- Losing the sense of self, or ego dissolution, which may be experienced as confusing, scary, isolating, like dying, or as detachment from reality
- Resurfacing trauma, where traumatic memories are re-experienced in a direct or symbolic way
- ‘Ontological shock’: the experience may challenge one’s beliefs about reality so profoundly that it induces a state of overwhelm, confusion, and rumination
- A sense of encountering negative entities
- Time distortion effects, such as time dilation (e.g., minutes feeling like hours) or the feeling that one is stuck in a timeless moment
- Perceptual effects, such as disturbing visions
- Cognitive effects, such as thought loops
- Somatic effects, such as leaving the body or the body dissolving
While these effects can be challenging at the time, it’s important to reiterate that their challenging nature doesn’t mean that users reflect on the experience negatively. As we’ve seen, research has shown that most people view their difficult psychedelic experiences in positive terms.
One way to understand people’s positive evaluation of their most challenging experiences is through the lens of psychedelic integration.
Psychedelic Integration: What Can Be Learned From a Challenging Psychedelic Experience?
Integrating a challenging psychedelic experience involves searching for clear insights, as well as how to put those insights into action.
At MycoMeditations, thousands of psilocybin therapy sessions have shown us that emotionally difficult psilocybin experiences can be sources of profound meaning and growth, so we work with guests to reliably unearth these benefits. As a result, we see how it can be premature to label any challenging psychedelic experience as simply bad, as there are typically clear aspects to draw healing from through the difficulty.
Based on the research we’ve outlined, stories from retreat attendees, and the common themes of challenging psychedelic experiences, the following lessons are possible:
- Confronting and taking a new perspective on traumatic memories or repressed emotions, which for many users involves adopting an attitude of self-compassion.
- Learning to accept and connect to an experience, rather than push it away, can reduce the feelings of distress associated with it.
- Viewing dissolution of the sense of self as an opportunity to construct a healthier, more adaptive self-model, thereby challenging rigid patterns of self-criticism and low self-esteem.
- Ascertaining important insights from entities, which could relate to one’s emotions, behaviors, relationships, or life path. An entity encounter may also lead to a sense of spiritual expansion, as researchers have connected these experiences to states of awe and changes to one’s beliefs about fundamental reality.
- Acute ontological shock during or after a psychedelic experience may lead to a re-evaluation of existential concerns, perhaps altering one’s views on what the psychotherapist Irvin Yalom called our “ultimate concerns”: death, freedom, isolation, and meaninglessness.
Important Perspectives to Consider When Talking About a Bad Psychedelic Trip
When the topic of bad psychedelic trips arises, it’s important to consider whether the user feels there has been a positive resolution to that experience or if there is lasting harm.
When psychedelic experiences lack adequate psychological support, a person may struggle to confront and work through difficult psychological material, which is essential when it comes to difficult psychedelic journeys. And without integration in place, such as facilitated group discussions at retreats or one-on-one psychotherapy sessions, there is a lack of opportunity to make sense of difficult experiences and process any residual emotions connected to them.
When the intention is to use psychedelics therapeutically, it’s crucial to have preparation, support, and integration in place, so that one is better able to transform challenging experiences into personal growth.
It can be premature to judge a psychedelic experience as completely or irrevocably bad based on it being uncomfortable, or even because of a degree of difficult adjustment after an experience. Reputable psychedelic therapists or retreats will support participants with further integration resources and practices, which allow them to build new perspectives about their experience. Through this process, distressing emotions, thoughts, or visions during a psychedelic experience can lead to lasting personal breakthroughs.
Because of the potential of a psychedelic experience to generate new insights and opportunities for self-growth, it can be helpful to reframe bad trips as challenging. This framing helps many participants view their emotionally difficult experiences as potentially therapeutic and transformative.

Burnout Recovery with Psilocybin for Executives and Leaders
Many high-performing professionals struggle with burnout. More than 50% of managers feel burned out, a worrying statistic that is confirmed by later research, showing that 56% of leaders experience this. A 2022 Deloitte study found that 70% of C-suite executives have considered quitting because of burnout.
Burnout recovery often involves changes to workload, approach to work, and lifestyle, to ensure that stress levels don’t reach unmanageable and extreme levels. Stress is expected and normal among leaders and executives.
The demand on entrepreneurs and leaders who’ve started their own companies, for instance, is often high. All sorts of stressors are present, including high-stakes financial responsibility, funding and managing cash flow, hiring and retaining talent, managing conflict, and fighting for attention in a competitive market. It is natural for these leaders to become stressed out and worried about these matters from time to time.

But when stress levels become chronic and severe, it leads to burnout, where a person experiences a state of emotional, mental, and physical exhaustion. To handle this, leaders must make sure to effectively cultivate and harness inner and outer resources.
The therapeutic use of psilocybin is emerging as a novel and effective way to reduce or resolve burnout in executives and professionals. As we will see, there are multiple levels at which psilocybin can help with burnout recovery, supported through research.
What Is Burnout Recovery? Symptoms, Causes, and Long-Term Impact
Burnout recovery is the process of restoring physical, mental, and emotional health after a period of sustained and severe stress and exhaustion. This may involve setting strict boundaries, prioritizing self-care to protect one’s mental and physical health, and taking other steps that can reduce stress, such as reducing hours or delegating tasks.
The aim of one or more of these steps is to enhance well-being and a sense of work-life balance, where work and the stresses associated with it don’t negatively affect the rest of one’s life. For instance, burnout is associated with depression and anxiety, sleep impairment, and cardiovascular disease, as well as relationship problems and stress in the home domain.
Research also consistently finds that burnout leads to “lower job satisfaction, absenteeism, and reduced professionalism, productivity, and commitment to the organization.” Another goal of burnout recovery, then, is to ensure that a high-performing professional or executive can perform their role as expected and desired, rather than feel that the stress involved is impairing their ability to do so.
Why High-Performing Professionals Experience Burnout: Key Causes
Executives can experience burnout for multiple reasons, including:
- Excessive demands
- Insufficient resources and support
- The expectation to act as “shock absorbers” for company crises
- The emotional labor of suppressing emotions and projecting strength and calm
- Overwhelming stakeholder demands and constant high-risk decision-making
- Tying self-worth to results
- Inability to set boundaries
- Toxic workplace cultures
According to Deloitte’s 2025 Workforce Intelligence Report, “mental fatigue, cognitive strain and decision friction are now the leading indicators of burnout, surpassing workload volume for the first time.” While workload can certainly play a role in burnout, it is the decision-making responsibilities and mental strain that many high-performing professionals experience that put them at risk of burnout.
What High Performers Often Get Wrong About Burnout Recovery
One mistake that executive professionals make in their burnout recovery journey is treating recovery with the same attitude that they’ve taken towards work. This can, ironically, lead to a state of exhaustion, as one may become overwhelmed with trying to fill one’s life with self-care routines while also juggling the responsibilities of work and home life.
Leaders should avoid suddenly implementing complex, ambitious, or high-pressure self-care routines. The demands on them are already high. Sensibly handling these demands, while in the process of burnout recovery, means having a clear sense of the time and mental resources available.
Simpler and less ambitious routines and lifestyle changes can still go a long way in reducing mental fatigue and cognitive strain. These are foundational changes, such as adequate sleep, short periods of exercise, micro-breaks, and brief periods of mindfulness meditation. When leaders manage their time effectively, such as by deprioritizing or delegating non-essential tasks, they can make time for short but effective interventions for burnout.

A second major mistake that many high performers make is believing that burnout is the result of a lack of willpower, rather than structural issues with how they work or their workplace, and how these issues contribute to chronic stress and physical and mental depletion.
Executives must avoid blaming themselves for burnout; exhaustion is not a result of personal weakness or failure. More often, it signals a need to proactively build the right support structures within their organization. High-performing professionals thrive when they take steps to make their work more collaborative. This is a sign of effective leadership.
To seek help and support – whether from colleagues, peers, a coach, or a therapist – is not a sign of weakness or incompetence. When high performers view their ability to handle any task or issue on their own as proof of their self-worth or success, this is a recipe for burnout and poses a significant risk to their companies.
How Psilocybin May Support Burnout Recovery in Executives
When we consider the causes and effects of burnout among high-performing professionals, there are several ways that psilocybin can aid in recovery based on what we know about its effects.
How Psilocybin Alters Self Perception and Identity
According to the philosopher Chris Letheby, psychedelics primarily benefit people’s mental health by altering the sense of self. Negative self-image and ideas around one’s unworthiness underlie conditions such as depression and anxiety. One’s thoughts act as fuel for this negative perception of oneself, where one believes one is incompetent, not good enough, or a failure.
One benefit of psilocybin is that it helps individuals see their maladaptive self-model as a constructed story, as one model among other potential ones, and that healthier ideas about oneself are possible.
As we’ve seen, executives are at risk of burnout when their self-worth is attached to their role and the expectations they’ve set themselves with respect to that. By revising the sense of self, high-performers start to see that feelings of worthiness and self-esteem don’t have to come from overwork, excessive self-reliance, or suppression of emotions.
By enhancing people’s sense of authenticity – a recognition of who one is deep down – psilocybin helps high performers recognize how their way of working may be misaligned with their personality, values, and goals. This provides the incentive to make work-related changes that feel more authentic to them as a leader.
How Psilocybin May Reduce Rumination and Negative Thought Patterns
Burnout is often characterized by rumination. For executives and leaders, this can involve repeated negative thoughts about work, such as worst-case outcomes, deadlines, mounting responsibilities, or negative judgments about how they are handling the work.
Rumination, as seen in depression, has been linked to overactivity in the default mode network (DMN), a brain hub responsible for self-referential thinking, where incoming information, experiences, and memories are related to one’s self-concept. Psilocybin dampens activity in the DMN, helping people break free from rigid patterns of thinking.
For leaders in need of burnout recovery, this quieting of the DMN is liberating. Executives start to gain a more realistic perception of their role and work-related situations, what’s in their control and what isn’t, which reduces stress levels and anxiety.
How Psilocybin May Increase Self-Compassion and Emotional Resilience
Research has found that psilocybin treatment promotes self-compassion, allowing people to feel a sense of care and kindness towards themselves and an ability to truly recognize their suffering. This can provoke a motivation to alleviate it.
One of the issues underlying distress and burnout among business leaders is heightened self-criticism, self-judgment, and a lack of self-compassion. High-performers may carry out their roles in ways that are detrimental to their mental health. The expectation to accept unhealthy levels of stress takes priority over one’s own well-being. Conversely, developing kindness towards oneself has been shown to improve the well-being and effectiveness of leaders.
Psilocybin enhances self-compassion, so when used by executives, it often enables them to view their emotional and physical health as a much bigger priority. Out of a genuine wish to feel well and derive fulfillment from life, they gain the motivation to make tangible changes to the way they work.
Moreover, increases in self-compassion following a psilocybin experience can lead to the adoption of healthy habits, driven by a desire to take care of oneself. In relation to burnout recovery, some of these beneficial self-care habits include better sleep hygiene, a healthier diet, a mindfulness meditation practice, regular exercise, and more time spent in nature. All of these changes go a long way in managing stress levels during burnout recovery.
Self-compassion is a strength; it makes people more resilient and equipped to handle adversity. By strengthening this trait, psilocybin helps executives develop both inner and outer skills to lead themselves and their companies more effectively.
Psilocybin and Burnout Recovery: What to Know About Mindset and Support
While we have looked at some of the research-backed ways in which psilocybin can benefit burnout recovery, this doesn’t mean executive professionals should simply take psilocybin mushrooms on their own, without any planning or preparation.
Mindset Preparation for Psilocybin Experiences
One’s mindset (or ‘set’) when taking psychedelics can affect the quality of the experience.
Executives should make sure their levels of restfulness and personal readiness for altered states are as good as they can be. By prioritizing sleep hygiene, physical health, mindfulness, and psychedelic preparedness in the days and weeks prior to a planned psilocybin experience, one will be more ready to handle the states of mind that arise.
The focus of mindset preparation should be about understanding what is already a challenge to them in their work going into the experience, the curiosity to gain insights that can improve their leadership or show them how to change their ways, and being willing to process difficult emotions that impact how they lead and work.
For leaders who are serious about burnout recovery through psilocybin, the experience should be approached with thoughtfulness and clear intentions, rather than recreationally or casually. For burnout recovery and tangible behavior change, the right psychological underpinnings need to be in place.
According to researcher Rosalind McAlpine, psychedeic preparedness involves being ‘ready’ across four domains:
- Support-planning: Having strategies in place for handling difficult experiences; having a plan for what to do in the days following the experience; and feeling a trusting, positive connection with the people one will have the experience with.
- Intention-preparation: Engaging with preparation practices, such as meditation, yoga, breathwork, journaling, diet, and exercise; speaking with a therapist or counselor; and contemplating the reasons for taking psilocybin.
- Psychophysical-readiness: Trusting one’s mind and body to safely process the experience; feeling prepared for the physical and psychological effects; and feeling ready to surrender to the experience and for whatever comes up during it.
- Knowledge-expectation: Being aware that the quality of the psilocybin experience can change; knowing that the experience is somewhat unpredictable; understanding that events from the past could surface during the experience; knowing that a range of intense emotions can arise; and doing research into the effects of psilocybin, through reading books or articles, watching videos, or listening to podcasts.
Why Professional Support Matters in Psilocybin Therapy
At a psilocybin retreat, or during psychedelic therapy, psychological support is provided. This provides a degree of safety that is absent when using psilocybin on one’s own or with friends (who may have no experience supporting people during these types of experiences).
If it’s someone’s first time using psilocybin, and especially if high doses are being used, having a trained psilocybin facilitator or therapist can make the difference between a prolonged, distressing experience and a therapeutic breakthrough that greatly impacts burnout tendencies and leadership capacity.
If negative emotions or thoughts arise, it’s important that they are worked through with an attitude of openness, curiosity, and acceptance. With psilocybin, leaders can gain insight into everything from how early-life experiences shape their current predicament to the present complexities they face as executives.
Psychological support from psilocybin facilitators often involves guidance on how to adopt an attitude of openness during a psychedelic experience, or how to work with the sensations that arise. Psychedelic facilitators and therapists help participants feel grounded and cared for in case the experience ever feels overwhelming or highly distressing.

