A Complete Comparison Guide for Ketamine vs Psilocybin
Ketamine and psilocybin are two popular compounds that can be used in a therapeutic context. Ketamine therapy and psilocybin therapy are proving useful for the treatment of mental health conditions such as depression, anxiety, addiction, and PTSD.
Yet, while both ketamine and psilocybin can induce profound alterations in consciousness, there are still several important distinctions between the two compounds. In this article, we’ll be unpacking these differences, which will cover the origins of these compounds, their mechanisms, the key distinctions between the experiences they offer, and much more.
Why People Compare Psilocybin vs Ketamine
People often compare ketamine with psilocybin because they both alter states of consciousness, have been studied alongside one another through the psychedelic renaissance, as well as alter brain activity and structure in ways that can alleviate psychological distress.
In the science of psychedelics, ketamine and psilocybin are two of the main compounds that researchers are interested in that have the potential to offer people significant and lasting mental health benefits. But as we’ll see, when we compare research on ketamine and psilocybin, mental health outcomes of ketamine therapy and psilocybin therapy differ in some ways.
Another reason people compare ketamine vs psilocybin is that the therapeutic application of them is legal in several countries and jurisdictions, and people are curious see which might be better for their needs.
This means that people have the opportunity to visit legal, safe, and regulated ketamine clinics and psilocybin retreats and service centers. However, the application of ketamine therapy is not exactly the same as psilocybin therapy, as the setting and procedures will often be quite different (with some similarities, as well).
People also compare psilocybin and ketamine because they are highly popular in recreational, spiritual, and therapeutic contexts (outside of legal settings). Psychedelic users who have experience with both will naturally recognize the unique effects and notice how they differ. Many people will prefer one effect over the other, often depending on the context.
Origins of Ketamine vs Psilocybin: Synthetic vs Natural Compounds
Ketamine, unlike psilocybin, is synthetic in origin. Ketamine was first synthesized in 1962 by Calvin Stevens and was considered an excellent short-acting anesthetic. It was originally created in the hopes of finding an anesthetic like phencyclidine (PCP), without the side effects of PCP (such as prolonged delirium). Unlike, say, LSD, which is originally derived from naturally occurring ergot fungus, ketamine is made entirely through laboratory processes.
Throughout the 1960s, ketamine continued be used as an effective anesthetic. In 1970, the FDA approved it as an anesthetic, which was available to the general population under the trade name Ketalar. In the 1970s, ketamine was widely used for surgical anesthesia in the Vietnam War.

Psilocybin, in contrast, is natural in origin and is much older than ketamine. Researchers believe it first evolved in mushrooms around 65 million years ago, with scientific hypotheses on its purpose focusing on its role as a deterrent, such as deterring insects from feeding on psilocybin mushrooms. Researchers speculate it could do this through appetite suppression or disorienting effects.
Some even suggest psilocybin arrived on Earth through panspermia. This scientific hypothesis encompasses different theories:
- Naturalistic Panspermia: Life on Earth may have originated elsewhere in the cosmos and eventually reached our planet by chance.
- Directed Panspermia: Life on Earth may have been deliberately seeded by intelligent extraterrestrial beings.
- Intelligent Design: Life on Earth may have emerged from conditions deliberately engineered by advanced extraterrestrial intelligences.
As radical as these theories appear to be, many users of psilocybin give this serious consideration, given its indescribable effects at high doses.
However, we don’t know definitively or precisely how psilocybin benefits mushrooms that contain it. But we do know that psilocybin first emerged long before humans ever existed, and most researchers don’t consider it to be a useless byproduct of fungal metabolism. While we don’t know exactly why it originated, many scientists believe it was likely related to the predators found in psilocybin mushrooms’ ecological niche, whereas figures such as Terence McKenna proposed it may have arrived from outer space.
How Ketamine vs Psilocybin Work: Differences in Brain Mechanisms
While ketamine and psilocybin alter consciousness, they do so through different means. Psilocybin metabolises into psilocin when ingested; psilocin then attaches itself to multiple receptors, but is thought to primarily cause psychedelic effects by activating serotonin 5-HT2A receptors. Ketamine, on the other hand, causes psychoactive effects by blocking NMDA (glutamate) receptors.
Both ketamine and psilocybin work to improve mental health on multiple levels:
- Psychological
- Spiritual
- Neurological
Let’s take a look at these three different levels of explanation to show us the ways in which ketamine and psilocybin differ.
Psychological Effects of Ketamine Therapy vs Psilocybin Therapy
Researchers believe that the benefits of ketamine may partly derive from the shifts in mindset and perspective that can occur during ketamine experiences. Since ketamine induces altered states of consciousness, people may gain new perspectives on themselves and the emotional problems they’ve been struggling with. Other researchers have similarly stated that the integration of insights in ketamine-assisted therapy strongly contributes to mental health benefits.
The psychological effects of psilocybin, according to research, are considered to be a strong predictor of therapeutic outcomes. In one paper, the authors conclude that insights on classic psychedelics (such as psilocybin) may be a stronger predictor of therapeutic benefits than mystical-type experiences. (For clarity, they define insight as “a sudden change in understanding or perspective that feels true or reliable”.) Researchers have found that subjective effects are less likely to mediate the benefits of ketamine compared to psilocybin.
Spiritual Experiences on Ketamine vs Psilocybin
Both ketamine and psilocybin can induce mystical experiences. And these experiences – of ego dissolution, unity, sacredness, and ineffability – are associated with improvements in clinical depression and anxiety.
While ketamine can induce intense mystical experiences, it does so less frequently than with classic psychedelics like psilocybin. Therefore, if mystical experiences play a role in alleviating emotional distress, this is potentially one way in which psilocybin has greater potential.
Neurological Differences Between Ketamine vs Psilocybin
Both ketamine and psilocybin promote rapid neuroplasticity in the brain, which is correlated with improved sustained mental health benefits in patients. However, the main way in which ketamine is believed to benefit patients with depression and suicidality is through these rapid brain changes, since, as we saw earlier, the subjective effects of ketamine matter less in terms of reducing depression and anxiety.
Moreover, ketamine and psilocybin promote greater neuroplasticity through different pathways: in the case of ketamine, by blocking NMDA receptors, and in the case of psilocybin, by activating serotonin receptors.
Different Mental Health Outcomes
It’s worth noting that the benefits of ketamine and psilocybin vary in how long they are sustained.
Research shows that the depression-reducing benefits of ketamine last a few days to two weeks: this is why multiple rounds of ketamine therapy sessions are often undertaken. This is critical for extended recovery.
In contrast, 1-3 psilocybin sessions have been found to offer sustained mental health benefits for up to a year (some patients will also remain in remission longer than this).
Data gathered from MycoMeditations retreats shows that attendees report significant, long-term reductions in PTSD, depression, and anxiety symptoms, with symptoms decreasing over 50% when measured one year post-retreat.
While research is still investigating why ketamine and psilocybin differ in their long-term benefits, one potential reason, as we touched on, is that psilocybin often provides a more emotionally, psychologically, and spiritually profound kind of experience.
The Experience of Ketamine vs Psilocybin
While both ketamine and psilocybin can produce effects like introspection, insights, visions, heightened emotions, and mystical experiences, the subjective effects are not exactly the same.
First, ketamine is classed as a dissociative anesthetic. It reliably produces dissociative experiences, such as feeling detached from one’s body and other kinds of out-of-body experiences. As a dissociative, it is also common for people to feel more ‘at a distance’ from psychological material, which can help people observe and examine this material without feeling overwhelmed.
Interestingly, this dissociative compound can be used to help people who are dissociated from their traumatic experiences. One psychedelic therapy training even focuses on addressing dissociation with ketamine.
Trauma can leave people either slightly or highly dissociated from the event or experiences as part of the body’s defense mechanism. It could be reasonable to suggest that ketamine mutes the part of the mind that is holding the dissociated trauma response so that the raw experience can be accessed and processed to at least some degree.
Psilocybin, in contrast, is not a dissociative but is instead, a classic psychedelic. Dissociating experiences are possible, but this only really happens when the experience isn’t approached or handled with care. The acute distress of such an experience can cause someone to feel disconnected from their body, self, or world.
Generally, when it comes to the therapeutic effects of psilocybin, it works in essentially the opposite way of ketamine.
Where ketamine tends to quiet everything enough for traumatic material to arise in a neutral, indirect way, psilocybin gradually opens people to the raw emotions and feelings behind the trauma. In this way, psilocybin therapy allows people to go straight to the core of what they are holding onto.
While this process often makes psilocybin therapy more intense, we suggest that this is why therapeutic outcomes are deeper and better sustained.
At some point, you must go back to where it started if you want to heal.
Classic psychedelics like psilocybin also tend to produce more ‘classic’ psychedelic visual effects, such as color enhancement, geometric visual effects (with eyes open and closed), and objects breathing and morphing.
Ketamine often distorts visual perceptions, too, but with eyes open, this tends to be more distortions in perspective and size (e.g., things appearing closer or further away than normal, or things looking bigger or smaller than normal).
With eyes closed, the visuals of ketamine typically differ from those produced by psilocybin. Often, the visual experience is described as more dream-like and immersive, while psilocybin often produces more vibrant and symbolic imagery.
Another key way in which ketamine differs from psilocybin is in the duration of the experience. You can expect to be back to baseline an hour after taking ketamine, whereas for psilocybin, the journey back to baseline takes anywhere from four to six hours.
The onset of ketamine’s effects is also quicker than that of psilocybin: they occur within seconds or a few minutes following administration (i.e., intravenous (IV) or intramuscular (IM) injection), whereas after consuming psilocybin mushrooms, the first effects are usually felt within 30-60 minutes.

Therapeutic Settings and Delivery Methods: Psilocybin vs Ketamine
In countries where ketamine therapy is legal, it is administered in a clinical setting. Where psilocybin is legal, however, it is not typically administered in a medical setting such as a hospital or clinic (except in the case of legal psilocybin clinical trials).
The exception, in the case of ketamine, is ketamine telehealth therapy, where someone self-administers sublingual ketamine (a dissolving tablet) at home, with video chat support from a mental health professional.
In the case of Oregon, psilocybin sessions can be legally held in service centers, which are not ‘clinics’ in the traditional sense – they do not provide diagnosis or prescriptions. However, they may be thought of as clinics in a therapeutic or wellness context, in that people visit them to improve their mental health.
Where psilocybin is legal, psilocybin retreats often operate as well, whereas ketamine can only be legally administered in a licensed medical setting. Taking ketamine may, in more limited cases, be taken in a retreat setting, but the administration itself would have to be in a medical capacity.
In a therapeutic context, ketamine is typically delivered via IV injection (although IM injection can be used, as well, with the onset of effects occurring more quickly with IV). Lozanges are common too.
Psilocybin, on the other hand, is always taken orally (as whole psilocybin mushrooms, typically dried, or as an extract or in synthetic form). Unlike ketamine, psilocybin is never delivered via injection; it is also never snorted, as ketamine normally is in recreational contexts or when using the FDA-approved nasal spray (Spravato).
Legal Status and Access: Ketamine vs Psilocybin by Country
As a mental health treatment, ketamine is legal in the US, the UK, Canada, Australia, and all EU member states. Legal psilocybin therapy, meanwhile, is available in Oregon, Colorado, Jamaica, the Netherlands, Australia, Canada, and Switzerland.
However, the ability to access ketamine therapy and psilocybin therapy often differs. For example, ketamine-assisted psychotherapy is FDA-approved for the treatment of treatment-resistant depression and major depression with suicidality. It can also be legally used off-label to treat other conditions like PTSD, anxiety disorders, OCD, bipolar disorder, and substance use disorders.
In Oregon and Colorado, on the other hand, legal psilocybin sessions are available to anyone aged 21 and older, regardless of medical diagnosis. And in countries with more restricted access – such as Canada, Switzerland, and Australia – psilocybin therapy is available to patients only if they meet a specific diagnosis, such as treatment-resistant depression and end-of-life distress.
Safety and Screening: Ketamine vs Psilocybin Risks and Eligibility
Ketamine and psilocybin also differ in their safety profiles.
Ketamine has a (much) higher potential for abuse, and ketamine abuse and addiction are associated with physical problems such as incontinence and bladder damage. The term ‘K bladder’ has emerged from this link. Psilocybin, on the other hand, is physically non-toxic and non-addictive.
Screening for ketamine therapy and psilocybin therapy differ as well. While schizophrenia is typically an exclusion criterion for both treatments, patients with suicidality and bipolar disorder can be accepted for ketamine therapy (as it’s deemed safe and effective, and in the case of suicidality, potentially life-saving).
However, people with bipolar disorder and suicidality are usually screened out of psilocyin clinical trials and psilocybin therapy, due to concerns that the experience may trigger or worsen a manic episode or suicidality, respectively.
Ketamine and Psilocybin Are Different Tools: Comparison Should Be Contextual and Safety-First
Ketamine and psilocybin are both promising new treatments for a range of mental health conditions. They both provide benefits to people through altered states of consciousness combined with enhanced neuroplasticity.
However, as we’ve seen, there are important differences between the two compounds in terms of experience, duration, legality, safety, and potential benefits. So while ketamine and psilocybin share some similarities, their differences need to be understood so that they can be used safely, in the right instances, and with realistic expectations.
With this understanding in place, one can approach ketamine therapy or psilocybin therapy with a prepared mindset, which is essential for having beneficial, therapeutic experiences.
Ketamine vs Psilocybin FAQs: Experience, Safety, and Therapy Differences
What is ketamine, and how is it different from psilocybin?
Ketamine is a dissociative anaesthetic with psychedelic effects. It’s different from psilocybin because it is synthetic in origin (although it can, in very limited contexts, occur in nature); it is classed as a dissociative; it was first used as an anesthetic (whereas psilocybin, as far as we know, was first used by humans as a religious sacrament); and it creates subjective effects through activity at glutamate receptors (rather than serotonin 5-HT2A receptors in the case of psilocybin). Also, psilocybin is a classic psychedelic, whereas ketamine is commonly referred to as a non-classic psychedelic.
How do ketamine and psilocybin experiences feel different?
Ketamine experiences tend to feel more dissociating, where you feel detached from your body, with more dream-like visions. Psilocybin experiences tend to involve more vivid colors, intricate patterns, symbolic imagery, and deep introspection. Psilocybin experiences are also more likely to involve entity encounters and mystical experiences.
What are the biggest differences in setting and session structure?
Legal, therapeutic ketamine experiences take place in a medical setting only, whereas legal, therapeutic psilocybin experiences can – depending on the jurisdiction – take place in a more home-like setting (i.e., a service center) or a villa-like setting in nature (i.e., a retreat). Ketamine therapy tends to involve 6-12 dosing sessions over several weeks, whereas psilocybin therapy involves 1-2 dosing sessions (spaced 1-3 weeks apart). However, at some psilocybin retreats, longer programs can involve three dosing sessions. A ketamine session is shorter than a psilocybin session (30-120 minutes vs 4-8 hours).
What safety factors should people consider before choosing either option?
Before choosing either ketamine therapy or psilocybin therapy, would-be participants should consider their family and mental health history, medication use, alcohol and drug use, and any underlying medical conditions.
How should integration differ between ketamine and psilocybin experiences?
Since the brain plasticity benefits of ketamine seem to be more critical for mental health benefits than its subjective effects, integration should be about making the most of this more plastic state. This means working with people on maintaining positive shifts and cognition, and developing healthier habits and relationships. Integration tends to be more future-oriented. Integrating psilocybin experiences, however, tends to be more about making sense of a symbolic, emotionally intense, spiritual experience. While psilocybin integration is often future-focused, it tends to be highly experience-oriented. This difference reflects the common need to make sense of psilocybin experiences that may be abstract, ambiguous, confusing, overwhelming, or challenging.

Psilocybin Therapy & How it Can Help People With Life Purpose
Finding life purpose is difficult. Everyone wants to feel that their life is going in a meaningful direction and that they are connected to a passion that brings them genuine fulfilment and satisfaction.
But how do we actually find life purpose? It’s not as easy as deciding on any random goal or career path, or what others tell us we should do, and hoping that this will feel purposeful and meaningful.
There are many ways to arrive at a more authentic (freely chosen and personal) sense of purpose in life.
Finding life purpose in this way often involves periods of introspection and self-reflection to discover one’s core values, which you can then shape and mold into a desired lifestyle.
A new path for catalyzing this process of self-discovery is psilocybin therapy.
Psilocybin experiences with psychological support – before, during, and after – allow people to have deep, internal experiences that catalyze the radical introspection and self-reflection needed to find life purpose. It’s no surprise that many people report their psychedelic experiences as one of the most meaningful experiences in their lives.
In this article, we’ll be delving into finding life purpose through psilocybin and the research indicating that this is a real benefit of psychedelics (and an underappreciated one).
What Is Life Purpose? Meaning, Direction, and Personal Values
“Life purpose” is one of those terms that, due to its complexity and philosophical roots, can be tricky to define.
Meaning and purpose tend to go hand in hand, and might be viewed as interchangeable in some people’s eyes, but they are distinct.
According to cognitive scientist John Vervaeke, meaning refers to one’s ongoing relationship to reality, specifically, being deeply connected to reality and gaining wisdom through this relationship. In contrast, life purpose is goal-oriented; it is an overarching direction or motivation in one’s life. Life purpose is one’s “mission”. For life purpose to be meaningful, however, it has to be coupled with deep connectedness to reality, wisdom, and self-transformation.
Of course, one person’s purpose in life will be different from someone else’s. This is because, as mentioned earlier, people have core values, and these values are unique for different people. People, of course, differ in their interests as well, which also determine a path in life that feels purposeful.
Signs of purposeful activities in life, which have a life-enhancing goal or effect, include:
- Personal growth: The activity leads to the improvement of one’s abilities, virtues, and relationships. Another way to phrase this is to say that the activity, project, or path in life benefits self-actualization, which the psychologist Abraham Maslow defined as the realization of one’s true potential; or as he put it, “What a man can be, he must be.”
- Sense of fulfilment: The activity provides a feeling of enthusiasm, joy, and peace.
- Contributions to others: Meaningful activities, or those with a purpose, are also those that improve the lives of others. This might involve committing oneself to a cause bigger than oneself, such as poverty or the climate crisis, or even just being committed to being more compassionate and friendly in everyday life.
- Fostering connection: A greater feeling of connectedness in life, whether it’s with others or the world around us, often feels like a life purpose for many. Without a genuine sense of connection, it can feel like an essential element of life is missing.
- Spirituality: For many, this involves being in relationship with a higher power or spirit(s), whereas for more secular-minded people, spirituality may encompass the other factors we’ve taken a look at: growth, deep fulfilment, serving others, and connectedness.
Why So Many People Struggle With Finding Life Purpose
Now that we’ve outlined the key aspects of life purpose, why do many people struggle to find it?
There is no single answer to this question that applies to all people. Nonetheless, there are several possible barriers that get in the way of people finding their life purpose.
External Pressures and Social Expectations
First, we all face and are influenced by external social pressures at one point or another.
Expectations from parents, other family members, friends, and cultural narratives can lead one to pursue a career or life goals that don’t feel personally fulfilling. This means we must become conscious of whether these external pressures are even valid.
Do they make sense?
Do they serve our best interests?
Often, these pressures are based on norms and values that have been built up through generations, maintained by tradition, culture, and even trauma. If strictly adhered to, these external pressures can get in the way of many people’s life purpose.
A Lack of Self-Reflection and Introspection
Second, many people live a life without dedication to self-reflection.
This often isn’t due to a lack of time; self-reflection just requires mindfulness, prioritization, and discipline. The nature of our fast-paced society and a cultural lack of value in introspection mean that self-reflection sits far down on the list of what many people value. And often, not understanding why it’s healthy to question our way of living means that introspection is never valued in the first place. Once introspection is prioritized and become a normal part of existence, people naturally self-reflect in ways related to their life.
Patience, Change, and the Evolving Nature of Life Purpose
Third, self-reflection might not deliver any concrete answers right away, but that’s because it takes time to understand one’s life purpose. It’s a process of continual observing, listening, learning, and shifting. Finding life purpose is an active pursuit, not a passive or random occurrence.
A person’s purpose is likely to change throughout their life. To identify and connect with the current sense of purpose, alongside the awareness to understand when it changes, is a continual pursuit. Embrace this as an ongoing process for living a healthy life.
Psilocybin Therapy as a Catalyst for Finding Life Purpose
Psilocybin therapy is seen as a powerful way to discover or reconnect with life purpose. Psychedelic experiences open windows of intense self-reflection and profound insights, often related to themes like meaning, purpose, authenticity, and personal growth.
There are multiple ways in which psilocybin therapy leads to these kinds of insights.
Disrupting Default Thought Patterns Through Psilocybin Therapy
One way psilocybin is effective at helping people find life purpose, for both healthy populations and people struggling with a mental health challenge, is through the disruption of default ways of thinking. And we know at the level of the brain.
The default mode network (DMN) is a brain network that is most active when the brain is at rest, such as when recalling memories, planning for the future, daydreaming, and mind-wandering. It is involved in self-reflection and our sense of self. Psilocybin has been shown to dampen DMN activity. This mechanism frees people from their habitual thought patterns and sense of self.
As a result, the brain becomes hyperconnected. Brain regions that don’t normally communicate with each other start doing so, and this allows new, alternative kinds of thinking and self-perception to emerge. This window of experience often comes with impactful insights, new perspectives, and new models of reality.