Executive types also tend to be highly cognitive people. Facilitators can help them connect more with their body and emotions, which is often necessary for psilocybin to be as impactful as possible. Many of the benefits of psilocybin stem from the emotions it evokes, and people need to be mindful and engaged with the sensations arising in their bodies to experience them.
Post-session support is also crucial. Retreat facilitators, therapists, or coaches can support leaders in how they process their psilocybin experiences. This gives leaders a chance to discuss what the experience meant to them and how they are beginning to see that they need to approach their work differently.
Support from someone with a similar background in leadership or an executive position is a valuable way to help a leader gain more from the experience, as their professional insight can inform decisions a leader is considering based on their psilocybin sessions.
How to Make Burnout Recovery Sustainable After Psilocybin Experiences
Psilocybin is not a cure or panacea for burnout. But it can be an important part of the solution.
Maintaining simple, healthy habits, such as regular mindfulness, good sleep hygiene, and an exercise routine, is often the best way to prevent burnout. These habits are effective at reducing stress and anxiety.
But burnout recovery is not just about external habits and lifestyle changes; it’s as much about growing as an individual to lead more effectively and better manage one’s inner resources. It’s about learning where energy is being inadvertently lost and how to better manage it going forward.
Burnout has a highly psychological component to it. Leaders and executives can develop the skills to better monitor and manage it. When insights and lessons about burnout emerge on psychedelics, these must be sustained and put into action after the experience. If a high-performing professional doesn’t integrate what they learned during their psilocybin experiences, there is a risk that they’ll fall back into negative work, lifestyle, and thinking habits.
This is where trusted support is essential. Leaders who work with a psychedelic-informed therapist or coach have an opportunity to deeply explore the insights that arose during a psilocybin experience and apply it into their role and lives. By prioritizing dialogue and communication about the experience and the work, executives can gain clarity and clear solutions to the problems they face.
Through this integration, leaders can enhance and maintain their skill sets and emotional well-being to support recovery from burnout and create a sustainable, ongoing solution to prevent its return.

Executive Burnout Recovery: How Psilocybin Can Help Leaders
The Complete Mushroom Ceremony Guide
A mushroom ceremony is an opportunity for profound healing and spiritual exploration. Taking psilocybin mushrooms in a communal, ritualized context offers a unique experience, distinct from psychedelic use in clinical or recreational environments.
We should state from the outset that a genuine, traditional mushroom ceremony is not necessarily what is offered at most psilocybin mushroom retreats. ‘Ceremonial’ use implies a type of belief structure, environment, practice, and ritual that not all psilocybin retreats adhere to.
MycoMeditations, for instance, does not offer traditional mushroom ceremonies. We offer guests guided, therapeutic psilocybin experiences in a group setting. While a mushroom ceremony shares these features, too, as noted above, it involves other features that differentiate it from many psychedelic retreats.
If you are planning to take part in a traditional mushroom ceremony, this is what you need to know.
What Is a Mushroom Ceremony? Meaning, Traditions, and Spiritual Context
There is evidence of the ceremonial use of psilocybin mushrooms from ancient Mesoamerica. The Olmec, Zapotec, Maya, and Aztec civilizations all used psilocybin as part of their religious practices. Archaeological evidence, including ‘mushroom stones’, indicates such usage occurred 3,000 years ago.
The ceremonial use of these mushrooms had multiple purposes, including communication with deities, divination, and healing. The Aztecs referred to the species Psilocybe mexicana as teonanácatl, which in the Nahautl language means “flesh of the gods”. They perceived these mushrooms as holy, a sacred substance that allowed communication with the divine.
A tradition of ceremonial psilocybin use has continued in Mexico up until the present day. Traditional Mexican mushroom ceremonies, or veladas, are nighttime rituals in which healers (curanderos/curanderas) guide participants through altered states, using specific chants, prayers, and offerings. In this tradition of Mazatec shamanism, as practiced in Huautla de Jiménez, Oaxaca, Catholic imagery often features as well.
The mushrooms are known locally as Ndí Xijtho (“little things that sprout from the ground”), or “holy children”, and are perceived as conscious, intelligent entities.
What to Expect in Your First Mushroom Ceremony: Rituals, Setting, and Experience
Not all mushroom ceremonies are alike. What you experience depends on the country and tradition in which it’s taking place, who’s leading it, and the specific rituals or practices that will be employed.
For example, if you take part in a velada in Huautla de Jiménez, you can expect:
- Recommendations to follow a “diet”, or abstinence from eating certain foods or engaging in sexual relations for some days before the ceremony.
- A sacred journey in which one is meant to enter into the “presence of God”.
- A ceremony led by a healer, referred to as chjota chijne (“wise person”), whose role is often based on lineage, traditional apprenticeship, training, and rites of passage.
- An experience that typically takes place in the healer’s home at night, with only candles used for light at the beginning of the ceremony, which are eventually put out to create total darkness.
- The burning of incense, copal, or any other aromatic materials for ritualistic cleansing.
- Prayers and petitions, which are made to God, Catholic saints, nature spirits, and deceased ancestors.
- The healer helping you navigate your visions and the healing process.
Mushroom ceremonies outside of Mazatec shamanism may involve some of these elements while including others (such as different religious or spiritual beliefs).

For example, some mushroom ceremonies may occur outside of a specific tradition or religion, but may focus on spiritual experiences, “energetic” healing, or connecting to nature. These may lean into New Age spirituality and can take place in legal and underground contexts. Ideas, practices, and music from different traditions may be used and combined. Guides may burn tobacco or sage, and use crystals, sound baths, or breathwork.
In short, a mushroom ceremony may feature:
- Active guidance from a shaman or healer
- Specific religious/spiritual beliefs
- Traditional music
- Possibly religious imagery
- Intentions that go beyond psychological healing, including physical healing, seeking knowledge of the future, and communicating with deities or spirits
How to Prepare for a Mushroom Ceremony: Mindset, Diet, and Practical Tips
Intention-setting is essential for mushroom ceremony preparation. This refers to what you specifically want to get out of the psilocybin experience, and in a traditional ceremony, it’s something that a shaman or healer will expect you to have ready to share with them.
Common intentions include:
- Healing physical or psychological problems
- Finding answers to questions about the future
- Resolving a conflict or broken relationship
- Diagnosing the spiritual or energetic roots of illnesses
- Communicating with the divine, spirits, nature, or deceased ancestors
Beyond intention-setting, wise preparation for a psychedelic ceremony should also involve:
- Packing comfortable clothing suitable for the season and climate
- Planning all travel well in advance so that there are no stressful surprises regarding transport to the ceremony
- Making sure that you don’t have any physical or psychiatric conditions or current medication usage that could interact negatively with psilocybin
- Getting enough sleep in the weeks before the ceremony, so that you feel physically and mentally rested
- Practising mindfulness and spending time in nature in the weeks or days before the experience, so that one feels calm before the ceremony
- Eating a healthy, balanced diet
- Preparing for the unknown: the experience may not fit one’s expectations or preconceived notions
- Adopting an attitude of humility and a willingness to surrender
- Being open to a potentially difficult experience at times, as well as the potential insights this may involve
What to Bring to a Mushroom Ceremony: Essential Items for Comfort and Support
It’s wise to bring personal belongings that help to create a “container” for the experience. These are any objects associated with personal or spiritual meaning, safety, comfort, or familiarity. The goal is to create a feeling of security, making it easier for one to surrender to the experience. Potentially useful items to bring include:
- A water bottle so that one can stay hydrated throughout the experience
- A journal and pen to record any important thoughts, emotions, or insights immediately after the experience
- Pictures of loved ones
- An item from childhood
- Special jewellery
- Sacred objects such as small ornaments or statues, sacred texts, images of deities or religious figures, prayer beads, or symbolic stones
How to Stay Calm Before a Mushroom Ceremony: Emotional Preparation and Grounding Techniques
Feeling ready to surrender to the wide array of psychedelic effects that can occur often involves emotionally supporting yourself before the ceremony.
We’ve already seen how preparation matters in the weeks and days leading up to a mushroom ceremony, but it’s also crucial to support yourself on the day of the ceremony, as this is often when nerves are at their highest.
To calm any nerves or anxiety before a mushroom ceremony starts, you can try a range of soothing and grounding techniques:
- Body scan: focus on physical sensations from head to toe
- Light stretching or yoga
- Deep breathing
- Progressive muscle relaxation (PMR): tense and release muscle groups starting from the feet up to the shoulders
- Listening to calming music
- Wishing oneself to have an insightful and beneficial experience
How Long Does a Mushroom Ceremony Last?
The effects of psilocybin typically last 4-6 hours, although in clinical trials, some participants experience effects up to eight hours after ingestion.
Mushroom ceremonies last longer than the acute effects of psilocybin because, before ingesting the mushrooms, time is spent:
- Preparing the mind, in which participants reflect on, write down, or discuss their intentions
- Performing “cleansing” rituals where healers may burn tobacco or incense to purify participants’ bodies
- Preparing the physical space, making it safe and comfortable for participants
- Welcoming participants into the space with music, chants, or prayers
- Honoring the mushrooms and journey ahead before consumption
- A ritualized form of consumption, in which the healer offers the mushrooms – raw, with honey, or as a tea – to each participant

After the effects of psilocybin wear off for ceremony participants, the ceremony is then formally brought to a close, often with a prayer to pay respect towards and thank the spirit world. The ceremony may also end with a closing circle to reflect on the experience along with a communal, light meal.
The Mazatec velada is a full-night affair, beginning at night and ending at dawn. The whole ceremony can last up to 10 hours. While the acute effects of psilocybin don’t typically last more than six hours, a traditional Mazatec mushroom ceremony is not considered finished until dawn.
Outside of the Mazatec context, in more New Age settings, mushroom ceremonies may last a similar or shorter amount of time, and they may also begin at a different time, too, so not necessarily finish at dawn. Indeed, some mushroom ceremonies are designed so that the effects wear off in time for participants to be able to sleep as normal.
What to Know About Integration After a Mushroom Ceremony
The term “integration” does not exist in traditional mushroom ceremonies as it does in non-ceremonial psilocybin retreats or New Age mushroom ceremonies. Rather than there being a discrete, formalized stage of integrating psychedelic insights or visions, the healer simply closes the ceremony at dawn.
After a traditional mushroom ceremony, a “diet” is often advised, involving abstinence from alcohol, pork and red meats, spicy food, black beans, and sex, lasting anywhere from 4 to 53 days. The intention here is to honor the mushrooms and secure the physical and spiritual healing received during the ceremony.
This contrasts with the Western concept of integration, in which participants process their psilocybin experiences for the purpose of psychological insight and improving mental health. This might take the form of a whole day after the dosing day, dedicated to group discussion and self-reflection, or several one-on-one sessions with a trained psychotherapist. In modern retreat and therapy settings, there are also usually no recommendations to follow any particular diet to help with integration.
As part of a traditional mushroom ceremony, the healer takes a more active role in diagnosing your problem or confirming what the mushrooms revealed, as well as providing specific prescriptions to help you, such as prayers, offerings, or community tasks you should engage in. Modern psilocybin retreats and therapy, conversely, tend to take a more non-directive approach, allowing participants to arrive at their own insights and conclusions.
How to Decide Whether a Mushroom Ceremony is Right for You
A mushroom ceremony is likely right for you if you would rather have a ritualized experience involving traditional music, singing, and spiritual beliefs and practices. For many people, the ceremonial context helps to facilitate spiritual experiences, and specifically the kinds of experiences they’re interested in, such as connection to the divine and spirits.
However, a mushroom ceremony may not be right for you if you want a more metaphysically and spiritually neutral experience, as well as a non-directive approach. You might be interested in “spiritual” experiences, but not those framed within a specific framework. For example, experiences of interconnectedness, unity, connection to nature, and communal bonding often take place in modern psilocybin retreats and can benefit people regardless of their religious or metaphysical beliefs.
If your main motivation is psychological insight, healing, and growth, then psychedelic therapy or a modern psychedelic retreat could be the ideal choice. However, if these benefits are just one potential outcome you’re interested in, and you’re curious to see what unique experiences and benefits a traditional mushroom ceremony can offer, then participating in the latter could be worth the commitment.

What to Know Before Your First Mushroom Ceremony
How to Know It’s the Right Time for Psychedelics
Choosing to take psychedelics is a big deal. When done safely and intentionally, psychedelic experiences can support real improvements in mental health and your life at large.
However, when done without proper preparation, or without feeling ready, they can pose risks.
With so much talk about the psychological benefits of psychedelics like psilocybin, ayahuasca, or ketamine in modern discourse, you may be wondering what it takes to be truly ready for the experience.
Psychedelic preparation encompasses multiple fronts, from your mindset and physical body to where you choose to take the psychedelic and the support you have around you.
In this article, we’re going to break down how you can know if you’re ready for a psychedelic experience, and what to do if you’re not ready yet but want to work towards getting there.
Why Psychedelic Readiness and Preparation Matter for Safety and Outcomes
Whatever your intention for a psychedelic experience, feeling ready is crucial to help you get the most out of it and avoid potential adverse effects.
Without readiness, you may feel overwhelmed by what comes up and unable to navigate the intensity of the psychedelic state. You may lose sight of why you decided to take the psychedelic in the first place, and come out of it feeling destabilized and unsure of what to do with what you experienced.
Psychological readiness is crucial to ensure safety. Feeling like an experience is too “big” to be able to hold can result in re-traumatization or extended difficulties, especially for people with a history of trauma and nervous system dysregulation. Many people report adverse effects following experiences they weren’t ready for.
Alternatively, when you feel ready – emotionally, mentally, and physically – you are more able to take the experience and translate it into something meaningful in your life. You are prepared for the intensity that the experience may bring and have tools to navigate whatever comes up.
You also have support around you in case you need it, and feel safe throughout all stages of the process, all the way from preparation to integration.
Here are our top signs you’re ready for a psychedelic experience.
Check Medical and Psychological Safety: Contraindications for Psychedelics
The first step to determining readiness for a psychedelic experience is making sure there’s nothing in your health history that would make it medically or psychologically dangerous.
If you’re seeking out a guided experience with facilitators or a psychedelic therapist, they should take you through a screening process to rule out any potential dangers. For all psychedelics, this should include asking about your mental health and a familial history of psychiatric conditions such as psychosis, schizophrenia, or bipolar disorder. If you have a history of more severe psychiatric illness, other therapies may be advised instead of psychedelics.
Screening, whether you do it with a facilitator or healthcare professional or through your own research, should also include physical health intake. Psychedelics like psilocybin mushrooms and ayahuasca are extremely safe physiologically for healthy individuals, but they can raise heart rate and blood pressure. People with cardiac issues should be aware of this and consult with their doctor(s).