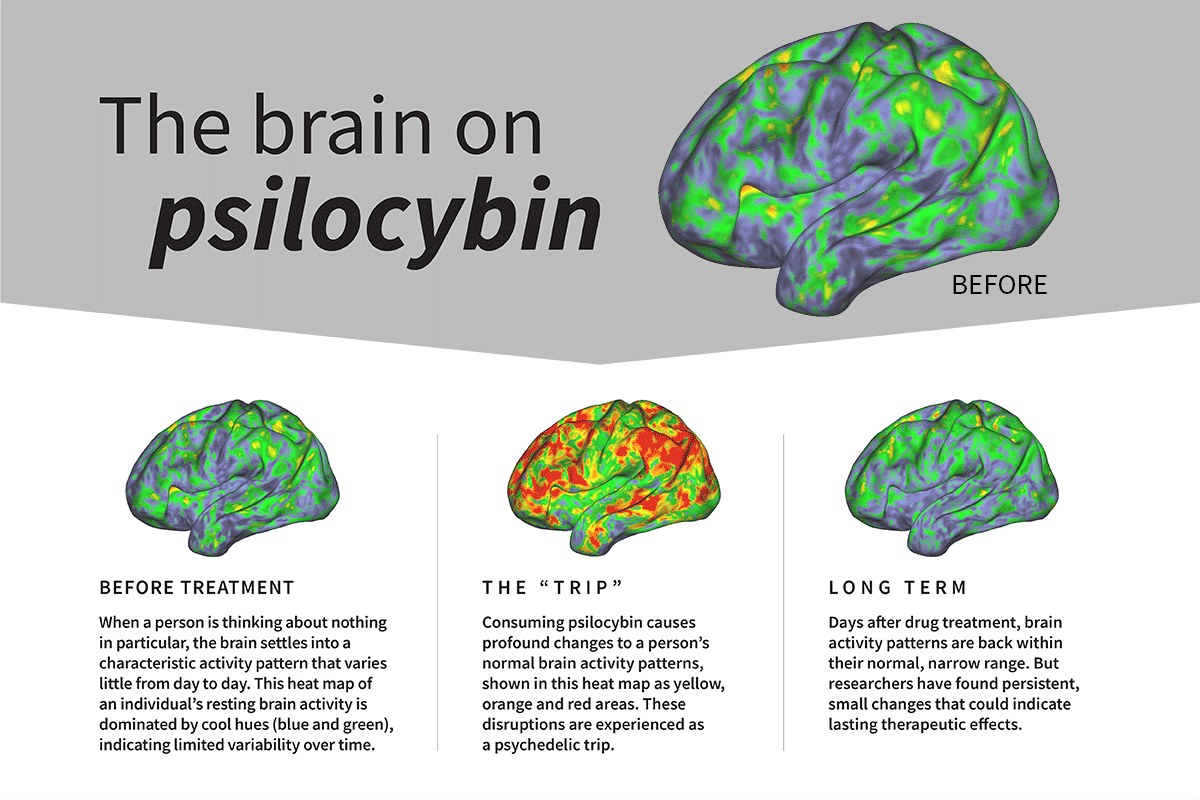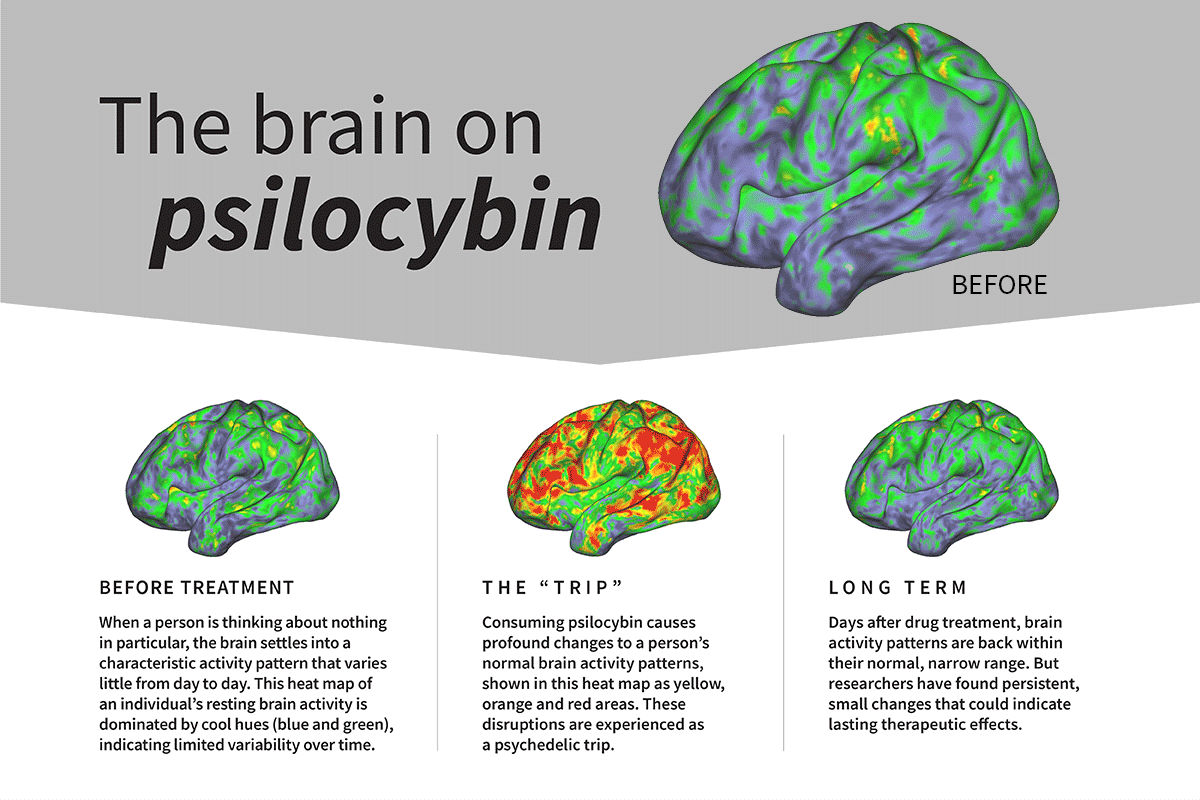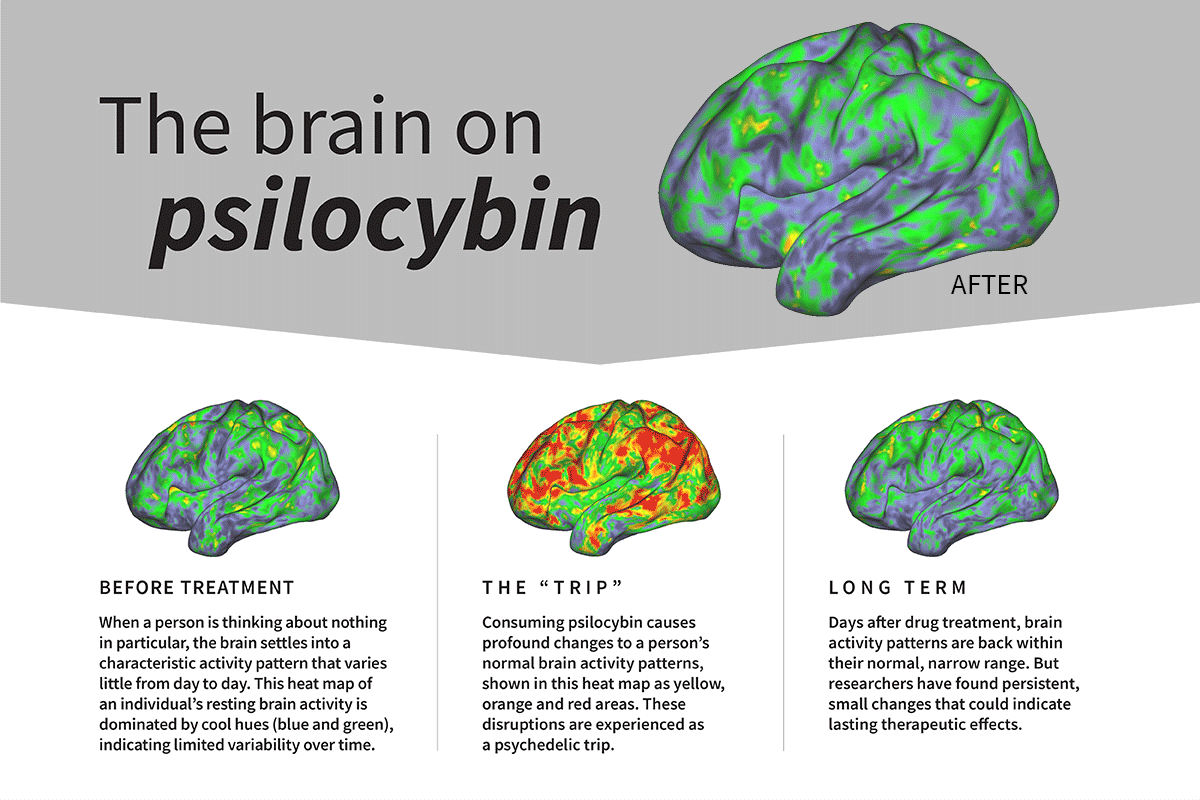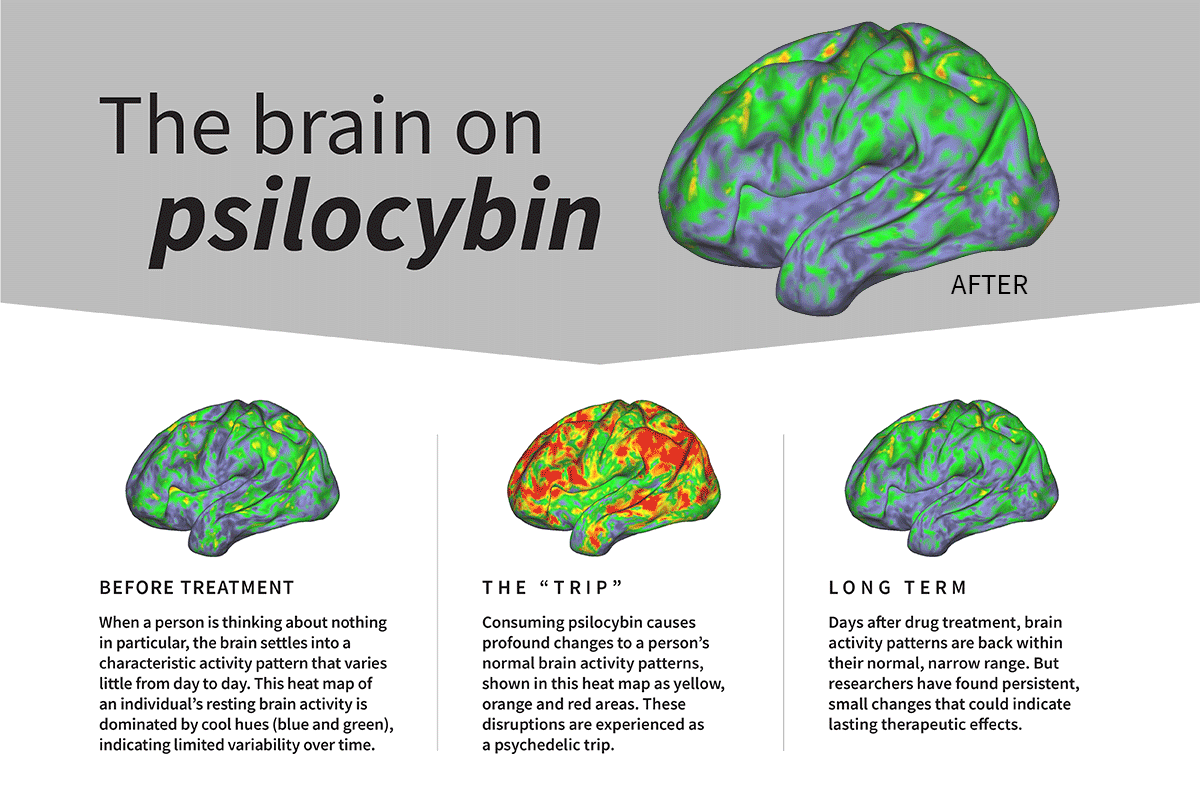
Mental health conditions such as depression and anxiety can also interfere with connecting to your purpose in life. Finding life’s purpose could be considered the top of Abraham Maslow’s hierarchy of needs. People will struggle with connecting to this need if they are bogged down by feeling worried, depressed, and ultimately unsafe. There isn’t enough space available for higher-order thinking.
However, psilocybin creates this space by weakening the DMN. Distinct DMN activity has been linked to rumination in mental health conditions like major depressive disorder (MDD). In other words, people with conditions like depression, anxiety, and OCD repeat the same negative thought patterns, which contribute to emotional distress.
In depression, self-referential thinking – the kinds of thoughts people have about themselves and who they are – becomes overly and consistently negative. People can feel like they have no purpose and nothing to offer to the world.
By freeing people from these mental ruts by disrupting the DMN, psilocybin allows people with mental health conditions to reconsider who they are and their life’s purpose.
Emotional Breakthroughs, Insights, and Mystical Experiences in Psilocybin Therapy
According to MycoMeditations CEO & Head Facilitator Justin Townsend, the three key mediators of psychedelic experiences are emotional breakthroughs, cognitive insights, and mystical experiences.
First, psilocybin often results in emotional breakthroughs or experiences of deep catharsis and resolution of an emotional wound or problem in one’s life.
Our experience of life and the ways of interacting with it are shaped by our past experiences. Many people have unprocessed trauma – singular trauma or complex traumas – which prevents them from having a more authentic, core connection to life. Psilocybin experiences can help people break through these emotional blocks and gain a clearer sense of life purpose.
Second, the psychological insights occasioned through psychedelic experiences often possess a connection as if they are coming from a higher place, such as a part of you beneath all the layers of trauma, conditioning, defence mechanisms, and bias. The filters of reality are pulled back for people, where access to a pure layer of thinking and processing takes place.
A 2025 study, for example, found that people who’ve had psilocybin experiences reported “long-lasting insights into their lives and values.” In a single psilocybin experience, someone may have deep insights that lead to the discovery of a life purpose.
Third, at high enough doses, and with the right preparation and support in place, psilocybin can induce mystical-type experiences. These are states of consciousness that feature qualities like ego dissolution, unity, interconnectedness, a sense of the divine or sacred, transcendence of time and space, ineffability, and a noetic quality (the feeling that the experience is objectively real).
Through mystical experiences, people finally connect to a state of being that doesn’t revolve around themself. People connect with something larger than themselves, and clarity around their own unique place within the bigger picture of life emerges. It’s also well-known in psychedelic research that mystical experiences are correlated with a range of persisting and positive effects in people.
Metaphysical, Spiritual, or Long-Term Perspective Shifts After Psilocybin Therapy
Psilocybin therapy, often because of the profoundness of mystical experiences, may lead people to adopt new worldviews.
For example, many (but not all) participants become more inclined to adopt metaphysical beliefs, such as panpsychism (consciousness is everywhere), idealism (consciousness is fundamental and the only real thing), animism (everything has a soul), and belief in God, a higher power, or ultimate reality.