Other medicines like ibogaine carry a higher physiological risk, especially to the heart, and should only be done in a clinical setting with continuous medical monitoring.
You should also discuss any medications you are taking with your provider. Certain psychedelics, particularly ayahuasca, pose a serious risk when combined with certain medications, especially pharmaceuticals like SSRIs and SNRIs. It can also be extremely dangerous to combine psychedelics with other substances, like opioids or alcohol.
If you are taking a contraindicated medication and wish to taper off, it’s essential you do this under the supervision of your healthcare professional. Abruptly stopping medications can be extremely dangerous. If it’s not a good idea to stop taking medication at this time, your provider may recommend a different psychedelic or alternative therapy.
Set an Intention, Not Expectations, Before a Psychedelic Experience
Once you have the all-clear on mental and physical health intake, it’s time to set your intention.
Why is it so important to have an intention for a psychedelic experience?
Whether you’re taking psychedelics in a therapeutic, intentional, or recreational context, it’s vital to understand why you’re doing it and what you want to get out of it. This helps guide the journey, enabling you to gain the insight you seek and ensuring the experience turns into real-life impact once it’s over.
Having a clear intention also acts as an anchor if the journey becomes challenging, rooting you in why it was important to you to have the experience in the first place. Intentions usually center on personal healing and growth, self-knowledge, or spiritual or transpersonal exploration.
Some examples of anchors that you take into a psychedelic journey might sound like:
“Come back to the breath.”
“Soften the body.”
“I am safe.”
“Trust and surrender.”
“Show me the truth.”
When going into a psychedelic experience, make sure to distinguish between setting intentions and setting expectations. Even with the strongest intention, it’s important to let go of any expectations of how the experience might unfold. Cultivating a sense of trust in the medicine that it will show you what you need to see will help you do this.
Sometimes this may mean more intensity, while at others it may mean more subtlety. There’s no way of knowing what’s in store. Try to let go of “wants” and avoid associating a “good” experience with lots of visions and immediate clarity.
Signs You Are Mentally and Emotionally Ready for Psychedelics
Next, it’s time to prepare your mind for the experience. Psychedelics can push us to the edge of what we feel our psyche can hold. Cultivating a positive and grounded mindset (the set in set and setting) before a journey is crucial in helping us navigate the psychedelic realms and avoid feeling destabilized once it’s over.
Engaging in activities like meditation, speaking to an integration coach or therapist, journaling, and – crucially – rest, leading up to a journey can all help you establish mental readiness for psychedelics. The goal is to cultivate a sense of surrender, acceptance, and presence in the face of whatever may come up.
Meditation in particular can help you take an observer stance toward psychological material, which is a helpful skill during intense psychedelic states.

You may also reduce or eliminate social media usage, consumption of dark or disturbing content, and screentime in general in the days leading up to your experience. This “mental diet” helps eliminate the mental clutter we accumulate through media exposure in our day-to-day lives.
Signs of mental and emotional readiness for psychedelics include having a stable sense of self, being able to feel strong emotions without shutting down or trying to escape or numb, and feeling able to tolerate uncertainty and let go of a sense of control.
If you are struggling with symptoms of severe trauma and nervous system dysregulation, it may be advised to start with a softer psychedelic experience, such as ketamine therapy, or do ample work in talk therapy before diving into a higher dose of classical psychedelics like psilocybin or ayahuasca.
The Importance of Feeling Physically Ready for Psychedelics
As well as mindset, it’s also essential to prioritize bodyset – the physical component of psychedelic readiness – ahead of a psychedelic experience.
With psychedelics (and with life), the mind and body are intrinsically linked. Many of the practices that help you feel good physically have a positive impact mentally, and vice versa.
Before taking psychedelics, it’s always a good idea to be conscious of the foods and substances you consume and anything toxic that may be going into your body. Guidelines will differ from one medicine to the next, but sticking with healthy, whole foods and staying away from processed foods is a good rule of thumb. In fact, healthy gut bacteria may even influence your experience. It also goes without saying that avoiding alcohol and other drugs is important.
Practices that connect you to your body and regulate your nervous system can help you get ready for psychedelics.This may include mindful movement like yoga, calming breathwork techniques, hot/cold therapies, grounding, and spending time in nature.

Connecting with sensations in your body and your breath during a psychedelic experience can be tremendously helpful in staying grounded and calm amidst intensity. Psychedelics amplify the current state of the nervous system, so anything that helps you enter the experience feeling calm and well-regulated will lower the chance of it being overwhelming or extremely dysregulating.
Signs of a regulated nervous system and that you’re physically ready include having consistent sleep, breathing mostly from the diaphragm, low levels of tension in the body, and an ability to self-regulate following moments of stress and anxiety.
Set and Setting Explained: Creating a Safe Psychedelic Environment
Now, it’s time to think about your setting and container for your journey. The psychedelic container is a metaphor that refers to everything that creates physical, psychological and emotional safety around your experience.
In the context of guided psychedelic sessions, the container includes not only the physical environment but the presence of trained professionals, the music, the use of shamanic or energetic tools, the boundaries and rules set by the facilitator(s), and the quality and dosing of the psychedelic medicine.
In a traditional ayahuasca ceremony, for example, the container encompasses the shaman serving the medicine, the team of helpers, the icaros, energy cleansing tools, and any pre- and post-ceremony support that participants receive from facilitators.
In a modern therapeutic context, the container would include a trained facilitator, a comfortable physical space, the preparation and integration sessions, and specific facilitation skills they may use during the journey itself.
The “tighter” the container, the more boundaries and support there are. The journeyer feels safe with the guide and has built a relationship with them, built on trust and consent.
Recreational or unguided journeys, however, usually entail “looser” containers. The physical environment may be less secure, such as a public space that’s outdoors, and those present may be trip-sitters or fellow journeyers.
If you’re considering taking a psychedelic on your own or with friends, make sure to set yourself up in a secure space where you won’t be disturbed, create a plan to reach out to a trusted friend (or at the very least, a hotline like Fireside) should you need additional support, and have a nourishing meal and safe space to rest ready for when you come out of the experience.
Whichever container you choose, safety is paramount. Make sure the medicine you’re taking is good quality and from a reliable source, and is dosed correctly. If you have any doubts about your physical or psychological safety, it’s not a good idea to go ahead with the experience.
Social Support Systems: How Human Connection Helps with Psychedelic Integration
Whatever the nature of your experience, a solid psychedelic support system is essential. Psychedelic journeys can take us to unexpected places and uncover deep-rooted psychological material that we need help to process. Even if the journey was ecstatic and illuminating, landing back into regular life can be a struggle, especially when you feel like nobody around you understands what you experienced.
You may want to book sessions with an integration coach or therapist after your psychedelic session. This can help you unpack visions and draw out the insights that you want to apply to your everyday life. A trained coach or therapist can keep you accountable and provide a safe space to process and understand your experience.
You might also seek out an integration group to connect with others who are on a similar path and share your stories with one another. These spaces provide a sense of community, support, and belonging post-psychedelic journey.
And of course, lean on close friends and family who understand why you decided to have a psychedelic experience. Tell at least a couple of trusted people before going into your session, so that in case you need extra support on the other side, they can show up for you. Human connection is critical for big psychedelic experiences.
Readiness is About Safety, Support, and Self-Awareness
If you’re still wondering whether or not you’re ready for psychedelics, you can complete this evidence-based survey to get your preparedness score.
This survey is the Psychedelic Preparedness Scale, which was developed by leading psychedelic researchers at University College London.
Ultimately, preparedness is just as much about a feeling as checking boxes. Tune into what feels true to you in your body and intuition, and start from there.
And remember: not all psychedelic experiences are created equal, and there are no rewards for jumping in at the deep end. You can always start slow and build up to stronger medicines and higher doses in time.
Curious about how science-backed, legal psilocybin mushroom retreats might help you find lasting healing? Discover our programs at MycoMeditations.
Psychedelic Readiness FAQs: Safety, Preparation, and Timing
How do I know if I’m ready for a psychedelic experience?
You can determine your psychological, physical and emotional readiness through this evidence-based survey, designed by leading psychedelic researchers.
What emotional factors should I consider before participating?
Prior to a psychedelic experience, it’s important to feel emotionally stable and regulated. You can prepare yourself emotionally through practices like meditation, breathwork, movement, time in nature, and speaking to a qualified coach or therapist.
Why are set and setting important for psychedelic experiences?
Set and setting are both crucial for a safe psychedelic experience. The set refers to your mindset going into the journey, which should be positive, grounded, and rooted in your intention. The setting refers to the physical environment around you and the people present. The physical space should be safe and comfortable, and you should ideally be guided by qualified professionals throughout. All of this helps you feel safe to surrender and open up to the experience, and avoid having a “bad trip.”
What kind of support should I have after a psychedelic experience?
Following a psychedelic journey, you may want to have sessions with an integration coach or therapist to help you process your experience, understand insights, and apply them to your daily life. You might also seek out community support through a psychedelic integration circle or from trusted friends who have had similar experiences and understand your decision to take psychedelics.
When is it better to postpone a psychedelic journey?
It’s better to postpone a psychedelic journey when there are medical, pharmaceutical, or psychological contraindications present. You should also postpone the journey if you are feeling like any aspect of the container is unsafe or not ideal for you, such as the facilitators, the surrounding group of participants, or the physical space. If you are feeling emotionally unstable, overwhelmed, or like you don’t have sufficient time and space to prepare for and integrate the experience, it is a good idea to save it for another time when you are more grounded and prepared.

Am I Ready For a Psychedelic Experience?
Essential Questions to Ask Before Choosing a Psilocybin Retreat
Before you sign up for a psilocybin retreat, it’s crucial to have already done research into the retreat you have in mind.
But what should this research look like before you book a psilocybin retreat?
To find out all the necessary details to ensure that a psilocybin retreat is reputable, safe, and ethical, one needs to ask the right kinds of questions. These are questions that someone should be able to find clear and full answers to from the psilocybin retreat website, organizer, and facilitators.
In this article, we will be covering the core questions that anyone should be asking before booking a psilocybin retreat. With these questions ready and the kinds of answers you should justifiably expect, you can feel confident about how to choose a psilocybin retreat.
Psilocybin Retreat Safety: Screening, Risks, and Medical Considerations
A safe psilocybin retreat will prioritize the physical and mental well-being of guests. This means having a screening process in place and trained facilitators who can handle the wide range of possible states of consciousness.
What Is the Screening Process for a Psilocybin Retreat?
One key aspect of psilocybin retreat safety is having an adequate screening process in place. This means retreat organizers should be asking potential guests a range of questions to see if there’s a risk of any negative reactions to psilocybin.
The screening process should check for psilocybin contraindications such as a personal or family history of specific mental health conditions (e.g., schizophrenia, bipolar disorder), current use of medications, high blood pressure, and heart conditions.
Screening also involves checking someone’s personal readiness for a psilocybin experience. This encompasses factors such as emotional stability, the ability to handle intense experiences, and the amount of psychological work a person has already done through traditional therapy.
What Are the Qualifications and Training of the Facilitators?
Part of feeling safe and supported during a psilocybin retreat involves trusting the ability of the facilitators to handle altered states of consciousness. Psilocybin experiences can involve a wide range of experiences that they must be ready for.
The perceptual, cognitive, and mystical effects of psilocybin may lead one to experience profound states of awe, bliss, and insight, as well as potentially confusion, overwhelm, and anxiety. It is safe to experience all of these alterations of mind, so long as a person feels physically and psychologically safe.
Well-trained and experienced facilitators will be familiar with the possible experiences guests can have and will have the knowledge and skills to support them through anything that arises.
Anyone interested in booking a psilocybin retreat should ask what qualifications, training, and experience the facilitators have. This might include specific higher education degrees, psychotherapy training, professional experience in the mental health sector, psilocybin therapy or facilitation qualifications, psychedelic facilitation experience, and relevant voluntary work (e.g., working for psychedelic care and harm reduction groups such as Zendo and PsyCare).
The Support Available During Psilocybin Dosing Sessions
It’s wise to find out precisely the level and type of psychological support you can expect during a psilocybin experience. This means getting clarity on how many facilitators will be present and how they respond to any challenging moments.
What Is a Safe Facilitator-to-Participant Ratio at a Psilocybin Retreat?
You’ll also want to ask how many facilitators will be present during the psilocybin sessions to provide support. Reputable psilocybin retreats will ensure that a sufficient number of facilitators are present for every dosing session.
Based on the group size, there should be enough facilitators so that if more than one person requires or requests psychological support or help, they won’t be left alone.
At the very least, a facilitator-to-participant ratio of 1:3 would be acceptable. Ideally, this is closer to 1:2 for more therapeutic retreats. Anything nearing 1:4 starts to become too low from our perspective.
Higher ratios reduce the risk of facilitators being overstretched during dosing sessions, which risks people being unsupported when they need it most. It can also lead to a feeling that the facilitators have to drift quickly without adequate time to truly be with a guest when the support is needed.
MycoMeditations has a facilitator-to-guest ratio of at least 1:1.5. This higher ratio allows us to provide the most personalized care within the benefits of group psilocybin experiences.
By asking about the facilitator-to-participant ratio, potential guests can gain a clearer sense of the level of support they can expect during their psilocybin experiences.
What Type of Emotional and Physical Support Is Provided During Sessions?
We briefly touched on the benefits of knowing a facilitator’s background. It’s useful for guests to know not just that they’ll be supported but also how they’ll be supported. Make sure to ask the retreat organizer or facilitator what approach they take during participants’ sessions. Helpful questions include:
- If touch is involved, when is there a discussion on the kinds of touch that one feels comfortable with?
- If the pre-selected music starts to misalign with the experience, how is this normally resolved?
- If one feels overstimulated or overwhelmed because of the group setting, is there a private area where one can be supported by a facilitator?
- If the effects feel overwhelming, confusing, or frightening, how do facilitators handle the situation? What might they do that helps guests move through these difficult feelings?
- If one feels physically uncomfortable, such as nauseous, hot, or cold, how can facilitators help guests feel more at ease?
Psilocybin Retreat Setting: Environment, Group Size, and Comfort
The setting in which a psilocybin retreat occurs can have a powerful impact on the quality of the experience. This covers group size and the environment in which the dosing session takes place, and the legal environment surrounding the retreat.
What is the Group Size?
Smaller groups (10–15 participants) typically mean a greater level of support and care on offer than larger ones. At MycoMeditations, psilocybin retreats typically have 8–10 guests, making them a more intimate, personalized experience. Other retreats may have upwards of 20 guests (with others supposedly reaching 100 guests).
Larger retreats, or even smaller retreats with a low facilitator-to-guest ratio, will have everyone in one room for the dosing, as this helps manage the group’s session. Some people enjoy going through these vulnerable experiences side by side with others, while others feel it doesn’t allow them to drop into the experience as deeply.
If you know you’d likely be uncomfortable being in an altered state in a large group, or you’d just prefer a more intimate experience, then it’s important to find out what the group size is before booking a psilocybin retreat.
What is the Environment for Dosing Sessions Like?
The kind of space in which a psilocybin experience occurs can affect its emotional quality. Some factors have the potential to facilitate therapeutic effects. Be sure to ask questions like:
- Does the psilocybin experience happen indoors or outdoors?
- If the session takes place in a natural setting, or there’s a view of a landscape, what is it like? What will guests be able to see and hear?
- If the dosing session takes place indoors, how is the room designed?
- How do facilitators help guests feel physically comfortable? Is it easy to comfortably sit and lie down during the experience? What do facilitators do if a guest feels too hot or cold?
- Are eye masks provided?
- What can guests expect from the pre-selected music playlist?
Is the Retreat Legally Operated?
You’ll need to confirm the legality of the psilocybin retreat before booking, so that you don’t fall prey to any legal trouble. Psilocybin retreats are legal in the Netherlands, Jamaica, Oregon, and Colorado.
However, psilocybin retreats also operate where psilocybin is decriminalized, not legalized. This means the substance remains illegal, but criminal penalties for possession and personal use are removed. While this means a psilocybin retreat is unlikely to receive interference from the law in Portugal and Spain, where psychedelics are decriminalized, this doesn’t necessarily make the retreats as safe as fully legal ones. This is because where psilocybin retreats are legal, there is often regulatory oversight ensuring facilitator training and safety protocols.
One key difference between legal and decriminalized psilocybin retreats is that the former often must comply with regulations that govern the quality of psilocybin products, screening, and facilitation.
Furthermore, many psilocybin retreats occur underground, where the psychedelic compound is illegal. If you ask a retreat organizer about the legality of the retreat and they confirm it has to operate in secrecy for this reason, proceed with caution. While many people have positive experiences at underground retreats, without any regulations, oversight, or reviews online, there is often a greater risk of negative experiences.
A legal setting provides a layer of safety, whereas an illegal, poorly prepared, and risky setting can lead to worry and unease. The legality of a psilocybin retreat is part of the social and cultural setting in which the experience occurs, so it shouldn’t be neglected.
Checking for the legality of the psilocybin retreat before booking can help you feel confident that the organizer and facilitators are reputable and trustworthy.
Psilocybin Retreat Dosing: Personalization, Dosage, and Safety
Psilocybin retreats vary in their dosing approach. It’s important to find out what approach is in place beforehand, so that you know how much you’ll be taking when the day comes. Dosing protocols also play a key role in facilitating therapeutic experiences.
Is There a Personalized Approach to Psilocybin Dosing?
Many psilocybin retreats take a personalized approach, varying them based on participants’ previous psychedelic experiences, current mental state, level of preparedness, and comfort levels. This approach can help ensure that each person achieves a desired intensity of experience, based on individual factors.
What is the Dosing Limit?
Psilocybin retreats also differ in the upper limits of the doses they are willing to work with. This is often based on facilitators’ level of experience, how much support is available, the methods and safety protocols in place, and the guest’s previous experience (if any) with psychedelics.
Are the Doses the Same Used in Clinical Trials?
At the same time, some retreats stick to the kinds of doses used in clinical trials, which will translate to a moderate dose of psilocybin mushrooms.
Using 2.5–4 g of dried moderate potency psilocybin mushrooms roughly translates to the 25 mg dose of synthetic psilocybin used in clinical trials, so this range has the potential to induce the kinds of effects that predict therapeutic outcomes, including mystical-type experiences, insights, and emotional breakthroughs.
However, some people require higher doses to experience these outcomes, as larger doses can help loosen unconscious barriers and defences that prevent people from accessing deeper, therapeutic states. Mystical experiences are also more likely to occur when higher doses are used, which is also what we observe at our retreats and see in clinical trials.
Why Preparation Matters Before Booking a Psilocybin Retreat
Preparation is an essential aspect of any safe and beneficial psilocybin retreat. Before booking, check what preparation is provided or recommended, and be sure to ask the organizer or facilitator for more details on this aspect of the experience. It’s helpful to ask about:
- Techniques for navigating altered states
- Recommended reading material
- Realistic expectations for the experience, including potential benefits and risks
- How one’s current mental state may influence the experience
- Any recommended lifestyle habits before the experience
As well as being able to guide you before you turn up to the retreat, a safe and trustworthy psilocybin retreat should also include preparation when you arrive, before your first dosing session. This might involve guidance on using an attitude of acceptance and surrender to help navigate the experience.
Psilocybin Integration Support: Questions to Ask Before Booking
Post-dosing integration sessions are also a crucial aspect of a transformative psilocybin retreat. If the website isn’t clear about the number or kind of integration included, be sure to find out:
- When integration support is included, is it soon after the dosing session on the same day, or only the day after?
- What the integration day looks like. It’s common for psilocybin retreats to give guests ample time for quiet self-reflection and time on their own, as well as for group discussions with guests and facilitators. But inquire how much time is allocated for these activities.
- The facilitators’ background in providing psychedelic integration.
Some retreats may include additional activities to help with feeling settled and to facilitate the processing of insights. Activities can include nature walks, meditation, yoga, artistic expression, and breathwork. Others will have longer therapeutic sessions for integration. Get a sense of what is planned or optional so that you are ready once you arrive at the retreat.
When the retreat is over, this is when the integration support should really be a focus. Ask whether the retreat provides or has recommendations for further integration, which might take the form of group discussion, psychedelic integration groups, educational materials for self-guided practices, or a network of psychedelic integration therapists or coaches. Any legitimate psilocybin retreat will prioritize participant safety and will have post-retreat support in place.
Making an Informed Psilocybin Retreat Booking
Booking a psilocybin retreat with confidence means being informed about what to expect from that experience. By asking the right questions, you can educate yourself about the potential effects of psilocybin and the kind and level of support, preparation, and integration involved in the retreat.
Before booking a psilocybin retreat, ensure that you feel satisfied with the information provided by the retreat company, as this is an important aspect of personal readiness. This will allow you to fully trust that you’re in safe hands, with all the help you need to have a transformative experience.

Questions to Ask Before Booking a Psilocybin Retreat
Overcome Addiction with Meaning and Purpose
According to the World Health Organization (WHO), globally, 3.5–5.7% of 15–64 year olds use illicit drugs, and between 10% and 15% of those users struggle with drug addiction or drug abuse. However, addiction encompasses more than just problematic drug use.
Addiction refers to any chronic, compulsive behaviour despite the harmful consequences that result, such as negative effects on one’s physical and mental well-being, relationships, and career.
Legal trouble may result as well, owing to the illicit nature of the activity (e.g., obtaining drugs, driving under the influence) or theft to fund the addiction. People struggling with addiction often desperately want to quit, but find they are unable to do so.
Many people are also addicted to gambling, food, sex, porn, the internet, and video games. All of these can lead to surges in dopamine, a chemical involved in the brain’s “reward system”, which is associated with motivation and reward. When these activities are excessively pursued, they can hijack this reward system: one feels compelled to keep engaging in these behaviors, despite the harm that follows.
Sometimes, the consequences of addiction are fatal. WHO has found that, worldwide, over 3 million deaths are due to alcohol and drug use. Addiction increases this risk due to overdose, drug adulteration, health complications, and suicide.

Many habit-forming drugs, such as opioids, quickly increase tolerance, meaning higher doses are needed to achieve the desired effect. Since addiction involves chronic, compulsive use, the buildup of tolerance can lead people to start taking potentially fatal doses, where overdose becomes a possibility.
That said, there are many evidence-based addiction recovery tools, which can help people either beat addiction or prevent relapse, but one type, which is often neglected and undervalued, is finding meaning and purpose in life.
As you will see, meaning and purpose are core addiction recovery tools. When a life is lived with these values in mind, many people find they no longer experience a compulsion to cope with emotional pain through addiction, or even if an old compulsion arises, they have an anchor to keep them from giving in to that impulse.
What Are Addiction Recovery Tools and How Do They Work?
Addiction recovery tools refer to evidence-based methods that help individuals achieve and maintain long-term sobriety.
What this long-term sobriety looks like can vary from person to person. While some may find abstinence from all drugs is necessary for avoiding harmful patterns of drug use, others may find that only avoiding one or more drugs is necessary for achieving this.
Common addiction recovery tools include:
- Cognitive behavioral therapy (CBT)
- Support groups such as SMART Recovery, Narcotics Anonymous (NA), Alcoholics Anonymous (AA), Sex Addicts Anonymous (SAA), and Gamblers Anonymous (GA).
- Regular exercise
- Mindfulness-based treatment
- Motivational interviewing
- Trauma-based therapy, which helps to address the childhood wounds or traumatic events experienced in adulthood that lead to addiction
- Psychedelic-assisted therapy
Why Meaning and Life Purpose Strengthen Addiction Recovery
The addiction recovery tools noted above can all be critical in helping people recover from addiction and stay sober. Resolving negative thought patterns, remaining more rooted in the present moment, enhancing well-being through exercise, finding support from others, and addressing trauma can all make recovery more likely and relapse less likely.
But finding a sense of meaning and purpose in life contributes to this goal as well. This is because meaning and purpose are fundamental human concerns. Research has found that both help people achieve sustained emotional well-being. They also protect people from experiencing psychological distress.

Meaning refers to a feeling of significance and coherence, a feeling that one’s life matters and that one can make sense of one’s life. In contrast, purpose is focused on a forward direction; it refers to an overarching goal or motivation in one’s life. However, both meaning and purpose are connected, as pursuing a long-term project can contribute to a feeling that life is characterized by significance and coherence.
Through their positive effects on mental health, meaning and purpose help protect people from becoming overwhelmed and distressed by negative thoughts and emotions, which an addiction may have helped to soothe.
The Science Behind Purpose-Driven Recovery
We have promising evidence to support the idea that meaning and purpose act as effective addiction recovery tools:
- A 2011 study published in the Journal of Substance Abuse Treatment found that purpose in life predicts positive treatment outcomes for cocaine abusers.
- In a 2025 study published in Alcoholism Treatment Quarterly, researchers note that meaning and purpose in life are essential aspects of recovery from alcoholism.
- A 2022 study published in Psych revealed that meaning-making processes are central to addiction recovery. These processes involved participants reinterpreting their past suffering or trauma, viewing their survival or recovery as having a purpose, and the development of a new identity (e.g., helping others).
- A 1986 study published in the Journal of Clinical Psychology highlights that purpose in life is linked to a lower likelihood of substance abuse.
How Addiction Disrupts Meaning, Purpose, and Identity
Addiction disrupts the ability to find genuine and fulfilling meaning and purpose in life by redirecting one’s attention to drug use. Addiction can become the primary focus in one’s life, due to how much time is spent craving a drug or activity, and building one’s life around engaging in it. Finding meaning and purpose through self-development, a career path, a life project, or helping others often gets sidelined in the process.
Addiction often negatively affects one’s sense of identity as well. Research has found:
- Identifying strongly as a “drinker,” “smoker,” or “drug user” is associated with a greater frequency of use and more severe addiction. When drug use becomes part of one’s identity, recovery can be more difficult, as continued drug taking is a way for people to reinforce their self-concept.
- People who experience addiction report losing their valued social roles or identities (e.g., worker, student, parent). Addiction creates a narrow identity centered on drug use, which results in the loss of identities that previously provided a sense of meaning and purpose in life.
- Addiction can result in a discontinuity of self, which is when there is a conflict between one’s past identity and addiction-centered identity. It involves the feeling that one is no longer the same person, which can lead to an identity crisis.
- Stigma surrounding drug use and addiction can reinforce a shame-based “addict” identity, which may affect treatment engagement, self-esteem, and willingness to seek help.
Rebuilding Identity as a Core Addiction Recovery Tool
Research has consistently shown that addiction recovery involves not just stopping drug use but developing a new sense of identity. Successful recovery involves replacing the “drug addict” identity with an identity based on being a non-user, in recovery, and positive roles influenced by relationships and community.
When researchers examined residents in addiction treatment centers, they found that those who identified more strongly with a recovery-based identity than an addiction-centered identity showed a greater commitment to sobriety, higher levels of psychological well-being, and lower emotional distress.
The link between rebuilding identity and recovery has led other researchers to propose a Social Identity Model of Recovery (SIMOR). This model suggests that adopting a recovery identity is crucial for successful outcomes. Being part of recovery communities – support groups like 12-step programs – helps reinforce a new, positive identity and sustain abstinence.
How to Integrate Meaning and Purpose into Addiction Recovery
There are many ways in which meaning and purpose can act as addiction recovery tools. What a meaningful, purposeful life looks like during recovery or post-addiction can vary between people.
But it’s also common for people struggling with addiction to imagine what such a life looks like. This is because addiction can involve unrealistic, limiting, distressing, or hopeless thoughts such as “I need drugs to feel happy,” “My life is ruined,” “I’ll always be an addict,” or “The future has nothing in store for me.” To combat these kinds of thoughts, which frustrate efforts to get sober, it’s important to see the possibilities that lie ahead, or how one’s life can be rebuilt after addiction.
With this in mind, here are some practical ways people can integrate meaning and purpose into their addiction recovery:
- Identifying and living in accordance with core values. These might include honesty, kindness, creativity, and family.
- Setting and pursuing meaningful long-term goals. These will vary between people, but they may come from education, hobbies, career accomplishments, and creative projects.
- Connecting with others. We’ve already seen how addiction support groups can create a strong sense of meaning and purpose, but other forms of community can foster this too, such as voluntary work, as well as spiritual, religious, and political communities.
- A sense of spirituality. Many addiction recovery programs and groups emphasize the role of spirituality as a source of meaning and purpose, and how this facilitates recovery. While for some, spirituality may fit into a religious framework, in the form of religious worship and prayer, for others, it may involve a meditation practice, connecting to nature, personal growth, or psychedelics.
Common Psychological Barriers to Finding Meaning and Purpose After Addiction
In an ideal world, it would be easy to identify what a meaningful and purposeful life looks like after addiction and have the resources in place to swiftly actualize it. However, several barriers can get in the way of this goal:
- Anhedonia. It is common to experience difficulty in feeling pleasure from normally pleasurable things after addiction. Anhedonia is often what drives many people to addiction as a strategy for feeling the pleasure one is lacking in life. Without the drug, the anhedonia remains. However, if anhedonia is a symptom of underlying depression, treating the depression may return the ability to experience pleasure, making recovery easier.
- Shame and guilt. Addiction can drive people to do things they regret, such as lying, stealing, or hurting others emotionally or physically. Post-addiction, this may lead to persistent feelings of shame and guilt, keeping one stuck in the mindset of “I’m a bad person.” However, this is why a core aspect of addiction recovery is making amends, as well as rebuilding an identity based on self-compassion and a more positive, realistic sense of identity.
- Leaving a social circle behind. People struggling with addiction may have formed a close-knit social circle based around using. To get sober typically means leaving this social circle behind. This can be challenging for two reasons: firstly, the potential guilt of “abandoning” one’s friends, and secondly, the possibility that one has no healthy social circle to return to. Nonetheless, sober and recovery groups, as well as many other communities, exist as positive forms of social connection.
Why Meaning and Purpose Sustain Long-Term Recovery
As we’ve seen, finding meaning and purpose in life is an essential addiction recovery tool. It is an evidence-based way to achieve sustainable recovery. A sense of living a meaningful and purposeful life is what helps motivate people to quit as well as remain free from the shackles of addiction in the long term.
By prioritizing meaning and purpose in addiction recovery, those who have struggled with addiction will be able to discover a fulfilling life not dependent on temporary highs. Once discovered, a life lived well and meaningfully becomes something worth protecting, and free from the influence of addiction.