Many people also shed their fear of death, which some research has tied to mystical experiences, as many people come away with a belief in consciousness continuing after death. Newer research finds a stronger predictor of reduced death anxiety is “impermanence acceptance”: the emotional acceptance of the fact that one’s life is temporary.
Other possible long-term perspective shifts caused by psilocybin therapy, which can make finding life purpose easier, are enhanced empathy and prosocial behavior, greater connectedness to others, and increased care for the environment and pro-environmental behaviors.
Changes of this magnitude related to such a core belief system within people will greatly shape their felt sense of life purpose.
Psilocybin Therapy May Open New Perspectives – But Purpose is Built Over Time
We can’t discuss important life changes related to psilocybin without emphasizing the importance of integration after psilocybin therapy. It’s one thing to have a clear insight into what one’s meaning and purpose in life is. But it takes time, attention, and effort to translate this insight into actual changes.
It’s crucial to keep in mind that while psilocybin therapy can (and often does) open people to new perspectives – perspectives which relate to meaning and purpose – life purpose is still built over time. Sometimes, continued therapeutic support will be needed.
Integrating psychedelic insights – turning new perspectives into a life lived with purpose – doesn’t end when psilocybin therapy ends. It tends to be a continued process of self-discovery.
Frequently Asked Questions About Psilocybin Therapy and Life Purpose
Why do people struggle with finding life purpose?
People struggle with finding life purpose for multiple reasons, including external social pressures, a lack of self-reflection, and difficulty arriving at concrete answers through self-reflection. However, psilocybin therapy gives people space to reflect and a more flexible way of thinking, which can encourage insights into life purpose.
How is psilocybin therapy discussed in meaning-related research?
Psilocybin therapy has been found to lead to lasting increases in people’s sense of personal meaning and spirituality. Participants find that their lives have more meaning and that they discover a more purposeful path in life.
What kinds of perspective shifts are commonly reported after psilocybin therapy?
Commonly reported perspective shifts include metaphysical belief shifts, acceptance of mortality, enhanced nature connectedness, and a higher degree of self-compassion and empathy towards others.
Why is integration of psychedelic experiences critical for lasting change?
Integration is essential for lasting change because without it, insights won’t turn into concrete traits and behaviors. They’ll just remain as insights. Integration involves taking actionable steps that translate insights into relevant changes (e.g., wanting to protect the environment may turn into a career or voluntary work related to environmental protection).
What are the ethical and safety boundaries of using psilocybin therapy to help with life purpose?
The ethical and safety boundaries in psilocybin therapy involve psychedelic therapists not imposing their own sense of meaning and purpose onto patients. Participants in psilocybin therapy can enter into highly suggestible and vulnerable states, and this, alongside the power dynamics involved, can make participants more susceptible to the influence of facilitators. It’s essential, therefore, that psilocybin facilitators adopt a more non-directed approach, giving participants the freedom to arrive at their own sense of meaning and purpose.

Finding Life Purpose Through Psilocybin Therapy
Psilocybin for Neuropathic Pain
In many countries around the world, the prevalence of neuropathic pain is nearly 10%. Millions of people struggle with this form of chronic pain, which can disrupt everyday functioning and degrade quality of life. Resulting from damage or disease to the nervous system, neuropathic pain is also associated with psychological distress, such as depression, due to the degree of pain involved and its impact on everyday life.
Many people manage their neuropathic pain with a mixed approach, including the use of medications, physical therapies, and psychological support. However, conventional approaches can fail to work or inadequately alleviate the pain and distress for the person living with it.
Fortunately, psilocybin research indicates that this psychedelic may not only be effective at alleviating mental health conditions; it could prove helpful for pain conditions like neuropathic pain as well.
What Is Neuropathic Pain? Understanding Chronic Nerve Damage Pain
Neuropathic pain (or nerve pain) is a type of chronic pain that results when the nervous system gets damaged or malfunctions. People with neuropathic pain may feel pain in any level of the nervous system, such as the spinal cord or brain (which make up the central nervous system), or the peripheral nerves – the nerves that spread to the rest of the body, such as the organs, limbs, fingers, and toes.
Common Symptoms of Neuropathic Pain and Nerve Damage
Essentially, when nerve fibers get damaged or malfunction, which may occur as a result of disease, they send incorrect signals. This can lead to pain and other distressing symptoms.
The possible symptoms of neuropathic pain include:
- Spontaneous pain: this can feel like burning, stabbing, an electric-like shock, tingling, numbness, or “pins and needles”.
- Extreme sensitivity to touch (allodynia): stimuli that are normally painless, such as cold or pressure (even light pressure), cause pain.
- Extreme sensitivity to pain (hyperalgesia): stimuli that are normally painful, such as heat or pinpricks, cause an increased pain response. In other words, things hurt more than they should.
- Decreased pain response (hypoalgesia): painful things are less painful than they should be. For instance, someone may be unbothered by a pinprick.
Other symptoms include:
- Unrelenting itching.
- Insomnia, as well as emotional distress related to disturbed sleep and chronic pain.
- Lack of coordination and falling (this can be related to reduced sensation in the feet).
- Muscle weakness, twitching, or cramping.
- The feeling of wearing gloves or socks when you’re not.
- Inability to move (if the motor nerves are affected).
The Causes of Neuropathic Pain
There are many possible causes of neuropathic pain, including:
- Inflammatory neuropathies, such as Guillain-Barré Syndrome (GBS) or Chronic Inflammatory Demyelinating Polyradiculoneuropathy (CIDP)
- Metabolic conditions (most commonly diabetes)
- Infections, such as Shingles, HIV, Lyme disease, and Hepatitis C
- Nerve damage resulting from accidents, falls, or surgical complications
- Alcoholism
- Chemotherapy and radiation drugs
- Autoimmune diseases, such as rheumatoid arthritis
- Nervous system disorders, such as Multiple Sclerosis and Parkinson’s Disease
Why Neuropathic Pain Is Hard to Treat With Conventional Medications
First, neuropathic pain can be tricky to manage because, even once the underlying cause is identified (e.g., a specific disease), the cause itself may be difficult to treat. For example, some conditions underlying neuropathic pain are not (currently) curable, such as Parkinson’s Disease. So patients and their doctors need to find a pain-relieving strategy that works for them. This can take time, trial and error, and a fluctuation between improved and worsened symptoms, until an optimal strategy is worked out.
In the case of Parkinson’s, specifically, one challenge is that the most common Parkinson’s medication, Levodopa, can also induce neuropathic pain, which might create the challenge of needing to find an effective way to resolve this side effect.
Second, when conventional treatments for neuropathic pain do offer relief, this may also come with unwanted side effects. For instance, common treatment options for nerve pain damage include tricyclic and SNRI antidepressants, anticonvulsant (anti-seizure) medications, and opioids. These drugs may, for some people, involve unpleasant physical and psychological side effects. Stopping the use of antidepressants and opioids can also result in withdrawal symptoms.
Third, whether or not medications involve unwanted side effects, they may still not offer adequate relief. This is why other treatment options are often recommended, such as physical and occupational therapy, cognitive behavioral therapy (CBT), mindfulness, a nutritious diet, regular exercise, and avoiding smoking and drinking. These may all help manage symptoms, but again, it can take some trial and error to find a specific lifestyle change, such as a dietary change, that provides noticeable relief.
Why Researchers Are Studying Psilocybin for Neuropathic and Chronic Pain
Psilocybin’s properties for catalyzing enhanced neuroplasticity, as well as its ability to help people overcome the trauma at the root of numerous mental health disorders, both reveal what makes psilocybin a promising treatment for neuropathic pain.
Psilocybin Increases Neuroplasticity and How This Helps Neuropathic Pain
Researchers have found that neuropathic pain involves maladaptive brain plasticity. In other words, the brain’s ability to rewire neural connections is impaired, leading to symptoms such as heightened pain sensitivity.
This doesn’t mean there is necessarily less plasticity, just that maladaptive brain plasticity is seen when the brain is unable to reorganize itself successfully. A disruption in this process can lead to dysfunctional patterns in pain processing, such as various forms of chronic pain or developing neuropathic conditions. In fact, many researchers are now recognizing neuropathic pain as a neuroplastic disorder.
Psilocybin is a promising treatment for neuropathic pain because it enhances neuroplasticity. Crucially, it increases adaptive neuroplasticity: it helps the brain reorganize itself in ways that lead to positive neural patterns, not harmful ones.
For example, enhanced neuroplasticity following psilocybin administration is associated with improved mood and emotional regulation. Because of this, researchers are also interested in the potential of psilocybin to increase adaptive brain plasticity in patients with nerve-damage pain. In a paper published in Medical Sciences (Basel), the researchers underscore:
“Emotional processes are now seen as important factors in causing and sustaining chronic pain, and mechanisms such as neuroplasticity in pain processing networks and neuroinflammation seem to be crucial to the maintenance of chronic pain states. Thus, psychedelic drugs [including psilocybin], by affecting neuroplasticity and neural networks and by modulating inflammation and the neuroimmune axis, present promising therapeutic opportunities.”
How Addressing the Root of Trauma with Psilocybin Could Lead to Positive Downstream Effects on Neuropathy
The link between emotional processes (those impacted by trauma) and pain, and how this relates to neuroplasticity, highlights the strong possibility that we see for psilocybin as a treatment for neuropathic pain.
We already know psilocybin helps to address emotional forms of pain, often caused by trauma. Psilocybin-induced altered states can allow patients to revisit, confront, process, and reframe the traumatic events from their past. We also know that PTSD and chronic pain often occur together and share neurological processes.
But what does trauma have to do with neuropathy?
Research shows that people who experienced childhood trauma have higher levels of pro-inflammatory markers as adults. Essentially, this means that trauma burdens people’s nervous systems, which can lead to downstream effects, such as neuropathy.
By addressing trauma during one or more psilocybin therapy sessions, it is possible that a state of chronic, elevated stress in the nervous system can be alleviated. Reduced neuropathy may then be a natural outcome of this alleviation on the person’s nervous system.
This same process may then enable the body’s innate ability to regenerate its nerves — with limitations regarding damage to the central nervous system — to rebuild damaged nerve endings or to create a new environment in which nerve regeneration treatments more easily succeed, such as stem cell therapy, platelet-rich Plasma (PRP) therapy, or electrical stimulation/neuromodulation.
Because psilocybin lacks the side effects associated with common neuropathic pain treatments, such as antidepressants and anticonvulsants, it is a promising candidate for treatment. In addition, psilocybin is known to be non-toxic and non-addictive (in fact, research indicates it helps to combat addiction). In contrast, antidepressants and opioids may have iatrogenic effects (drug-related harms), such as withdrawal symptoms.
What We Know About Psilocybin and Neuropathic Pain
A growing body of research suggests that psilocybin can be effective for the treatment of chronic pain disorders, such as fibromyalgia.
In animal studies, researchers found that a single dose of psilocybin led to a rapid and sustained alleviation of allodynia and anxiety- and depression-like states. In other words, psilocybin helped treat chronic neuropathic pain, including not just the physical pain but also the mood changes associated with the condition.
The study authors state, “Using local psilocin injections, the key active metabolite of psilocybin, we show that the engagement of prefrontal cortical circuits is critical for the concurrent alleviation of both conditions [allodynia and psychological distress].”
This finding supports the idea that psilocybin’s alleviation of neuropathic pain is based on restoring the normal functioning of brain regions, in this case, the prefrontal cortex, which is involved in emotional regulation and pain processing. Dysfunction in this brain region is associated with chronic pain, including neuropathic pain.
In another paper, researchers consider potential mechanisms of action by which psilocybin alleviates chronic pain, “including targeting serotonergic pathways through the activation of 5-HT2A receptors at both spinal and central levels, as well as neuroplastic actions that improve functional connectivity in brain regions involved in chronic pain.”
In a different vein, a 2025 study published in the Journal of Pain found that psilocybin can aid chronic pain rehabilitation by improving self-perception and meaning-making (allowing a chronic pain patient to reform their sense of identity in light of their illness and generate meaning in life). In this way, psilocybin is useful not just for addressing the brain-pain connection but also for the emotional toll that nerve-damage pain involves.