Finding Meaning and Purpose as Core Addiction Recovery Tools
How Psilocybin Therapy May Help Heal Childhood Trauma
Childhood trauma significantly increases the risk of various mental health conditions in adulthood, and for many people, it can also lead to issues such as addiction and relationship problems.
It is estimated that 62.8% of US adults have been exposed to an adverse childhood experience (ACE). ACEs are not identical to trauma. The latter is the emotional distress in response to ACEs, which can leave a lasting mental, physical, and behavioral impact.
ACEs are potentially traumatic events, with the most common types being emotional abuse, parental separation, household member substance use, physical abuse, a household member living with a mental illness, witnessing intimate partner violence, sexual abuse, and parental incarceration. One in four people in the US has experienced four or more ACEs.
Because the wounds of childhood trauma are deep, healing from it is often a long and emotionally difficult process. Many individuals who have experienced childhood trauma live with chronic or treatment-resistant depression.
Trauma-based therapies can offer people much-needed relief, but these treatments, as well as conventional medications, don’t work for everyone. There may be no response, inadequate relief, or, in the case of certain medications, troubling side effects that lead to discontinuation.
Addressing childhood trauma with psilocybin-assisted therapy is gaining widespread recognition as a novel treatment that avoids many of the pitfalls of traditional approaches. Psilocybin experiences, when combined with trauma-informed therapy, can facilitate a powerful emotional healing process. In this article, we’ll explain why.
Why Researchers Are Exploring Psilocybin-Assisted Therapy for Childhood Trauma
There are many reasons why researchers are interested in psilocybin-assisted therapy for healing childhood trauma.
Tackling Treatment-Resistant Mental Health Conditions
As already mentioned, some mental health issues don’t respond well to treatments. However, it’s important to note that this typically refers to conventional treatments, sometimes specified as when someone tries at least two antidepressants without adequate benefit (in the case of depression).
It is estimated that 30% of people with depression have the treatment-resistant form. For treatment-resistant PTSD, the figure is 33%. But, as well as medications failing to offer substantial relief from symptoms, traditional talk therapy can be inadequate for many as well.
This is not to discount, of course, the fact that psychiatric medication and various types of psychotherapy can help people with trauma-related conditions experience an alleviation of their symptoms. Nonetheless, patients with a history of childhood trauma show poorer responses to psychotherapy and pharmacological treatment.
Healing childhood trauma with psilocybin-assisted therapy is promising because it has shown an impressive efficacy in treating treatment-resistant forms of depression. The treatment appears to be effective at facilitating the processing of emotional pain, attachment wounds, and relational difficulties in a deeper or more catalyzed fashion than traditional treatments.
Limitations and Side Effects of Conventional Trauma Treatments
Traditional medications can help alleviate symptoms related to childhood trauma and can be incredibly beneficial and sometimes life-saving for many people. However, despite potential benefits, unwanted side effects may occur as well. The most common ones include nausea, weight gain, insomnia, dry mouth, blurred vision, sexual dysfunction, emotional blunting (or emotional numbness), and withdrawal effects when discontinuing use too quickly.
Psilocybin-assisted therapy may involve some uncomfortable effects as well, such as nausea, headache, and temperature fluctuations. However, these are acute effects, which last only during the session itself.
In contrast, the side effects of daily use of psychiatric medication may be more of a constant challenge for people to deal with.
The Rapid Healing Potential of Psilocybin Therapy Sessions
Another difference between traditional mental health treatment and psilocybin-assisted therapy, which attracts interest from researchers, is the major difference in the amount of treatment involved.
Many people who are on a journey to healing childhood trauma may be in therapy for years. Similarly, people struggling with the effects of childhood trauma may use antidepressants daily for years. Again, this commitment to treatment often yields positive results: a significant alleviation of symptoms and the ability to live a functioning, fulfilling life.
But we also know that this journey may involve a lot of trial and error, with talking therapies, therapists, and various medications (and doses) failing to provide adequate benefit in the short term.

While psilocybin therapy is often considered expensive, it can cost someone the same amount as long-term psychotherapy. And if the latter doesn’t provide substantial or lasting benefit to someone, the additional time engaged with psychotherapy may be unnecessary in certain circumstances.
In contrast, research has shown that one or two therapeutic psilocybin sessions, alongside several preparatory and integration sessions, can provide significant and (crucially) lasting relief. Three dosing sessions can provide even further benefits, as evidenced by data gathered from MycoMeditations psilocybin retreats.
Mental health benefits from psilocybin-assisted therapy can last up to 12 months, and sometimes longer for many people; although it is worth noting that some patients do also see a return of symptoms. In these cases, follow-up psilocybin or trauma integration sessions may be helpful.
In any case, researchers so far find it encouraging that the time commitment involved in psilocybin-assisted therapy, lasting a matter of weeks, could provide such long-lasting benefits.
Proposed Mechanisms: How Psilocybin Therapy May Help Process Trauma
The evidence so far for the use of psilocybin for addressing childhood trauma is promising. The authors of a 2023 study concluded that this treatment “may feasibly help in supporting survivors of adverse childhood experiences with particularly strong benefits to those with more severe childhood adversity.”
Researchers have suggested multiple ways that psilocybin therapy can be helpful for healing childhood trauma. These mechanisms tend to work together, offering a multi-leveled approach, which is often needed in cases of deeply rooted or complex trauma.
Reductions in Experiential Avoidance and Increased Emotional Connection
A 2020 study found that reductions in experiential avoidance – the avoidance of challenging emotions – predict decreases in depression severity following psilocybin therapy. Avoiding trauma-related memories or emotions is a common response to trauma. It is an understandable response and coping mechanism. However, it can get in the way of processing the emotional pain associated with the traumatic event(s).
The authors of the study note, “We conclude that integrating psychedelics with psychotherapeutic interventions that target experiential avoidance (e.g., ACT) may enhance therapeutic outcomes.”
Reductions in experiential avoidance can also be helpful in the context of post-psilocybin trauma therapy, as this can make people more open to discussing the resurfacing of traumatic memories and emotions associated with it.
Other researchers discovered, similarly, that psilocybin therapy enhanced patients’ connection to their emotions, and this predicted therapeutic outcomes. A follow-up study from one of Imperial College London’s trials on psilocybin therapy for depression found that patients contrasted this benefit from psilocybin with the emotionally disengaging effects of antidepressants.
A Unique Way of Engaging with Childhood Trauma
Facing childhood trauma can be extremely challenging at times. It can bring up intense feelings about oneself and the person or people whose actions led to the trauma. This is why traditional treatments may be slow. Emotional triggers and avoidance are common barriers to successful treatment.
Psilocybin-assisted therapy for healing childhood trauma often works because it involves a unique way of confronting this kind of trauma. Traumatic memories, sometimes played out vividly or symbolically, can arise. While challenging at times, when professional psychological support is involved, psilocybin therapy clients often report a deep processing of the emotional pain.
As a participant in a 2025 study on psilocybin therapy for PTSD said, in relation to difficult memories that arose, “And it was … intense, but it felt … productive … it felt like, it was necessary somehow … that kind of … physical … element … releasing a lot of emotion.”
The authors of the study write:
“The treatment facilitated an experience of both direct and indirect engagement with trauma-related material during psilocybin treatment. Unlike standard treatments requiring direct confrontation with trauma memories, psilocybin appears to enable a broader, indirect engagement with traumatic material via a range of affective, somatic and self-transcendent experiences (e.g., moments of perceived unity, dissolution of self, or felt connection with a larger whole).”
Rebuilding Self-Worth After Childhood Trauma
Childhood trauma is associated with rumination, low self-esteem, and feelings of unworthiness and shame later in life. When trauma occurs in childhood, as the brain is going through major developments, the sense of self can be negatively impacted.
This maladaptive way of relating to oneself can extend well into adulthood, where one believes one is fundamentally unworthy, not good enough, or a bad person. This low self-worth is not just a risk factor for conditions like depression, but also suicidality.
Healing childhood trauma with psilocybin-assisted therapy also seems to work by addressing negative self-talk and self-image. Studies have found that psychedelics can effectively alleviate trauma-related shame, guilt, and self-condemnation. Psychedelics, including psilocybin, can do this by fostering emotional states such as self-acceptance, self-compassion, and self-forgiveness.

By reducing self-criticism and enhancing a more positive relationship to self, psilocybin-assisted therapy can help heal the emotional wounds of childhood trauma. This doesn’t erase the wrongs done or the memories of the trauma. But it does enable a person to have a healthier sense of self that can cope with the past, live more mindfully in the present, and thrive in adulthood, despite what happened to them in childhood.
Risks and Ethical Considerations in Psychedelic Trauma Therapy
The recalling of childhood trauma during psilocybin therapy presents unique risks and ethical considerations. Some patients felt their well-being worsen as a result. This is why adequate and sometimes more extensive trauma-informed and evidence-based therapy is required in conjunction with psilocybin therapy and post-session. Therapists must minimize the risks of re-traumatization as far as possible.
While 22% of people recalling childhood trauma during psychedelic experiences reported re-traumatization, which is not a tiny minority, it’s important to note these experiences often occurred outside the context of supervised and supported psychedelic therapy. Researchers emphasize:
“Participants who experienced trips alone without any guide or subsequent therapy show how a lack of support can leave someone to cope with the fallout on their own, potentially worsening trauma symptoms. Conversely, those who actively engaged in integration work through psychotherapy, journaling, meditation, support groups, or deep personal reflection are more likely to report that they transform their challenging experiences into healing”.
One ethically sensitive issue related to psilocybin therapy is the emergence of apparently long-suppressed and forgotten childhood trauma. As Saga Briggs writes for Big Think:
“Psychedelics have also been shown to increase suggestibility and enhance false memories — effects that understandably raise suspicions about retrieved memories, similar to suspicions in the “memory wars” of the 1990s, a series of debates on the scientific validity of repressed memories, uncovered trauma, and the perils of memory recovery therapy.”
This creates a challenge for psychedelic therapists about how to handle experiences of “forgotten” trauma emerging during sessions. The authors of a 2025 paper argue:
“Clinicians and researchers should indeed refrain from confirming (or dismissing) the accuracy of reported memory experiences if they do not have outside corroborating information. While confirmation is problematic, dismissal or overt skepticism is also not appropriate and may cause harm by, e.g., disrupting the therapeutic relationship.”
This aligns with the non-directive approach to psychedelic therapy that clinicians, therapists, and ethicists deem most appropriate and ethical. This means therapists don’t force their interpretations onto the client, but rather let them discover the meaning of their experiences that are most helpful to them.
Psilocybin is a Powerful Catalyst, But It’s Not a Standalone Solution
It’s crucial to keep in mind that psilocybin therapy for healing childhood trauma doesn’t work only through the psilocybin sessions. Experiences of emotional connection, self-compassion, and catharsis are, of course, important aspects of successful treatment, but so is trauma-informed and evidence-based therapy.
Post-session trauma-informed and evidence-based therapy helps to minimize the risks of re-traumatization by giving clients space to process any difficult emotions that arose or which still remain after the sessions.
Lastly, a focus on the integration process that follows psilocybin therapy is key to deepen and continue exploring new positive beliefs, thoughts, and feelings going forward, while mending trauma following a psilocybin session.
By sustaining these healthier ways of relating to oneself, psilocybin therapy serves as an unmatched catalyst to help people heal the wounds of the past.

Healing Childhood Trauma with Psilocybin-Assisted Therapy
The Ways That Psilocybin May Impact Inflammation
Inflammation is the body’s natural response to injury or infection. It involves immune cells reaching a damaged part of the body, which leads to tell-tale signs of inflammation such as redness, swelling, heat, and pain. It is a defense mechanism, and one which is crucial for healing.
Yet, while temporary inflammation is curative, chronic inflammation, lasting months or years, is linked to various diseases. One sign of the latter is persistent pain. It is an aspect of conditions such as diabetes, arthritis, autoimmune diseases, inflammatory bowel disease (IBD), and fibromyalgia.
Research has found that 34.6% of US adults suffer from systemic inflammation, meaning that they have widespread inflammation in the body, which often results in chronic pain. However, systemic inflammation is not always painful: poor diet, lack of exercise, and a sedentary lifestyle can lead to a low-grade, body-wide type of inflammation without pain. Although this does increase the risk of chronic pain.

Other symptoms of low-grade, systemic inflammation can include persistent fatigue, digestive issues, skin problems, insomnia, and mood changes.
Treating inflammatory conditions (painful or otherwise) can be challenging. Non-steroidal anti-inflammatory drugs (NSAIDs) are a conventional strategy, but they can come with side effects, and long-term use can increase the risk of heart attack, stroke, kidney damage, and high blood pressure.
However, alternative anti-inflammatory options exist. Psilocybin is one novel compound that is showing promise as a safe and effective way to reduce inflammation.
In this article, we’ll be exploring why researchers are studying the use of this psychedelic for inflammatory conditions, as well as proposed mechanisms, and what the evidence does (and doesn’t) currently tell us.
What Is Chronic Inflammation and Inflammatory Pain?
Inflammation occurs when the body releases immune cells, such as cytokines, in response to injury, infection, or irritation. These cells fight off pathogens and repair damaged tissue. The release of immune cells into damaged tissue causes swelling, which puts pressure on nearby nerve cells, thereby resulting in pain.
With inflammatory conditions, this immune response doesn’t turn off. This leads to persistent inflammation and, in turn, chronic pain.
Causes of chronic pain conditions include acute injuries, autoimmune diseases (where the immune system mistakenly attacks healthy tissue), lifestyle factors, stress, and chronic infections.
Inflammatory pain conditions vary. Where the pain occurs depends on where the inflammation is happening.
For example, inflammation in the joints is associated with rheumatoid arthritis, gout, and ankylosing spondylitis; when in the muscles, tendonitis and fibromyalgia can result; while in the digestive tract, chronic inflammation is tied to irritable bowel disease (IBD).
But again, pain is just one aspect of inflammation, and it’s not always present. In the above conditions, for example, people may experience fatigue or weakness in the related areas of the body, or persistent diarrhea and unexplained weight loss (in the case of IBD).
Furthermore, in cases of systemic inflammation, the symptoms may not be localized in a specific area or system of the body. Because lifestyle factors that create more widespread inflammation, the symptoms may therefore be more numerous and diverse. And, for some people, this kind of inflammation doesn’t always result in pain, or at least not severe or chronic pain.
Why Researchers Are Exploring Psilocybin for Reducing Inflammation
There are many reasons why researchers are interested in the use of psilocybin as an alternative way to reduce inflammation:
- Many people are not helped by conventional anti-inflammatory treatments. As a novel treatment, psilocybin acts in different pathways in the body compared to NSAIDs, for instance. This could help explain why it provides unique forms of relief for people.
- Psilocybin is non-toxic. Acute and long-term use are not associated with negative health effects.
- Low, non-psychedelic doses of psilocybin may also help reduce inflammation, which would make widespread application of the treatment easier. While we recognize the manifold benefits of the altered states produced by psilocybin, the use of psychedelic drugs without such effects can still hold therapeutic value.
Proposed Mechanisms: How Psilocybin Might Reduce Inflammation
Below are several ways in which psilocybin reseaech has signalled it’s potential to possibly help reduce inflammation.
5-HT2A Receptor Activation and Anti-Inflammatory Effects
Research has found that psilocybin produces long-lasting reductions in inflammatory pain in mice, via activation of 5-HT2A receptors. Researchers behind this 2025 study state:
“Our results demonstrate that a single administration of the classical psychedelic psilocybin can reverse pain-like evoked behaviors in two mouse models of chronic pain between 6 and 14 days. However, the effects of DOI lasted only up to 24 h in the same models. Despite differences in the time-course of efficacy, the antinociceptive [pain-reducing] effects of both psychedelics seem to be mediated via 5-HT2AR-dependent signaling. Furthermore, the effects of psilocybin and DOI in our studies are not specific to a nociceptive modality since they were active in mechanical, cold, and thermal responses.”
They add that “the anti-inflammatory effects of psilocybin and DOI may be a contributing factor to their analgesic-like properties.” This indicates that just a single dose of psilocybin may alleviate chronic pain by reducing inflammation, and more so than other psychedelics, such as DOI. The authors also state:
“Since the spinal expression and levels of 5-HT2AR subtypes are increased in chronic pain models such as chronic inflammation, neuropathy and CIPN [chemotherapy-induced peripheral neuropathy], it is possible that the single administration of psilocybin and/or DOI in our models reduce pain-like behaviors by decreasing 5-HT2AR subtypes in the spinal cord and other brain regions as reported in animal studies.”
Another 2025 study echoes these findings: psilocybin’s activation of 5-HT2A receptors is correlated with reductions in inflammatory pain, as well as decreased anxiety and depression, conditions also influenced by inflammation.
The Mind-Body Connection: How Mental Health Affects Inflammation
Psilocybin’s ability to alleviate conditions like depression, anxiety, and PTSD may also contribute to its anti-inflammatory potential. These mental health conditions are not only influenced by inflammation; they are also associated with further increases in it. This is why an anti-inflammatory approach to depression can be effective, and also why reducing inflammation can occur when one addresses emotional pain on a psychological level. In other words, psilocybin therapy may have beneficial downstream effects on our physiology.
For many people, psilocybin can address the psychological factors behind inflammation, which may manifest as pain and/or other physical symptoms. By helping people process and overcome issues like negative mood, rumination, and trauma – all linked to increased inflammation – psilocybin may exert an anti-inflammatory effect.
Recovering From Chronic Stress Through Neuroplasticity
In addition, many mental health conditions result from chronic stress. Through its neuroplastic effects, psilocybin could counteract stress-related brain changes, which would be helpful not only for alleviating emotional distress but also for inflammation. Stress-related brain changes highlight again how poor mental and physical health are connected by similar causes.
Since evidence suggests that psilocybin can correct maladaptive neural pathways, which are influenced by chronic stress, this is another potential way it can enhance both psychological and physical well-being.
Psilocybin for Reducing Inflammation: Study Limitations and the Need for More Research
While there are several studies indicating that psilocybin reduces inflammation, it’s also important to highlight the research gaps:
- Reliance on pre-clinical (in vitro) models. Studies have found that psilocybin reduces inflammation in human cell cultures, but this doesn’t capture the complexity of the whole human body. Inflammation, after all, is related to many different systems, interactions, and processes.
- The limitations of animal models. Psilocybin can reduce liver inflammation in mice. However, most animal studies involve acute inflammation, not the sort of chronic inflammation that many people deal with. In addition, while mouse models are useful indications of what could be helpful for people, rodent immune systems still differ from those of humans.
- Limited human clinical data. A placebo-controlled study showed that psilocybin decreases inflammation in participants, but the study involved a small sample size and healthy volunteers, so the results may not translate to those with chronic inflammation.
- Some conflicting evidence. One study found that psilocybin had no significant positive change on inflammatory markers. Nevertheless, we should note that this study involved healthy volunteers, so this evidence may not count against the use of psilocybin for treating inflammatory conditions.
The gaps and limitations in the research tell us that more work needs to be done in this area.
However, the evidence and proposed mechanisms so far are a highly promising start. The burgeoning research on psilocybin indicates that psychedelics have applications beyond the psychological, and it shows too how deeply tied our mental and physical well-being are.
FAQs About Psilocybin and Inflammation
What is inflammation, and when does it become a problem?
Inflammation results from immune cells being sent to fight off pathogens or repair damaged tissue. This increase in immune cells in the damaged area causes blood vessels and tissue to swell, intruding on nearby nerves, resulting in symptoms like pain, swelling, and redness. Acute inflammatory pain is normal and a sign of healing. When it’s chronic, however, it can become a source of persistent pain or other distressing symptoms such as fatigue, difficulty sleeping, poor mental health, digestive issues, and weight loss or weight gain.
Why are researchers interested in psilocybin and inflammation?
Researchers are interested in studying psilocybin for reducing inflammation because there is promising pre-clinical evidence, as well as animal studies and some clinical data, showing its efficacy. Moreover, psilocybin has a better safety and side effect profile compared to long-term use of some conventional anti-inflammatory drugs, such as NSAIDs.
What limitations exist in current inflammation research surrounding psilocybin?
Imitations in the research on psilocybin and inflammation research include a reliance on pre-clinical (in vitro) data, animal models, and clinical data involving small sample sizes and healthy volunteers.
Why is it important to avoid overstating medical claims about psilocybin’s effects on inflammation?
It’s crucial not to exaggerate claims about psilocybin’s use for reducing inflammation, as research in this area is in its infancy. The best way we can legitimize and explore the potential of psilocybin’s potential broad applications, such as for inflammation, is to continue rigorous research until medical claims can be proven. That said, it is helpful to mention the positive signals when they present themselves through research. Future studies and trials may provide more robust evidence about psilocybin’s efficacy for various types of inflammation, as well as the mechanisms involved.
Can Psilocybin Reduce Systemic Inflammation and Inflammatory Pain?
The Complete Comparison of MDMA vs Psilocybin Therapies
Many people compare MDMA vs psilocybin therapy, as these are two of the main psychedelic therapies being researched to address mental health challenges.
However, they differ in a variety of ways: effects, therapeutic models, the type of preparation and integration required, safety considerations, and legality.
We’re going to be unpacking all of these differences to help you pick which of the MDMA therapy or psilocybin therapy best suits your needs and preferences if you’re interested in psychedelic therapy.
Why People Compare MDMA vs Psilocybin Therapy
The ‘psychedelic renaissance’ refers to the resurgence of scientific research into psychedelic compounds for therapeutic purposes, as well as increased public interest in these experiences.
Two of the main compounds studied as part of this renaissance, which the public is increasingly interested in for therapeutic application, are MDMA and psilocybin.
MDMA is often derived from safrole oil, found in the sassafras tree, whereas psilocybin is the psychoactive compound found in a range of Psilocybe cubensis mushrooms.
These two compounds both emerged into mainstream culture in the last century, and also became looped together in prohibition.
Modern research has brought both of these compounds back into conversation as serious therapeutic interventions, with important differences between them to understand.
MDMA vs Psilocybin: Clinical Research and Primary Uses
Many people compare MDMA vs psilocybin because there is a wealth of research supporting their use to alleviate certain mental health conditions. Nevertheless, this research differs in terms of the conditions focused on for each medicine.
While both MDMA and psilocybin can treat a variety of conditions – often the same ones – much of the research on psilocybin therapy has focused on depression, whereas much of the intrigue around MDMA therapy is based on its success in treating PTSD.
Of course, there is evidence showing that psilocybin can be helpful for PTSD symptoms and that MDMA therapy can alleviate depressive symptoms. However, because MDMA and psilocybin therapy differ in terms of research and clinical focus, this inevitably leads people to compare the two psychedelic therapies to see which one is most relevant to their psychological needs.
MDMA vs Psilocybin: Different Chemistry and Neurological Effects
The other major reason people compare MDMA and psilocybin is that they are substances with vastly different qualities.
First, MDMA is a phenethylamine, which is a family of drugs that can include stimulants, entactogens/empathogens, and psychedelics. MDMA can encompass all of these effects, producing stimulation, enhanced emotional connection and openness, and minor psychedelic effects.
MDMA is sometimes categorized as a non-classical psychedelic. Mescaline is another phenethylamine, but it’s a classical psychedelic with more typical psychedelic effects like color enhancement and visual distortions.
Psilocybin, like mescaline, is also a classical psychedelic, but it’s not a phenethylamine. It’s a tryptamine, which means it contains an indole ring structure and is structurally similar to the amino acid tryptophan.

Because of their differences in chemical structure, MDMA and psilocybin affect receptors in the brain differently. As researchers in one paper highlight:
“MDMA is a potent monoamine releaser that produces an acute euphoria in most individuals but it is not considered a classic psychedelic, as psilocybin is. Direct 5-HT2AR stimulation is the defining pharmacological property of classic serotonergic psychedelics, but relative to classic psychedelics, MDMA has a far weaker affinity for the 5-HT2A receptor”.
The key monoamines released by MDMA include serotonin, dopamine, and norepinephrine, whereas the primary effects of psilocybin are attributed to how psilocin, the compound left behind after psilocybin is metabolized in the body, directly activates serotonin 5-HT2A receptors, as well as many other receptors.
How MDMA-Assisted Therapy Works for PTSD and Trauma
As we’ve seen, MDMA is an entactogen/empathogen. This means it reliably produces a feeling of empathy and connection to others, feelings of love and friendliness, and emotional openness. MDMA tends to help people talk openly about their thoughts and emotions, and also allows people to approach aspects of their mind that they normally can’t access.
These empathogenic effects are a main driver of the therapeutic effects of MDMA therapy.
For example, people living with PTSD find it incredibly difficult to revisit and discuss traumatic memories. To try and engage with traumatic material is highly distressing for these people, and can lead to a trauma flashback or re-traumatization.
However, the qualities of MDMA allow clients who experience the therapy to feel safe, and this heightened comfort allows them to revisit and talk about trauma in a way that is otherwise blocked off and unavailable, or even potentially unsafe. This safe access point to traumatic material allows people to process trauma in substantial ways.
MDMA’s ability to enhance feelings of connection and trust results from the release of oxytocin: a chemical involved in bonding and feelings of love. This is especially important in the context of MDMA therapy because it involves working with a therapist. The therapeutic alliance – the feeling of trust and emotional openness with a therapist – predicts success in psychotherapy.