Limitations of Current Research on Psilocybin and Neuropathic Pain
A systematic review of studies on psilocybin and neuropathic pain shows promise, but there are some caveats to note.
Researchers analyzed 28 relevant studies. They found that “current research shows potential for psilocybin as a treatment option for chronic pain relief,” but stress that “methodological issues and a lack of high-quality evidence underscore the need for further investigations with standardized protocols.” For example, the authors highlight, “The majority of the included studies (76.2%) were of low or very low quality.”
The low-quality studies were mainly case series and reports, not placebo-controlled clinical trials. This made them susceptible to bias. A lack of close monitoring, standardized protocols (such as with dosing), representative patient selection, and long-term follow-ups also jeopardizes the quality of evidence. However, as the authors point out, future studies could be more rigorously designed, which could help to bolster the promising findings made so far.
Psilocybin Safety for Neuropathic Pain: Screening and Contraindications
Certain psilocybin research and anecdotal reports indicate that this classic psychedelic can help patients experience significant and lasting reductions in neuropathic pain symptoms. Yet, while this may motivate some people living with nerve damage pain to seek out psilocybin treatment, it’s important to stress that psilocybin does involve some contraindications.
As a result, psychedelic clinics and retreats need to have careful screening protocols in place. This ensures that someone with neuropathic pain doesn’t take psilocybin if they have other conditions or medication use that could result in harm.
For instance, if someone with neuropathic pain also has a personal or family history of schizophrenia, bipolar disorder, or a personality disorder, they may not be deemed suitable for psilocybin therapy. This is because most of the research on psilocybin and neuropathic pain involves macrodoses of psilocybin, which are doses large enough to cause psychedelic effects. It is these altered states of consciousness that may be risky for these vulnerable individuals.
A New Lens on Neuropathic Pain – With Ongoing Research
Clinical trials in the future could help to further illuminate the efficacy of psilocybin for neuropathic pain. By comparing psilocybin to placebos, as well as to conventional treatments, we can see precisely how effective this psychedelic is in improving the physical and psychological symptoms of nerve damage pain.
Further research may also help to establish whether microdosing and non-hallucinogenic versions of psilocybin could benefit neuropathic pain without altered states, which would be options for those normally screened out of psychedelic studies, treatments, and retreats.
As it stands, the research on psilocybin for neuropathic pain is already promising. It indicates that this psychedelic compound addresses this type of pain in a unique way, distinct from conventional medications. By enhancing neuroplasticity and addressing deep emotional wounds, psilocybin can restore the nervous system, allowing people to feel the weight of their emotional and physical pain lifted.
FAQs About Neuropathic Pain and Psilocybin Therapy
What makes neuropathic pain uniquely challenging?
Neuropathic pain is uniquely challenging because the physical and emotional pain can be severe; it can be hard to identify the cause; conventional treatments (even when combined) may not offer adequate relief; and even when these treatments do provide relief, they may come with side effects.
How does the brain shape the experience of nerve pain?
The brain and spinal cord become hypersensitive to incoming pain signals, which increases pain perception. Maladaptive plasticity in the brain occurs, where the brain reorganizes its neural pathways in harmful ways; specifically, neural pathways related to pain are rewired, leading to chronic, persistent pain.
Why are researchers exploring psilocybin in pain studies?
Psilocybin can enhance adaptive neuroplasticity, plus it is non-toxic, non-addictive, and lacks the side effects of traditional medications. Furthermore, through the altered states of consciousness it induces, psilocybin can provide additional benefits such as an improved sense of identity and meaning-making.
What does current evidence suggest about psilocybin for neuropathic pain, and what does it not?
The current evidence suggests that psilocybin can reduce pain perception and improve the mental well-being of patients. It does not show, however, that psilocybin is a cure for neuropathic pain: we do not have evidence that it eliminates all neuropathic pain. Therefore, psilocybin should be viewed as a potentially effective way to manage symptoms. Another hypothesis is that, by addressing trauma, psilocybin can alleviate the constant stress that the nervous system is under. Since chronic stress has been linked to neuropathy and chronic pain, it’s possible that psilocybin’s emotional impact can have downstream effects on pain perception.
Why are safety and screening essential?
Safety and screening are essential to ensure that somebody doesn’t take psilocybin for neuropathic pain and experience any contraindications. Trustworthy clinics and retreats should have rigorous exclusion criteria in place, so that people don’t risk a worsening of physical or mental health as a result of psilocybin use.

Neuropathic Pain and Psilocybin: Addressing Nerve Damage Differently
Contraindications for Psilocybin: Understanding Medications, Conditions, and Screening
While psilocybin proves beneficial for many people, some should avoid using this psychedelic (as well as the other psychedelics). This is because psilocybin has contraindications, meaning it shouldn’t be used in some situations because there is a risk of harm. Certain physical and psychological conditions as well as medications can increase that risk if psilocybin is used.
In this article, we’ll be taking a look at common psilocybin contraindications and how proper psychedelic screening can help protect users’ well-being, whether this takes place in clinical or retreat settings.
Why Psilocybin Screening Is Essential for Safety and Eligibility
Psychedelic screening involves checking would-be participants’ physical and mental health, as well as their use of medications or supplements. Participants may be asked about their physical and mental health history, including historical and current diagnoses. This screening process is important given some of psilocybin’s contraindications.
The risks of psilocybin do not apply equally to all people. Some mental health conditions, for instance, may be worsened by an intense psychedelic experience. And certain medications can lead to physical complications, varying depending on the type of medication that someone uses.
Psilocybin Contraindications Related to Mental Health
A growing body of evidence indicates that psilocybin therapy can offer significant and long-lasting benefits for people with depression, anxiety, PTSD, end-of-life distress, and addiction. In clinical trials of psilocybin therapy for these conditions, researchers also highlight psilocybin’s safety.
Some uncomfortable effects can occur, such as headache, anxiety, dizziness, and nausea, but these effects are typically short-lived and highlight the often surprising physical component of this type of therapy.
The vast majority of participants do not experience persistent negative effects from psilocybin, and serious adverse events are rare. In these rare cases, particularly when the considerations shared in this article aren’t properly taken into account, people can experience a range of challenges following a psychedelic experience, such as Hallucinogen Persisting Perception Disorder (HPPD), emotional and mood difficulties, and issues with perception of self and reality.
Prolonged adverse effects are more common in underground or uncontrolled settings. In clinical trials, in contrast, researchers deem psilocybin therapy safe and effective for the treatment of mood dysfunction, for example.
Approaching psilocybin therapeutically can help prevent adverse outcomes, such as experiences of destabilization, depersonalization, and ontological shock. Careful instruction and skilled guidance go a long way in helping participants let go and surrender to the psilocybin therapy experience, which protects them from these post-experience psychological difficulties. Resisting, rejecting, or not being ready for what manifests during these experiences can leave people shaken up following psilocybin. In addition to this, proper preparation and integration should be provided to help support intense altered states of consciousness.
Failing to provide this support can cause participants to fall into what’s been called a “trauma vortex”, as popularized by Peter Levine. The experience of a trauma vortex is often accompanied by overwhelming fear and extreme rumination. People may start to dissociate as a protective mechanism when entering this state. This process is what can leave people coming out of psychedelic experiences feeling destabilized or left with varying degrees of dissociation (also known as depersonalization or derealization, depending on the experience).
Other important preparations include cultivating an informed and ready mindset in participants (e.g., informing them about possible experiences, particularly based on their background), creating a calm, peaceful environment for the experience, and providing therapeutic touch, if and when necessary (which helps participants feel cared for and grounded during the experience).
The high degree of psilocybin safety observed in clinical trials is also due to the rigorous psychedelic screening that takes place.
Screening involves excluding people with certain mental health conditions or mental health histories. This typically includes a current or past history of schizophrenia, bipolar disorder, borderline personality disorder, or other psychotic disorders, such as delusional disorder, paranoid personality disorder, and schizoaffective disorder.
While psilocybin therapy can be helpful for alleviating depressive symptoms, if these symptoms occur alongside psychotic or manic symptoms, the treatment may be too risky. Through this rigorous screening, the risk of experiences like destabilization is minimized.
These psilocybin contraindications mean that if someone with one of the conditions above takes psilocybin, they may be at greater risk of their symptoms being triggered or worsened. This might involve, for instance, a highly distressing psychotic or manic episode.
A Canadian study showed that people who required acute care (a visit to an emergency clinic or hospital admission) after an incident involving hallucinogens were associated with increases in risk of death relative to the general population, particularly from suicide.
This is why psychedelic screening at retreats must factor in these conditions, as adverse events involving psychedelics can happen.
People at risk for suicide, which might be indicated by suicidal ideation that includes a plan, means, or intent, or suicidal behaviors like a recent suicide attempt, must also be excluded from psychedelic therapy for the time being. This does not eliminate the risk of increased suicidal ideation following psilocybin therapy, as one case study underscores, but it does significantly reduce this risk.
It’s important to keep in mind that there are ways to prevent these adverse events or suicidal ideation following a psychedelic experience.
As we’ve outlined above, issues related to preparation, guidance, integration, or a lackluster screening process can leave people in a highly negative state following a psychedelic experience.
By promoting and practicing thorough therapeutic standards across all levels of psychedelic therapy, we can decrease the odds of these unfortunate outcomes.
Medical Contraindications to Psilocybin Use
Most psilocybin contraindications are related to increased psychological distress, but some are related to physical harm. The main physical concerns related to psilocybin safety are transient increases in heart rate and blood pressure.
This means that serious or uncontrolled cardiovascular conditions are psilocybin contraindications, and so people with these conditions should usually be excluded from clinical trials, psychedelic therapy, and psilocybin retreats.
Antidepressant and Psychiatric Medication Interactions with Psilocybin and the Associated Risks
Clinical trials often require the tapering of antidepressant medications before someone is deemed suitable for taking psilocybin. However, research has not found that using an SSRI antidepressant at the same time as psilocybin increased heart risk or serotonin syndrome.
The latter condition – when an excessive level of serotonin accumulates in the body, which is potentially life-threatening – can occur when taking two drugs that increase serotonin levels in the body. Both antidepressants and psilocybin boost serotonin levels, but there’s little evidence that SSRI antidepressants, in combination with psilocybin, increase the risk of serotonin syndrome.
Case studies have found an increased risk of serotonin syndrome when psilocybin is used in combination with non-SSRI antidepressants. But this link remains an area of ongoing investigation. As it stands, a scientific review concluded that the combined use of antidepressants and psychedelics is safe, although the authors acknowledge limitations and gaps in knowledge in studies on the potential risks.
The risks that do exist are relative to the type of antidepressant used. For example, MAOI (monoamine oxidase inhibitors) prevent the metabolism of serotonin, which could lead to dangerous levels of serotonin when combined with psilocybin or other psychedelics. MAOI antidepressants are riskier to use at the same time as psilocybin compared to SSRI antidepressants.

The main risk we have seen in combining antidepressants with psilocybin therapy, and why we require our guests to wean off their antidepressants with their prescribing professional before arriving, is that the presence of antidepressants in a person’s system will make it difficult to determine a safe therapeutic dose. Antidepressants diminish the strength of psychedelic effects, often to widely varying degrees based on factors such as which exact antidepressants the person is taking, how long they have been taking them, medication dosage(s), and their unique biochemistry.
These factors create uncertainty about determining an appropriate therapeutic dose of psilocybin that accounts for these variables.
In addition to safety considerations, there is also a high likelihood that people engaging with psilocybin therapy while still on SSRI or SNRI antidepressants will be left underwhelmed as a result of the dampening effects that these medications have on the psychedelic experience. As a result, the presence of these medications will often mute the therapeutic potential of psilocybin therapy.
However, one clear contraindication between a psychiatric medication and psilocybin is when the medication lithium is involved. A high percentage of lithium users (47%) reported seizures in their psychedelic reports in a self-reported study.
Given that lithium is most often prescribed as a mood stabilizer, people taking lithium also likely have the very mental health conditions (i.e., bipolar disorder) that would typically preclude them from receiving psilocybin therapy after completing a proper screening protocol.
Substance Use and Addiction as Psilocybin Contraindications
Those with current alcohol or substance abuse, occurring in the past year, may also be excluded from psilocybin therapy. This is due to several reasons:
- Impairment and Suppression: Mixing psilocybin with alcohol or opioids can increase the risk of injuries and accidents due to confusion or impaired judgment and coordination. Substances such as alcohol and opioids may be used as avoidance mechanisms by those who are addicted to them, which will suppress psilocybin’s ability to catalyze any sort of real therapeutic state. As a result, someone who is currently addicted to another substance or engages in avoidance behaviors is most likely unprepared for psychedelic therapy.
- Greater unpredictability: Active substance use introduces a potentially more unpredictable ‘set’ (or mindset), which can increase the risk of negative psychological reactions. For example, one study found that many psychedelic users who had challenging experiences combined psychedelics with alcohol and cannabis.
- Underlying medical conditions: Chronic substance and alcohol use can lead to liver, kidney, and heart conditions. Since psilocybin transiently increases heart rate and blood pressure, this can pose a risk to people with pre-existing or unstable cardiovascular issues related to regular substance use.
- Withdrawal symptoms: Quickly and suddenly quitting alcohol or a drug to which someone is dependent – to access psychedelic therapy – can lead to withdrawal symptoms, which may be physical or psychological in nature, or both. At worst, weaning off so suddenly is simply unsafe. Assuming a person is physically able to participate in psilocybin therapy, such a rapid shift will likely create a negative ‘set’ in which to have a psychedelic experience, and it would increase the chances of distressing experiences.
However, this doesn’t mean that substance use, which doesn’t meet the criterion of addiction, is excluded from psilocybin therapy.
Psilocybin safety also isn’t usually jeopardized if someone currently smokes, so a current smoking habit is not an exclusion criterion. In fact, researchers have shown that psilocybin therapy is safe and effective for the treatment of tobacco addiction.
Age Requirements and Brain Development in Psilocybin Screening
To participate in a psychedelic clinical trial, currently, you typically need to be aged 18 or over. In legal psychedelic therapy and psychedelic retreats, the age requirement is usually 21 and over (such as in Oregon), although many retreats (and even some clinical trials) exclude those younger than 25 years old.
One major reason for these age requirements is that the brain has not fully developed until the age of 25. (This is a bit of an oversimplification: the brain continues to change after the age of 25, including in significant ways, but a lot of the rewiring or pruning process in the brain does occur before the age of 25.)
Age requirements in psychedelic screening are based on concerns about longer-lasting negative effects, due to the brain being more malleable before the age of 25. In addition, the prefrontal cortex is still developing in adolescence (it matures much later than the limbic system, which processes emotions). The prefrontal cortex is important for emotional regulation. Psychedelic experiences can, at times, be challenging. So, if someone under 18 takes psychedelics, it is thought that they may have a harder time managing or processing intense or challenging psychedelic experiences.
However, it is not automatically risky to use psychedelics before the age of 25, as many cultures involve psychedelic use earlier in life than this. Researchers are also exploring the potential of safely administering psychedelic therapy to adolescents.
The risk of administering psychedelics to those younger than 25 may relate more to psychological readiness and support systems than brain development. Many of the adverse effects of adolescent substance use may be less from the consumption of a particular substance, but rather from many of the same factors we have outlined above (screening/suitability, preparation, set, and setting).
For example, in cultures in which psychedelic use among adolescents is normalized – such as the Santo Daime church, Amazonian ayahuasca sects, the Bwiti tradition, and the Huichol people of Mexico – psychedelics are approached in a prepared, ritualized, communal way. Psychedelics are also treated with the utmost respect. This cultural framework helps make the experiences safer.
The Psilocybin Therapy Screening Process Explained
The following screening process for psilocybin therapy usually involves the following steps or considerations. This is the screening process that we at MycoMeditations, after integrating the protocols from psychedelic clinical trials with our decade-plus of experience administering psilocybin therapy, have found to be the most effective in ensuring psychedelic safety and readiness:
- Application submitted: The application must be comprehensive and cover everything from reasons for attending a psilocybin retreat to mental health information, family mental health information, cardiovascular health, general health, medications, supplements, allergies, and understanding previous psychedelic experiences. This serves as a full-spectrum evaluation to identify any contraindications to taking psilocybin. This part of the psilocybin screening process also involves taking the participant’s support system, life stability, and readiness for psychedelic therapy into account.
- Initial consultation: The participant has an introductory conversation with a psilocybin therapist, facilitator, or retreat organizer. This involves discussing the client’s mental health history, current symptoms, and therapeutic goals. The aim is to establish initial eligibility.
- Further psychological, medical, and physical assessments: If the application and discussion raise any red flags, this stage of the screening process is an opportunity to follow up in the appropriate areas to safely approve that this participant can safely engage in psilocybin therapy.
- Informed consent: Potential participants are informed of the risks, benefits, procedures, and any unknowns associated with psilocybin therapy. Participants must provide written consent and are informed that they can withdraw from treatment at any point.
- Establishing rapport: During these initial interactions in the psychedelic screening process, the client and psilocybin therapy provider begin to establish a sense of trust and rapport, which is a key component of safety in psilocybin therapy. A participant needs to feel safe, prepared, and supported when enrolling in psilocybin therapy.
What To Do if Psilocybin Contraindications Are Flagged
If someone finds that their medical history excludes them from participating in psilocybin therapy, this doesn’t mean there are no options available.
For example, while psilocybin therapy risks may be higher now for a particular individual, that doesn’t mean they have to be in the future. At a later time, for instance, someone’s physical or mental health could be improved, or medication or substance use could change, in ways that make them eligible for psilocybin therapy.
But what should people do before they’re eligible for psychedelic treatment, or if, say, it’s unlikely they will be (due to a pre-existing medical or mental health condition)?
Fortunately, there are still other ways to improve mental well-being without psychedelics, including psychotherapy, medication, dietary and lifestyle changes, and social support. While other consciousness-altering activities (such as meditation) may benefit someone with a psychotic disorder, intensive meditation can also trigger or worsen psychotic symptoms.
Some non-classic psychedelics, on the other hand, are often considered safe for many people excluded from therapy involving classic psychedelics, such as ketamine therapy for those with bipolar disorder.
Researchers are also drawing attention to the potential of microdosing, or non-hallucinogenic psychedelics (also known as psychoplastigens), being helpful for those with typically contraindicated conditions such as schizophrenia and bipolar disorder. This is due to increased neuroplasticity while avoiding intense altered states. In the future, there could be ways for those living with schizophrenia or bipolar disorder to benefit from the brain benefits induced by psychedelics without risking the triggering or worsening of symptoms.
Responsible Screening Protects Participants and Preserves the Integrity of Psilocybin Therapy
An ethical psilocybin therapy provider should have a comprehensive psychedelic screening process in place. This is crucial for protecting the physical and psychological safety of potential participants. Without such screening, practitioners increase the risk of physical complications, psychological distress, and more serious and longer-lasting adverse effects.
Psilocybin therapy is not recreational; it is not to be taken lightly. It can pose risks if administered carelessly or unethically. This is why any legitimate psychedelic therapy provider must prioritize psilocybin safety. To better understand what this process should look like, click here to learn how to book a psychedelic retreat safely.
When psilocybin therapy is provided with the proper safety considerations in mind, eligible participants have the opportunity to have supported, transformative experiences that can offer profound and long-lasting benefits.
Psilocybin Contraindications and Screening: FAQs
What conditions make psilocybin unsafe for some people?
Psilocybin contraindications include serious cardiovascular conditions, as well as psychotic disorders, bipolar disorder, and borderline personality disorder. Also, women who are pregnant are advised to avoid psilocybin.
Why is psychological screening critical before psilocybin use?
Psychological screening minimizes the risks of intense psychological distress before and after psilocybin use. It reduces the likelihood that psychotic or manic symptoms will be triggered or worsened.
How do medications interact with psilocybin?
Some medications, such as SSRI antidepressants, increase serotonin levels in the body. Psilocybin does the same. However, there’s no conclusive evidence that using an SSRI antidepressant at the same time as psilocybin would lead to serotonin syndrome, or excessive (and dangerous) levels of serotonin in the body. This risk seems to be mostly confined to MAOI antidepressants.
What alternatives exist if psilocybin isn’t appropriate?
If psilocybin isn’t appropriate for someone, less risky alternative treatments include psychotherapy, medication, dietary and lifestyle changes, social support, and meditation (although intensive meditation may involve higher risks for some people). Ketamine is also showing to be a safe alternative for people who may have contraindications with psilocybin due to a personal or familial diagnosis of bipolar disorder.
How do ethical providers assess participant readiness?
Ethical psilocybin therapy providers assess people’s readiness in terms of their awareness of potential risks and benefits, intentions and therapeutic goals, and openness to the wide variety of psychedelic effects that may occur.

Who Should Avoid Psilocybin? Psilocybin Contraindications and Screening
The Legal Status of Psilocybin Therapy in 2026
Where is psilocybin therapy legal? This is an important question for anyone interested in therapeutic psychedelic experiences. Despite the growing body of research indicating the varied benefits of psilocybin therapy, legal forms of this treatment aren’t widespread (at least not yet).
While, of course, psilocybin mushrooms grow naturally all over the world, and can be cultivated easily, this doesn’t mean someone can replicate psilocybin therapy on their own. Moreover, despite easy access to psilocybin mushrooms, they may still remain illegal in the country in which they’re picked or grown.
For these reasons, many people who want to experience the mental health benefits of psychedelic therapy will prefer legal psilocybin therapy. This article will point you to where psilocybin is legal and what this treatment involves.
What is Psilocybin Therapy?
Psilocybin therapy involves taking synthetic or natural psilocybin in the presence of (typically) two therapists, normally one male and one female. The purpose of the treatment is to alleviate the distress associated with a mental health condition, such as depression, anxiety, or PTSD.
Clinical trials on psilocybin therapy have led to certain protocols relating to best practices. These include a playlist that augments the altered states; the wearing of an eye mask to encourage a deeper, introspective journey; preparatory sessions with a therapist before the dosing sessions; integration sessions after the dosing sessions; the use of moderate to high doses; and the encouragement for the participant to “trust, let go, be open” during altered states.
Through these protocols, participants who undergo legal psilocybin therapy have personally and spiritually rich experiences. It is the quality of these experiences that many researchers and facilitators believe drives therapeutic outcomes.
Why Psilocybin Therapy Laws Are Changing Worldwide
Since the 1970s, psilocybin has remained illegal in most of the world. And in most countries, it has sat in the most prohibited category of drugs (e.g., Schedule I in the US). This means governments in these countries, for decades, have created laws based on the position that psilocybin has no medical value and a propensity to lead to abuse.
Modern psychedelic research has challenged these long-held assumptions, which have lumped in psychedelics with drugs of abuse such as heroin, cocaine, and methamphetamine. Based on the mental health benefits that have been steadily proven through research, and a very low risk of abuse and physical harm, psilocybin therapy is increasingly becoming legalized.
Is Psilocybin Therapy Legal in the United States in 2026?
Psilocybin therapy is not legal federally in the US. It is not (yet) an FDA-approved treatment, so it is not accessible across the US. Federal law requires drugs to be approved as safe and effective by the FDA. If and when psilocybin therapy gains FDA approval – which could possibly happen in the next two years – the treatment can then be utilized and marketed across the US. However, the lack of FDA approval doesn’t mean that legal psilocybin therapy doesn’t exist in the US. Outside of federal legalization, psilocybin therapy has been legalized in certain jurisdictions (with more campaigns underway that aim to achieve the same in other states and cities).
US States and Cities with Legal Psilocybin Therapy Programs
Psilocybin therapy is legal and available in the states of Colorado and Oregon. Here is an overview of the differences between the programs available in these states:
Psilocybin Therapy in Oregon
- Psilocybin use outside of licensed therapy is not permitted. Psilocybin therapy is only available at licensed service centers.
- Psilocybin therapy is separated from other medical treatments, which means that licensed psilocybin service centers cannot offer this service alongside treatments such as diagnosis and psychotherapy. If someone wants these treatments alongside psilocybin therapy, they need to be sought outside a psilocybin service center. However, preparation and integration can be offered by psilocybin facilitators at service centers.
Psilocybin Therapy in Colorado
- Psilocybin use is permitted outside of licensed therapy, as the state decriminalized natural psychedelics for personal use, which also includes psychedelics besides psilocybin mushrooms, such as mescaline-containing cacti.
- Psilocybin therapy can be offered in more varied settings, including private residences (under strict rules).