Understandably, PTSD can make people feel distrustful and closed off around others. By softening these barriers and defences, MDMA can allow people to see their therapist as truly trustworthy and as someone they can honestly confide in. This emotional openness creates a strong therapeutic alliance.
In other words, MDMA can catalyze a process that may take years, or not happen at all, in regular psychotherapy.
Beyond PTSD, the ability of MDMA to reduce fear and anxiety applies to social situations as well, which also makes MDMA therapy useful for the treatment of social anxiety.
Because of the unique effects of MDMA, there is often more active, psychotherapeutic work during MDMA therapy sessions than there is for psilocybin. This might involve therapeutic dialogue about how the client feels or what’s coming up for them during the session.
Active psychotherapy during MDMA therapy is more helpful than it is for psilocybin therapy because the client is more likely to have their cognition intact, which allows them to have more complex spoken dialogue with the therapist.
How Psilocybin Therapy Works for Depression and Mental Health
We can now contrast the approach to MDMA therapy described above with psilocybin therapy. Since psilocybin is a classical psychedelic, resulting in distinct receptor activity, this leads to entirely different effects than those produced by MDMA.
As a 5-HT2A receptor agonist, psilocybin disrupts brain networks to a greater degree than MDMA. This includes disruption of key brain regions such as the default mode network (DMN), an interconnected brain system that is most active during rest, such as when people are daydreaming, thinking about the past, and planning for the future. It is also involved in the sense of self.
Research on depression has found that distinct activity in the DMN is associated with rumination. In other words, when the activity of this brain system increases, this is correlated with more rigid, negative thinking about the past, the future, and oneself. Other studies echo these findings.
As Chou et al. note in a 2023 study, “Individuals at-risk for depression therefore may have an underlying neurocognitive vulnerability to use a brain network typically involved in thinking about oneself to preferentially ruminate about negative, rather than positive, information.”
Psilocybin therapy helps treat depression, for instance, by disrupting this overactive DMN. It dampens DMN activity. This deactivation allows brain regions to communicate more freely, which is associated with the increase in openness and the reduced mental rigidity observed in psilocybin therapy.
This break from the rigid patterns of rumination that a person has become used to allows for new and healthier perspectives on the past, future, and present to emerge. These changes in psychological flexibility are also shown to continue long after the psilocybin dosing sessions are over.
This occurs because of psilocybin-induced neuroplasticity: the ability of the brain to form new neural connections.
Researchers believe this is what makes psilocybin therapy such a promising treatment for depression, as it helps unstick people from inflexible thought processes and beliefs.
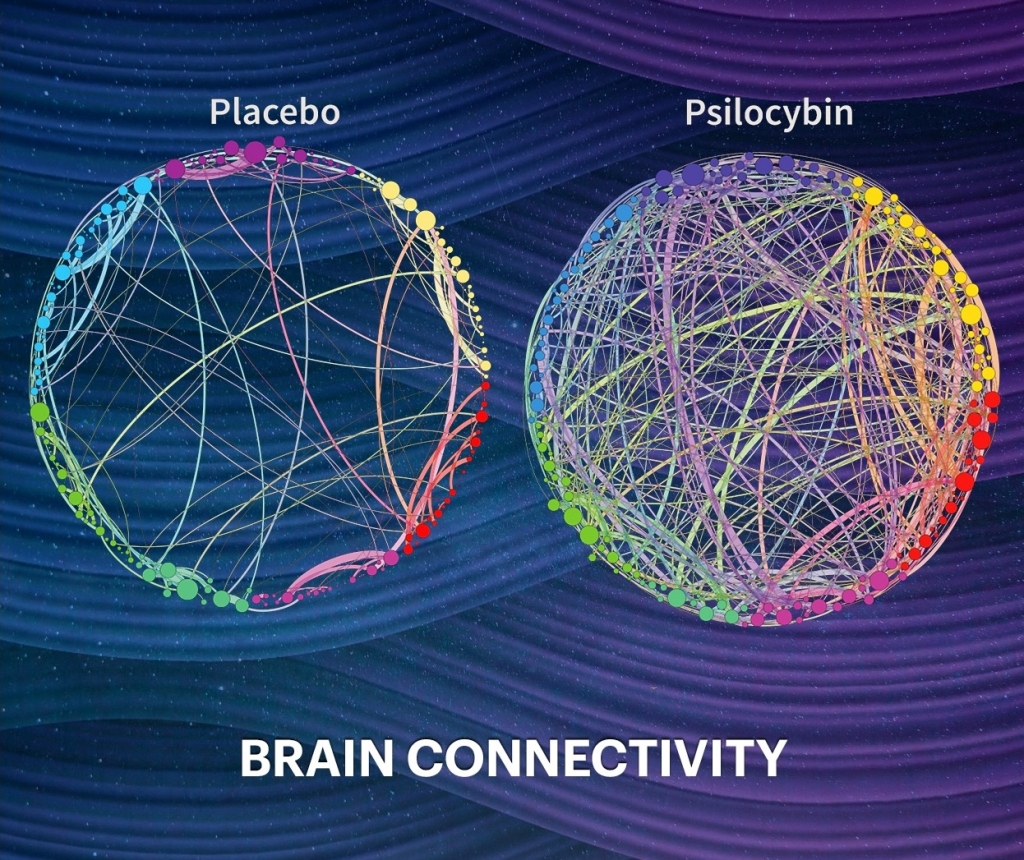
For example, philosopher Chris Letheby has argued that psychedelic therapy works because it helps people revise their current models of self, shifting them from beliefs such as “I’m broken” to more positive and realistic self-models.
Another major distinction of psilocybin vs MDMA is the particular way it unearths unconscious material. This is due to psilocybin’s unique ability to disrupt the DMN. When brain regions that are normally disconnected suddenly exchange information with each other, the unconscious parts of a person’s mind rise into conscious awareness.
Mike Ljubsa, an owner of MycoMeditations, says, “It’s like the mind is free to put everything back where it belongs to find a healthy equilibrium. This means new thought processes take over to metabolize and process the blockages that stand in the way of that equilibrium.”
The ability of psilocybin to induce ego dissolution, more reliably than MDMA, is also what facilitates this processing of unconscious material emerging. This is because the ego creates defenses to avoid confronting what we find most painful, distressing, or shameful. To confront these patterns means losing control and facing uncertainty, which our ego will always resist.
Through softening or dissolving the ego, psilocybin catalyzes people’s ability to confront and heal their negative, unconscious beliefs, emotions, and memories.
In contrast to MDMA therapy, psilocybin therapy tends to involve less talking during the session. The role of the therapist is more to represent safety, warmth, and support through their presence. They are there to provide guidance and empathic listening if the client needs it, but for the most part, the therapist and client do not talk and interact as actively as they do during MDMA sessions.
For this reason, the nuances of body language and non-verbal communication are especially important with psilocybin therapy.
What a MDMA Therapy Experience Feels Like
Here are some of the unique effects of MDMA that differentiate MDMA therapy from psilocybin therapy:
- Lower fear and anxiety, and increased euphoria.
- MDMA encourages people to feel connected to others and feel comfortable with social interaction around both familiar and new people.
- MDMA often leads to experiences where a person more deeply appreciates another person they’re with, including their personal qualities, the relationship they have together, and how this person enriches their life.
- The pro-social, pro-bonding, pro-intimacy effects of MDMA can translate into a desire for forms of physical touch such as hugging and hand holding.
- Increases in trust, which can catalyze the therapeutic process through a strong therapeutic alliance and emotional openness.
- Feeling warm or hot, rather than experiencing chills.
- Sweating
- Bruxism (jaw clenching)
- Enhanced pleasure from tactile sensations, such as touching soft fabrics or skin-to-skin contact, which can feel grounding and increase connectedness to others in the case of human touch.
- Physical euphoria may help people reconnect to their bodies and stay rooted in the present moment.
MDMA experiences last 4-6 hours.
What a Psilocybin Therapy Experience Feels Like
As well as producing classic psychedelic effects like visual distortions and mystical experiences, psilocybin experiences often differ from MDMA experiences for the following reasons:
- Transient anxiety is more common, as well as uncomfortable moments that might result in fear or overwhelm. However, when worked through, these sorts of emotions can be sources of insight and growth.
- Psilocybin experiences are more emotionally unpredictable.
- Deeply introspective states, involving subjects beyond the personal and emotional, can occur, relating to existential, philosophical, spiritual, or metaphysical topics.
- The experience is less conversational. During psilocybin therapy, clients immersed in the experience don’t tend to be as talkative.
- More of an inward experience, as psilocybin therapists encourage clients to focus their attention inwards. This helps clients work through a lot of psychological material in a single session.
- Nausea, during the onset phase, is more common.
- Body heaviness is more common.
- Some people experience chills.
- It is less common for people to desire physical touch, hand holding, hugging, etc., except in cases involving psychological support from the therapist.
Like MDMA, psilocybin experiences last 4-6 hours.
MDMA vs Psilocybin Therapy: Treatment Structure and Environment
MDMA therapy is currently in a clinical setting. In MDMA therapy clinical trials, treatment sessions occur in a hospital, clinic, or research facility, although the room is still designed to be aesthetically pleasing and calming.
The same applies to psilocybin therapy clinical trials. People can lie down on a bed or couch, and typically, mood lighting, artwork, and plants are present.
Outside of a research context, legal MDMA therapy, available in countries such as Australia, also occurs in this kind of clinical setting.
Legal psilocybin therapy, however, can occur in a greater variety of settings, due to differing legislation and regulations.
For example, in US states such as Colorado and Oregon, psilocybin therapy is offered in a non-clinical context. It takes place in healing centers, which look more like a wellness center than a clinical environment.
Legal psilocybin therapy can also be delivered in group or private retreats, like those organized by MycoMeditations.
Structure-wise, however, there are many features common to MDMA-assisted therapy and psilocybin-assisted therapy:
- Multiple preparation sessions so that clients can set their intentions and goals, as well as learn what can occur during the experience and how best to navigate it.
- Multiple integration sessions so that clients can process, make sense of, and apply their experiences.
- In a research context, there are two therapists/facilitators (one male, one female) during the dosing sessions. However, outside of a research environment, there may just be one therapist/facilitator present, or more than two in the case of a psilocybin retreat.
- Often, there are two dosing sessions, typically with a 1-5 week gap between them..
- Clients can lie down with an eye mask and listen to a pre-selected playlist, which helps to enhance inward-focused, insightful, and transformative experiences.
- There is an emphasis on trying to “trust, let go, and be open”. Trusting the medicines being used makes an incredible difference in outcomes.
Nonetheless, even though both MDMA therapy and psilocybin therapy involve preparation and integration sessions, this doesn’t mean these sessions look the same.
Psilocybin vs MDMA: Preparation for Psychedelic Therapy
Because psilocybin experiences tend to involve more intense and unpredictable altered states, to prepare for them, there is usually a greater emphasis on developing an attitude of acceptance and surrender, as well as preparing for ego dissolution or existential themes to emerge. The therapists try to prepare the client for a deep journey into unknown terrain.
In contrast, MDMA therapy preparation tends to be more trauma-focused. This means focusing on building a strong therapeutic alliance, identifying the relevant trauma and any triggers, clarifying relational patterns, and establishing some grounding skills. This preparation helps people feel safer when addressing trauma during dosing sessions.
MDMA vs Psilocybin: Psychedelic Integration
Integration for psilocybin or MDMA therapy doesn’t always differ that widely. This is because integration focuses on translating altered states into lived changes. These psychological and lifestyle forms of integration apply to both.
Given that MDMA therapy is most commonly used for the treatment of PTSD, integration may tend to focus on these themes. MDMA experiences can be helpful to build a new relationship to trauma going forward, with integration themes such as cultivating sustained openness, nervous system regulation, and self-soothing.
Integrating psilocybin experiences may also involve re-evaluating one’s relationship to the past, as well as cultivating a healthier, more growth-oriented outlook. Yet, what makes psilocybin therapy distinct from MDMA therapy, integration-wise, is that it often involves making sense of more intense, abstract, or symbolic altered states. For example, psilocybin can produce mystical unity, ego dissolution, archetypal imagery, existential insights, and profound feelings of joy and bliss that require their own attention afterwards.
MDMA vs Psilocybin Therapy: Screening and Safety Considerations
The exclusion criteria for MDMA or psilocybin therapy, based on safety considerations, can vary depending on the study in question. For example, for a phase 3 clinical trial of MDMA therapy for severe PTSD, the study notes:
“Exclusion criteria consisted of primary psychotic disorder, bipolar I disorder, dissociative identity disorder, eating disorders with active purging, major depressive disorder with psychotic features, personality disorders, current alcohol and substance use disorders, pregnancy or lactation, and any medical condition that could make receiving a sympathomimetic drug harmful due to increased blood pressure and heart rate, including uncontrolled hypertension, history of arrhythmia, or marked baseline prolongation of QT and/or QTc interval.”
Psilocybin therapy studies often include most of these same exclusion criteria as well. It’s possible that, due to its more powerful mind-altering effects, psilocybin may be riskier for those prone to psychosis or bipolar disorder than MDMA is.
MDMA, because it elevates heart rate and blood pressure more than psilocybin, may involve an elevated heart risk for those with an underlying heart condition. Nonetheless, most MDMA and psilocybin therapy studies still screen equally for both these psychological and physical risks.
MDMA carries a greater physical risk compared to psilocybin, whereas the risks of psilocybin are more psychological in nature. With chronic, high-dose MDMA use, researchers have raised concerns about increased neurotoxicity (i.e., damage to serotonin-releasing neurons).
Nonetheless, MDMA therapy is limited to 2-3 sessions, which minimizes the risk of neurotoxicity. Moreover, MDMA-related neurotoxicity has also been associated with use in hot, unventilated environments, which doesn’t apply to MDMA therapy sessions.

Psilocybin is more often associated with challenging experiences and extended psychological difficulties compared to MDMA. The latter refers to issues outlasting the session, such as feelings of existential confusion, destabilization, or social disconnection.
However, it’s important to note that challenging experiences are correlated with better outcomes when they’re supported. Indeed, many people who have had difficult psilocybin experiences found these to be profound sources of meaning, spirituality, self-insight, and personal growth.
Crucially, without adequate screening, preparation, psychological support, and integration, the risk of distress related to psilocybin experiences increases, both during and after sessions.
While the more intense mind-altering effects of psilocybin can result in challenging experiences, with the right treatment protocols and structure in place, these experiences can be transformed into positive change.
Legal Status and Access: MDMA vs Psilocybin
Psilocybin-assisted therapy is legal in more countries and jurisdictions than MDMA-assisted therapy is. The latter is currently only legal in Australia and Canada. Psilocybin therapy, in contrast, is legal not just in Australia and Canada but also in New Zealand, Colorado, Oregon, and soon in New Mexico.
But, as we can see, neither MDMA therapy nor psilocybin therapy is widely legal and accessible. However, there is active legislation seeking to legalize psilocybin therapy in more US jurisdictions, as well as efforts, which have faced some obstacles, to get MDMA therapy FDA-approved. So, in the near future, these psychedelic therapies could be more widely available.
How to Decide Between MDMA and Psilocybin Therapy
Both MDMA and psilocybin can offer people therapeutic altered states of consciousness.
However, while both kinds of experiences may help treat similar mental health problems, MDMA therapy is considered most effective for the treatment of PTSD, including severe, chronic, and treatment-resistant PTSD.
In contrast, there is strong evidence supporting the use of psilocybin to alleviate depression, including severe, chronic, and treatment-resistant depression.
But, this doesn’t mean that people with PTSD should only consider MDMA therapy, or those with depression should only consider psilocybin therapy. Emerging evidence shows a wider application of both MDMA therapy and psilocybin therapy. The former has successfully treated alcoholism, while the latter has also been helpful for those with OCD and anorexia.
As well as considering what the latest research says, often people will make decisions based on the level of risk they’re comfortable with, legal and access considerations, and the kinds of effects they feel most prepared for.
By understanding how MDMA and psilocybin differ in terms of these factors, it becomes a lot easier to decide on which psychedelic treatment is the best fit for you.
FAQs About MDMA vs Psilocybin Therapy
How do MDMA therapy and psilocybin therapy differ?
MDMA therapy tends to be more focused on the treatment of PTSD, whereas psilocybin therapy tends to have wider applications, although much research attention has been on the treatment of depression. During dosing sessions, due to the effects of MDMA, people tend to talk and interact more with the therapists present than they do during psilocybin therapy.
What types of experiences are associated with MDMA therapy and psilocybin therapy?
MDMA therapy is associated with highly empathic, prosocial, and emotionally open experiences, whereas psilocybin therapy more reliably produces mystical experiences, as well as stronger visual effects like color enhancement, visual distortions, geometry, and visions.
How are MDMA-assisted therapy sessions structured?
MDMA-assisted therapy sessions, like psilocybin therapy sessions, involve the client taking the dose in the presence of two therapists (one male, one female) in a clinical context. When the effects take hold, clients typically lie down with eye shades on and listen to a pre-selected playlist, featuring music to facilitate deeply emotional and insightful experiences. The therapists are there to provide emotional support and an empathetic ear if the client needs it.
What role does integration play after psychedelic therapy?
Integration sessions help people process and make sense of what they experienced, as well as explore how best to apply the insights and lessons of the experience to their ongoing attitudes, beliefs, path in life, sense of self, and relationships. Integration is crucial for sustaining and enhancing the mental health benefits of psychedelic therapy.
How should someone decide between MDMA therapy and psilocybin therapy?
Someone can decide between MDMA and psilocybin therapy based on the problem they deem most important to address, the drug effects and level of risk they feel most comfortable with, and which treatment will be most accessible and affordable to them.