- The law allows psilocybin therapy to be integrated with other mental health services, such as psychotherapy. This means that both supervised psilocybin experiences and psychotherapy with a licensed mental health professional can be delivered at the same clinic.
Psilocybin therapy will also soon be legal in New Mexico, although the rules and regulations surrounding the treatment are still being worked out, and it won’t be available until December 2026.
There is also active legislation in the following states (meaning psilocybin therapy could soon be legalized): Alaska, Georgia, Illinois, Indiana, Iowa, Kansas, Kentucky, Maine, Massachusetts, Minnesota, New Hampshire, New York, North Carolina, Rhode Island, Utah, Vermont, Virginia, and West Virginia.
Below is a map that shows the various levels of legalization, active legislation, clinical research, reform, and more for psychedelics (including psilocybin therapy) within the United States on a state-by-state basis.
Where is Psilocybin Therapy Legal Outside of the US?
Psilocybin is fully legal in Jamaica and the Netherlands, meaning there are no specific requirements for accessing psilocybin therapy legally or for how practitioners must provide it. As a result, these are the countries where psilocybin retreats have become the most popular.
Psilocybin therapy, as practised in the medical model, seen in clinical trials, is legal – for the treatment of certain conditions – in Australia, New Zealand, Czechia, Germany, Canada, and Switzerland.
Psilocybin is also decriminalized in Portugal and Spain. This means that the cultivation and sale of psilocybin mushrooms is still illegal, but criminal penalties have been removed for possession and use of them.
What “Legal” Actually Means in Psilocybin Therapy
When we refer to ‘legal’ psilocybin therapy, we mean that the use of the psychedelic psilocybin is being used in compliance with specific national or state laws. This might include the use of psilocybin for only certain conditions, such as treatment-resistant depression or end-of-life distress, which have not responded sufficiently to other treatments.
Psilocybin therapy clinics also need to meet certain requirements before they can obtain a license to operate, such as employing specific staff (e.g., psychiatrists, licensed facilitators), implementing safety protocols (e.g., screening clients), and ensuring adequate storage facilities for psilocybin and hygiene standards. Other requirements may include a certain number of preparatory and integration sessions.
Legal psilocybin therapy sessions take place in licensed facilities, clinics, hospitals, or retreats, not at home or in underground therapy sessions or retreats. Legal psilocybin therapy also involves supervision and guidance from one or more trained professionals (e.g., licensed therapists or national- or state-sanctioned facilitators).
Risks of Psilocybin Therapy Outside Legal and Regulated Settings
Legal psilocybin therapy, like any treatment, is not risk-free. However, it has safety protocols in place that minimize these risks as far as possible. Through adequate screening, preparation, and support during dosing and integration sessions, the vast majority of psychedelic therapy participants won’t experience any long-term issues as a result of treatment. This is not to say that even rigorous clinical trials involve no adverse effects; sometimes, this can happen, and researchers are continually learning lessons from these cases.
Yet, many safety protocols are lacking outside of legal frameworks, which increases the chances of an adverse experience. When psilocybin therapy is carried out in an underground setting, the following risks may apply:
- If clients (or facilitators) are sourcing psilocybin, they may not be aware of the specific strain of mushroom or the potency of the mushrooms being used. In legal psychedelic therapy, in contrast, synthetic psilocybin allows for more accurate psilocybin dosing. Even when natural psilocybin is used, in the form of whole mushrooms or extracts, regulatory requirements lead to more precise dosing than using psilocybin mushrooms sourced from the black market, as cultivation environments are highly controlled and monitored by law. Psilocybin mushrooms are often tested for psilocybin content within legal jurisdictions. Without accurate dosing, participants may find themselves having a much more intense (and distressing) experience than expected.
- There is no requirement for a psychedelic therapist or facilitator to be licensed or to have received any training to gain appropriate qualifications to guide clients through psilocybin therapy. One potential risk of a lack of training is that guides aren’t equipped to safely administer different doses and the nuances involved in selecting the appropriate dose for a participant.
- There are no complaints or mediation processes in place in case an underground facilitator engages in unethical behavior.
- Psilocybin products are not tested: this is a problem because many ‘psilocybin’ products in the black market actually contain 4-AcO-DMT (which, while it most likely converts to psilocin in the body, it has different dosages than psilocybin and there is little research on it).
- There is no requirement for any number of preparatory or integration sessions to take place, or for therapeutic frameworks to be in place that ensure people are adequately prepared for the experience and have support following psilocybin therapy.
- It is easier for unscrupulous practitioners to operate in underground settings, which makes it difficult to know who is trustworthy. This worry is not an ideal way to enter a psilocybin therapy session.
The Future of Psilocybin Therapy Legislation
If FDA-approved, psilocybin therapy would be available to all citizens of the US. This FDA approval would also mean that someone could potentially use their medical insurance plan to cover the costs of treatment.
However, there are campaigns in other countries that are calling for the medical legalization of psilocybin, including the United Kingdom. If psilocybin therapy were more widely legalized and accessible, this would make it easier for those who need it most to access this treatment.
Understanding Psilocybin Therapy Laws is Essential Before Participation
If you want to feel safe and confident in a psilocybin therapy program and the facilitators leading it, then it’s essential to understand the legal context. Not understanding this could lead to unexpected practices or oversights (which you may have assumed wouldn’t have occurred).
In a fully legal setting, high ethical and safety standards are in place, which make malpractice far less likely. Without an understanding of the legal context, one might also overlook the possible legal ramifications of possessing and using psilocybin if something were to go wrong. In a worst-case scenario, this could lead to criminal prosecution, penalties, or a criminal record.
Joining a legal psilocybin therapy program, offered by MycoMeditations, for example, means that you can be free of any of those worries. Rather than stressing about how to navigate psilocybin therapy’s complex legal environment, our psilocybin retreats ensure total legal compliance and the highest therapeutic standards, allowing you to put all your focus into your healing, which is what matters most.
FAQs About Psilocybin Therapy Legality in 2026
Where is psilocybin therapy legal in 2026?
Psilocybin therapy is legal in the following US states: Colorado, Oregon, and New Mexico. It is also legal in Australia, New Zealand, Czechia, Germany, Canada, and Switzerland under stricter medical access.
What’s the difference between decriminalization and legalization?
Decriminalization means that someone won’t receive criminal penalties for possessing or using (certain amounts of) psilocybin products. The cultivation, sale, and marketing of such products are still outlawed. Legalization, in contrast, means that growing, selling, and marketing psilocybin products is not prohibited.
Can people legally participate in psilocybin therapy today?
Yes, but only in the jurisdictions noted above. Outside of these states and countries, participating in psilocybin therapy may be decriminalized or illegal, with varying criminal penalties in the latter case, depending on the jurisdiction.
How do international laws for psilocybin differ from US regulations?
Internationally, psilocybin is a controlled substance under the UN’s 1971 Convention on Psychotropic Substances. This requires member nations to prohibit general use, allowing it only for strict medical or scientific research. This contrasts with some US regulations, in states such as Colorado and Oregon, which allow limited legal access to psilocybin therapy due to state-sanctioned psilocybin therapy programs.
How might psilocybin therapy laws change in the future?
Many US states have active legislation related to psilocybin therapy, so it’s likely that, in the near future (i.e., the next couple of years), we will see more states legalizing this treatment. In the near future, we may also see more European nations legalize psilocybin therapy. However, these legislative changes, including how quickly or slowly they occur, depend in large part on the pace of research.

Where is Psilocybin Therapy Legal in 2026?
Inside the World of Jamaican Mushroom Retreats
Jamaica is one of the most popular destinations for guided psychedelic experiences, particularly when it comes to retreats involving psilocybin mushrooms. Many people are opting for a Jamaican mushroom retreat for many reasons: psychological healing, a profound reset, new perspectives, personal growth, the discovery of meaning and purpose, or a renewed sense of spirituality.
In this comprehensive guide on Jamaican mushroom retreats, we’ll be taking a look at why the Caribbean island is a premier destination for these retreats, what happens during a mushroom retreat, and all the practical details you need to know before attending one.
Why Jamaica Is a Leading Destination for Psilocybin Mushroom Retreats
The first reason why a Jamaican mushroom retreat appeals to many people is that it will be fully legal. Psilocybin mushrooms are legal to cultivate, sell, possess, and use in Jamaica. By attending a mushroom retreat in Jamaica, you can be safe in the knowledge that your retreat experience isn’t illegal in any way.
Legal mushroom retreats tend to have higher standards of safety, ethics, quality control, and professionalism compared to illegal, underground ones, which will be more secretive. Above-ground psychedelic operations are protected within the bounds of the law if anything negligent were to happen.
Jamaican mushroom retreats have the added appeal of taking place in a beautiful Caribbean setting. These retreats are often held in particularly sought-after, idyllic environments. For example, MycoMeditations’ Jamaican mushroom retreats are held in three locations: Blue Marlin and Rainbow Tree are on the island’s private, peaceful south coast, and Bluefields Bay takes place in the parish of Westmoreland, known for its grand mountains and crystal blue waters. Each retreat location offers picturesque views of the sea, the sound of the waves, quiet beaches, and palm trees. Natural settings help to create a feeling of calmness, awe, and positive mood, which is ideal for therapeutic psychedelic retreats.
What Happens Before a Jamaican Psilocybin Mushroom Retreat
Before a Jamaican psilocybin retreat, you will be in the preparation phase of the experience. At MycoMeditations, preparation for each session consists of guided discussions and personalized therapy with licensed mental health professionals. Preparatory sessions involve discussions about an attendee’s intentions, current mindset, and any fears they may have about entering the mushroom session.
This is complemented by an abundance of resources (guided meditations, reading material, music recommendations, and more) along with personal support made available in the weeks leading up to the retreat.
Preparation aims to help you enter the mushroom experience with openness, confidence, and a sense of readiness, which will be conducive to having a deeply therapeutic experience at your Jamaican psilocybin retreat.
Inside a Jamaican Mushroom Retreat: What the Experience Is Like
Jamaican mushroom retreats differ in their duration and schedules. Some might offer a single psilocybin mushroom experience, with a day for preparation and integration on either side of the session, whereas others offer more dosing, preparation, and integration sessions. Retreats that lean to the spiritual side may call their experiences mushroom ceremonies, compared to the sessions of a more therapeutic-focused retreat.
MycoMeditations offers an 8-day mushroom retreat. This includes a first day for arrival and settling in, three dosing days, three integration days, and a final day for farewells before departure.
The MycoMeditations retreat program is one of the most therapeutically intensive psychedelic retreats in the world. These three psilocybin sessions are conducted privately for each guest, the mushroom doses tend to be higher than what people will otherwise have access to, and there is an extremely high therapeutic intention behind every aspect of the retreat, including multiple-hour integration sessions.
Downtime is scheduled for much-needed introspection and relaxation. This time helps attendees reflect on psychedelic experiences from the day before, and about the next dosing session to come. Therapists and facilitators are there to assist in this process throughout the whole week.
Jamaican psilocybin retreats are usually group retreats, with MycoMeditations usually having 8-10 guests in our group experiences. However, private retreats are often an option, too.
What Participants Typically Experience at a Jamaican Psilocybin Mushroom Retreat
There is no single kind of experience that people have at a Jamaican mushroom retreat. This is because people bring their own life histories, mindsets, personalities, intentions, beliefs, and cultural and religious backgrounds with them. However, at MycoMeditations, we emphasize the transformative potential of a psychedelic retreat when working with psilocybin mushrooms in the optimal way. We understand the opportunity to provide people with profound psychological healing, regardless of the specific problem they want to address, when these retreats are curated in the right way. This speaks to the flexibility of mushroom retreats in Jamaica, where they can help alleviate and get to the roots of depression, anxiety, social anxiety, PTSD, end-of-life distress, chronic pain, or a lack of spirituality.