MDMA vs Psilocybin: Differences Between Psychedelic Therapies
A Complete Psilocybin Mushroom Ceremony Guide
Psilocybin-assisted therapy has hit headlines over the last several years, thanks to the mounting number of clinical trials proving its therapeutic potential for conditions like depression and end-of-life anxiety.
But the ritualistic use of “magic mushrooms” doesn’t just go back decades, or even centuries. Some argue that these mushrooms have been part of sacred human healing and divination rituals for millennia.
Today, Indigenous cultures still exist that practice traditional psilocybin mushroom ceremonies. In Mexico, communities such as the Mazatecs and Zapotecs continue to hold these powerful rituals, rooted in ancestral wisdom of how to use sacred mushrooms to support mental, physical, and spiritual healing.
What really happens inside these ceremonies? And how can we engage with Indigenous traditions in a culturally responsible way?
In this article, we’ll dive into:
- The origins of psilocybin ceremonies
- Traditional Indigenous mushroom ceremonies in Mexico
- What really happens inside the ceremony
- Safety protocols in a legitimate mushroom ceremony
- The rise of New Age mushroom ceremonies
- Cultural responsibility and mushroom traditions
The Origins of Psilocybin Ceremonies
Evidence suggests that humans have been using mushrooms in rituals since ancient times. In the Guatemalan highlands, archeologists have uncovered stone sculptures shaped like mushrooms, with human and animal faces carved on the stems. Researchers suspect that they were a large part of Mayan culture within their religious ceremonies, where hallucinogenic fungi played a major role.
In Spain, Psilocybe-like mushrooms appear in ancient pictographs, also alongside large animals, potentially implying shamanic meaning. Archeological excavations in Algeria have also revealed mushroom figures within ancient petroglyphs, which some researchers associate with shamanic ceremonies.
In Mexico, a fifteenth- or sixteenth-century manuscript depicts “gods and sacred entities associated with mushroom rituals” in Mesoamerican culture. Spanish colonial records also detail the Nahua culture’s ritual, therapeutic, and divinatory uses of psilocybin mushrooms.
Traditional Indigenous Psilocybin Mushroom Ceremonies in Mexico
Across several indigenous communities, especially in Oaxaca, Mexico, curanderos and curanderas use psilocybin mushrooms in nighttime ceremonies, often referred to as veladas.
The Mazatecs are the best-known Indigenous group that uses psilocybin mushrooms. María Sabina, the first person to introduce the Western world to psilocybin mushroom ceremonies, came from a Mazatec community in Hautla de Jiménez, a town in the Sierra Mazateca region of Oaxaca.
The Zapotec peoples of Oaxaca are also known to have cultural practices using psilocybin mushrooms, as well as the Nahuas, Matlatzincas, Chatinos, Chinantecs, Mixes, and Mixtecs.
Traditional mushroom ceremonies in these communities are deeply embedded in the cosmovision, language, and ethics of those groups. This annotated bibliography, which looks at 49 texts concerning Indigenous practices with psilocybin mushrooms, established that ceremonies are intentionally held for healing, diagnosis, and/or divination by experienced healers – not for recreation or pure curiosity.
Healers may use the mushrooms to identify the cause of illness and the correct treatment, find answers to problems in their community, and communicate with non-ordinary intelligences, such as saints, ancestors, and elements of nature.

Mushrooms are treated as sentient beings and must be approached with humility and reverence. According to these traditions, using them irresponsibly could result in loss of visions, illness, or going mad.
“The ability to heal and communicate with sacred entities is considered a granted gift and implies a permanent commitment to the community and the divinities,” writes Osiris Sinuhé González Romero, PhD., a researcher on the history and philosophy of psychedelics.
“Among the Mazatec people, these wise people are the chjota chijne…To be a chjine is a whole ritual process that takes years and implies responsibility and commitment.”
What Happens Inside a Traditional Psilocybin Mushroom Ceremony
While mushroom ceremonies might seem mysterious from the outside, they are carefully structured and timed, and include the use of several shamanic tools for energetic cleansing and divination.
Maria-Heleyna YeiXochipahtli is a French Canadian ceremonial guide who has been working with mushrooms for over 30 years. She apprenticed with Maria Sabina’s daughter, Apolonia, for 13 years until her passing, living and studying for 7 of those years continuously in Huautla de Jiménez.
Maria-Heleyna offers both group and individual ceremonies rooted in the Mazatec mushroom tradition across North and South America and in Europe.
Maria-Heleyna always opens her ceremonies with a blessing with flowers, a candle, and copal (sacred smoke that comes from burning tree resin). “I learned how to read candles and the copal, which tells me a lot about how a person is, who’s in their lineage, or the spirits around the person,” she explains.

She then offers the medicine, dosing each person intuitively. She passes around a tobacco paste for people to put on their hands and body to “direct the energy of the mushrooms to the extremities of the body” and heal certain parts of the body. She also performs energy cleansings with an egg.
Then follows silence. Maria-Heleyna always does her ceremonies at nighttime when the “energy is quieter,” and neighbors are asleep. “After, I start to do some incantations and prayers. I speak the mushroom language and help them go to where they need to go. I bring a container of light, good energy, harmony, love, and call in angels and guides,” she says.
“I don’t talk much, and the people don’t talk between themselves or touch each other. It’s a very personal, inward journey.”
Participants may experience states of profound emotional processing, psychological insight, and feelings of connection to the universe or nature. Many will also see colorful visions in the form of geometric patterns and spiritual imagery.
“I give personal healing therapy to some of the patients during the ceremony. I cleanse the eyes with the egg, for example, or I do a special treatment on the body,” she adds.
In the morning, when participants wake up, she opens a sharing circle to be able to “wrap things up and put things in context.” Following this circle, she recommends not talking about the experience in the ceremony for 40 days. “No talking, no writing, no painting, keep it completely inside.”
This is an interesting contrast to modern approaches to psilocybin therapy, where processing and sharing your experience in the days and weeks following it is encouraged.
She explains that, “if not, it converts itself into postcards – mental analysis – and you lose the full perspective. It’s really about the art of keeping it for yourself and integrating.”
Safety Protocols in a Legitimate Mushroom Ceremony
As with other sacred medicines and psychedelics, mushroom ceremonial guides should conduct a process of screening and preparation before accepting anyone into their ceremonies.
This is the case especially for ceremonies held with people from outside Indigenous communities, who are more likely to be taking medications or have complex psychiatric conditions that should rule out psilocybin mushroom consumption.
For Maria-Heleyna’s participants, she instructs no substances, alcohol, and sex for four days before and four days after the ceremony. She also has her group participants fast for 24 hours beforehand, and her 1:1 clients fast for 72 hours prior.
She provides ceremony preparation and integration support on either side of the ceremony to ensure folks have clarity around their intention going in, and can safely “land back” into their lives afterwards.
Safety in mushroom ceremonies also requires a careful eye on ethics on the part of the guides.
Psychedelics put individuals in a vulnerable and susceptible state, making these spaces ripe for ethical missteps and abuse. Guides who haven’t undergone proper training, position themselves as a “guru,” violate physical boundaries, and engage in inappropriate relationships with the people they’re supporting are a no-go.
Anyone considering attending a mushroom ceremony should vet the facilitator or guide by asking about their background and training, seeking recommendations and references from people they trust, making sure they are trauma-informed, and following their gut if something feels off.
The Rise of New Age Psilocybin Mushroom Ceremonies
With the recent boom in popularity of psilocybin mushrooms, “New Age” style ceremonies have emerged. Facilitators, often Western, may combine elements from different traditions with modern spiritual tools to create a new kind of guided psychedelic experience.
This might look like using sound bath and crystals alongside tobacco and other sacred smokes. Guides might combine breathwork techniques into the mushroom experience, play the native drum and sing traditional chants, or even offer other medicines in the same ceremony, such as sweat lodge or MDMA.

While they may be well-meaning, it’s important to be discerning about facilitators offering mushroom experiences that are not rooted in traditional knowledge or modern clinical practice.
Many of these groups integrate elements from different Indigenous cultures without having truly studied and apprenticed with those communities. For example, they may use sage to smudge the ceremony space without a proper understanding of the plant’s cultural significance or having ever been taught how to smudge properly. This is considered cultural appropriation by many Indigenous folks.
Ethics and Cultural Responsibility in Psilocybin Mushroom Traditions
While guides have a responsibility to be in cultural reciprocity with the Indigenous traditions they practice, participants play an important role in maintaining an ethical relationship to these traditions, too.
Anyone taking part in a traditional mushroom ceremony, or traveling to the Sierra Mazateca in the hope of an “authentic” experience, should reflect on how to do this in a culturally respectful and ethical way.
Following New York banker R. Gordon Wasson’s photo essay on his experience taking mushrooms with María Sabina in Huautla de Jiménez in 1955, tourists flocked to the village with expectations of having their own experiences with the niños santos.

In a panel discussion with Chacruna, Mexican anthropologist Sarai Piña Alcántara explains:
“Since the arrival of the ‘güeros,’ as gringo tourists in Huautla are called, psychedelic and neo-shamanic tourism has emerged. Since the 1960s, people from different countries, social classes, and academic backgrounds have visited the area in order to spend an evening with the “little ones that sprout” and interact with a “true shaman.” Many arrive in the region with idealized concepts about the Mazatecs and their evening rituals.”
What has followed is the commodification of veladas and a commercial market for mushrooms in the region, explains Sarai. This has led to a shortage of mushrooms over the last 15 or so years. Hauatla is also seeing an influx of neoshamans and New Age facilitators looking to learn ceremonial techniques to offer outside of the region, she adds.
If you’re considering traveling to take part in a traditional mushroom ceremony, you may want to reflect on the following questions:
- Has the guide gone through the proper training and received the blessing to lead ceremonies from the community?
- How might my presence as a visitor affect the local community, economy, and ecology?
- What assumptions or romanticized ideas am I bringing about Indigenous cultures or “shamans”?
- What responsibility do I have after the experience – to the people, the place, and the tradition itself?
Finally, you may also want to consider why you are seeking a traditional ceremonial setting in the first place. Does it come from a genuine desire to build a relationship with the tradition? Or is it due to mere curiosity or the perceived benefit of “going to the source”?
Most Westerners will resonate more with – and get more out of – a modern therapeutic setting that better resonates with their own background, cultural context, and frame of worldview. Traditional ceremonies aren’t necessarily the ‘best’ way of working with psychedelics for everyone. What matters is how you can make sense of these psychedelic experiences within your own life and integrate them afterwards in a helpful way.
Psilocybin Mushroom Ceremonies: A Living, Ancient Tradition
As more than simply being altered state experiences, psilocybin mushroom ceremonies are intentional rituals that call for experienced and responsible guidance. While modern science and New Age spirituality are reshaping how many people encounter psilocybin, these ancestral practices remind us of the importance of intention, respect, and integration when communing with psychedelic medicines.
At MycoMeditations, despite having a non-ceremonial approach to our psilocybin retreats, we hold these Indigenous lineages and their practices in great reverence and gratitude. Without them, we recognize that we wouldn’t have access to the healing power and wisdom of psilocybin mushrooms in today’s world.
FAQs About Psilocybin Mushroom Ceremonies
How are psilocybin mushroom ceremonies structured?
Psilocybin mushroom ceremonies usually open with a sharing of the participants’ intentions and an energetic cleansing ritual, such as using copal or tobacco smoke. Then, participants ingest the mushrooms and settle into their space to wait for the effects to begin.
There may be music throughout or only during certain parts, either with live instruments or played through a speaker. Traditional Indigenous mushroom ceremonies may only include songs and chants. Once participants are out of their journey, they have some time to relax and perhaps share what they experienced before closing the ritual.
What safety measures are used in legitimate mushroom ceremonies?
Legitimate mushroom ceremonial guides should always take you through a process of intake and preparation before providing you with mushrooms. This means ruling out any pharmaceutical, medical, or psychological contraindications and providing the necessary support so you feel ready for the experience.
During the ceremony, the guides should show trauma-informed care, ethical practice, and knowledge of spiritual and energetic protection to keep participants safe. Following the journey, they should be available for anybody who may be struggling to integrate or process their experience, or who is feeling destabilized in the aftermath.
Why is integration important after a psilocybin mushroom ceremony?
Integration is crucial after any psychedelic ceremony to ensure you can process the experience and apply the insights you received to your everyday life. This may look like receiving support from integration practitioners, attending integration circles, and taking the time and space to sit with what came up and embody what it means to you.
Who should consider–or avoid–a psilocybin ceremony?
People who are seeking psychospiritual exploration or to improve aspects of their mental health may consider a psilocybin ceremony.
Individuals who are feeling psychologically destabilized or have a history of psychiatric conditions such as bipolar disorder, schizophrenia, psychosis, or borderline personality disorder, as well as those with serious cardiovascular conditions, should not take psilocybin mushrooms. Psilocybin is also contraindicated with certain medications, such as lithium or MAOIs.
