So, what is it about a psilocybin retreat that can address a wide variety of conditions? At MycoMeditations, we observe what many researchers have seen in studies on psychedelic-assisted therapy: significant and lasting reductions in chronic distress are often related to the quality of the psychedelic experience people have. On dosing days, Jamaican mushroom retreat attendees might experience:
- Novel insights (into themselves and their past)
- Powerful emotional release
- Feelings of peacefulness, bliss, awe, or joy
- Challenging emotions like anxiety and fear (which could be related to psychedelic effects or psychological material that arises)
- New (and healthier) ways of thinking about themselves and issues in their lives
- A stronger connection to their emotions and bodies
- Moments of self-transcendence
- Visions (which could be personal, geometric, archetypal, cosmic, or religious)
Many of these effects predict positive outcomes. The intensity of psychedelic experiences also predicts clinical improvements. This is why MycoMeditations opts for high-dose experiences (which reliably involve stronger effects). Taking a high dose of psilocybin mushrooms on one’s own, or without adequate psychological support, can be risky. But when done with sufficient preparation, professional support, and integration – and in a calming, optimized setting – these risks are mitigated.
At MycoMeditations, we consistently observe transformative psychedelic experiences through this approach. Our emphasis on adequate preparation and integration support also helps people achieve more profound changes (both during and after the retreat).
Safety Protocols and Ethical Standards at Jamaican Mushroom Retreats
A legitimate Jamaican mushroom retreat should prioritize high standards of safety for all of its attendees.
The MycoMeditations team consists of trained, licensed therapists and facilitators with years of experience under their belts. Many have received mental health and psychedelic facilitation training, and they have helped guide and supervise many guests navigate altered states of consciousness throughout our lengthy history, making them some of the most experienced psychedelic practitioners. Their level of knowledge, skills, experience, and warm personal qualities help ensure that participants feel safe, protected, and looked after during their psilocybin retreat experience.
MycoMeditations also places great emphasis on offering inclusive and approachable mushroom retreats. This means that we don’t impose our own frameworks or belief systems onto guests. These days, it can feel like psychedelic retreats have to be delivered in a way that blends New Age spirituality, Eastern mysticism, and Indigenous beliefs and practices. While we recognize these frameworks work for some, they don’t for everyone (and in some cases, this blending is culturally insensitive or guilty of cultural appropriation).
To respect everybody’s diverse beliefs and backgrounds, we simply opt for compassionate, therapeutic care and help people form insights and conclusions based on the personal frameworks that resonate best for them.
Integration Support: What Happens After a Psilocybin Mushroom Experience
Integration support is an essential component of any Jamaican mushroom retreat. Psychedelic integration is the process of reflecting on a psychedelic experience and trying to find the insights, lessons, and meaning contained in it. Sometimes, this process of sense-making is obvious: the insights during the experience were clear and obvious. But other times, the experience (or certain aspects of it) might be confusing, ambiguous, paradoxical, or strange.
On integration days at MycoMeditations, guests are supported by therapists as they think through and discuss their psilocybin sessions, so they can discover the clearest and most relevant lessons. These lessons might relate to a person’s past, sense of self, values, attitudes, beliefs, relationships, habits, lifestyle, or career path. Professional supports deepens this process significantly by helping to open up new perspectives and healthy avenues of thought.

However, integration is not just about ‘turning altered states into altered traits’, that is, turning meaningful experiences into lasting, meaningful changes in one’s everyday life. For many people, it also involves landing safely and calmly back into ordinary life. Sometimes, it’s difficult to transition between one or more intense psychedelic sessions, in a retreat setting, back into one’s routine of work, city life, personal projects and hobbies, seeing friends and family, and (possibly) childcare.
This is why MycoMeditations prioritizes integration and aftercare. Dedicated integration days, group and private integration therapy, downtime, and resources for continued integration help ensure that mushroom retreat attendees feel grounded and ready to re-enter everyday commitments and lifestyles.
Post-retreat, we offer three stages of integration:
- 1st integration (2-3 weeks post-retreat): Adjusting to life back home and maintaining positive momentum.
- 2nd integration (4-6 weeks post-retreat): Seeing what changes have occurred and, if old patterns return, recognizing how they are best approached.
- 3rd integration (6-8 weeks post-retreat): Solidifying a healthy mindset and lifestyle to carry into the future.
Travel, Accommodations, and Logistics for a Jamaica Mushroom Retreat
Jamaican mushroom retreats will differ in their booking process, travel and accommodation options, and the logistics involved. Each retreat will have its own process to follow.
To book a Jamaican mushroom retreat with MycoMeditations, you first fill out an online application. After doing so, the MycoMeditations therapy team will review the responses, conduct a brief screening to make sure you’re well-suited for the retreat, and to ensure that a psilocybin retreat is a safe fit for you. The application is comprehensive and allows you to state your personal and family mental health history, experience with psychedelics (if any), medication and supplement use, and any special requirements or requests.
Once the application is approved, participants can select their preferred retreat location, date, and room. MycoMeditations offers different accommodation options, including shared and private rooms. Once registered for the retreat, the guided preparation process then begins.
Typically, Jamaican mushroom retreats include private transport as part of the package. This saves the hassle of arranging your own transport and ensures a positive experience as you transition in and out of the retreat setting.
For those with specific dietary requirements (e.g., vegetarian, vegan, dairy-free, gluten-free, coeliac), Jamaican psilocybin retreats should be able to make these types of accommodations for you.
Conclusion: Is a Jamaican Psilocybin Mushroom Retreat Right for You?
A psilocybin retreat in Jamaica is ideal for those who are open and ready to experience altered states of consciousness. Previous psychedelic experiences can help people feel more ready and prepared for a Jamaican mushroom retreat experience, but it’s not necessary. Retreat facilitators help those new to psychedelics feel safe and receptive to new states of consciousness.
A psychedelic retreat is also ideal for those who recognize that it is by no means a permanent ‘cure’ or ‘fix’ for a particular problem. Mental health issues, for instance, can be complex and deeply rooted. While legal psilocybin retreats offer significant and lasting decreases in distress, the long-term outcomes of joining a mushroom retreat in Jamaica will require continued effort and discipline with the ensuing integration process.
Nonetheless, many attendees experience significant and lasting reductions in emotional distress, allowing them to live life with a greater sense of ease, well-being, connection, and purpose. A psychedelic retreat can often be the catalyst for profound personal change when you join one that’s facilitated therapeutically and responsibly.
Mushroom retreats in Jamaica may be the right choice for you if you’re seeking psychedelic experiences within some of the most beautiful outdoor settings to complement your journeys, and if you’d like to access the most proven, therapeutic psilocybin retreat models to guide you through the next chapter of your healing.
Frequently Asked Questions About Jamaican Mushroom Retreats
What makes a Jamaican mushroom retreat different from other retreats?
Jamaican mushroom retreats differ from Dutch psilocybin retreats in that they offer only psilocybin mushrooms, whereas the latter can only (legally) provide legal magic truffles. Jamaican psychedelic retreats also differ from other psychedelic retreats by only offering psilocybin mushrooms, if lawfully conducted. Other psychedelic retreats may provide psychedelics such as San Pedro cactus and Bufo (5-MeO-DMT), as well as Kambo and rapé (tobacco snuff) experiences.
What happens during a typical mushroom retreat experience?
Typically, participants spend days and weeks preparing for the experience. They have 1-3 psilocybin sessions on the retreat, as well as integration support sessions, and time for other activities such as walking, hikes, meditation, yoga, breathwork, and socializing.
Why is Jamaica a legal destination for psilocybin retreats?
Jamaica offers fully legal psilocybin retreats. Psilocybin mushrooms are not prohibited in the country. They are legal to cultivate, sell, possess, and use.
How do preparation and integration support the outcomes of a mushroom retreat?
Preparation for mushrooms retreats ensures attendees are aware of potential psychedelic effects and teaches them the best way to relate to and navigate the experience. Integration support, meanwhile, helps attendees reflect more deeply on what they experienced, encouraging new or more profound insights and lessons. In short, preparation maximizes the potential of positive, therapeutic experiences, while integration further deepens the therapeutic value of what was experienced on mushrooms.
Who should consider attending a Jamaican mushroom retreat?
A Jamaican mushroom retreat is ideal for those seeking a deeper approach to improving mental health, exploring spirituality, and achieving personal growth. It appeals to those who’ve found that conventional or alternative approaches have failed to offer the relief or answers they’re looking for. A psilocybin retreat, however, is not a panacea, and it shouldn’t be viewed or treated as a recreational experience.

A Complete Guide to Jamaican Mushroom Retreat Experiences
Psilocybin Therapy to Overcome Fibromyalgia
Often stigmatized and downplayed, the reality of living with fibromyalgia is more debilitating than many people are aware of. If you live with this condition, you are likely familiar not only with the crippling physical pain but also the profound mental health impact and cognitive impairment that can come alongside it.
With pharmaceutical treatments for fibromyalgia simply not providing the relief that so many seek, some individuals have begun to explore the power of psychedelic therapy. Early research suggests that psilocybin impacts the pain-processing systems in the brains of fibromyalgia patients and helps to treat depression and anxiety symptoms.
In this article, we’ll explore:
- The wide-reaching impact that fibromyalgia has on patients
- What psilocybin is and how it works in the brain
- How psilocybin may work to treat fibromyalgia
- A real-life story of overcoming fibromyalgia with the help of a psilocybin retreat
- Top considerations if you’re considering psychedelic therapy
Fibromyalgia Explained: Symptoms, Impact, and Current Treatment Options
Approximately 2% of the US population lives with fibromyalgia, or four million people, with a disproportionate number of these being women. Worldwide, prevalence rates can range from 2% to 8% in some countries.
Fibromyalgia symptoms are generally described as widespread pain and stiffness, fatigue, sleep problems, and brain fog. However, these often don’t encompass the individual’s full lived experience.
Living with fibromyalgia can have a debilitating effect on a person’s daily life. They may struggle to stay in work, keep up with hobbies that they enjoy, and socialize with family and friends. For some, even basic tasks like bathing or cooking a meal feel impossible. Physical symptoms can lead to a vicious cycle of emotional distress and social isolation, with 50% of fibromyalgia patients suffering from depression and anxiety.
There is no widely accepted cure for fibromyalgia. Common treatments for managing fibromyalgia symptoms usually take a multidisciplinary approach, incorporating medications, psychological support, physical therapies, and lifestyle changes. Pharmaceuticals are often used to ease symptoms and aid sleep, while psychological and physical therapies aim to help the individual cope better in their day-to-day life.
Many people will experience no significant improvement in their pain symptoms using pharmaceutical treatments, especially given the myriad side effects that come alongside pain, sleep, and depression medications. So it’s no surprise that some fibromyalgia patients are seeking out alternative solutions, including psilocybin therapy.
What Psilocybin Is and How It Works in the Brain
Psilocybin is a naturally occurring psychedelic compound found in “magic mushrooms.” The mushrooms have been used by Indigenous groups for healing and spiritual connection for centuries (if not millennia), and now, the Western medical and psychological field is slowly catching up to their potential.
Psilocybin works mainly by impacting serotonin signalling in the brain, which is heavily involved in perception, mood, and cognition. Once ingested, psilocybin is converted into psilocin, which binds to a wide range of neuroreceptors, notibly the 5-HT2A receptor, within the brain. These receptors are especially concentrated in the brain regions related to our sense of self, sensory processing, and emotional regulation.
This causes the default mode network (DMN) – the brain region linked to self-referential thinking and rumination – to become less tightly organized. At the same time, brain areas that don’t usually communicate start talking to each other, producing altered perceptions, changes in a sense of self, and ego dissolution at high doses.
Psilocybin also promotes neuroplasticity, which is the brain’s ability to form new neural connections. This makes it easier for people to make changes, quit old habits, and enforce new adaptive behaviors in the aftermath of a session.
How Psilocybin Therapy May Help Treat Fibromyalgia Pain
When it comes to fibromyalgia, psilocybin’s ability to interact with the serotonergic system – and possibly stress-regulation systems such as the HPA axis – plays a key role in its potential to relieve symptoms. Given that fibromyalgia pain sometimes arises from altered pain processing in the nervous system, essentially a hypersensitivity to pain, patients need a treatment that focuses on modulating the signaling that’s associated with pain transmission, perception, and amplification.
On the neurological level, psilocybin reduces DMN activity, enhances brain connectivity and flexibility, and modulates the serotonin signaling, which is thought to play a role in pain transmission, processing, and amplification in fibromyalgia. Essentially, by modulating pain-processing circuits in the brain, psilocybin can potentially reduce pain signals and sensitivity.
Patients also experience a window of psychological and neural plasticity, making it easier to “reset” counterproductive thought and behavior patterns that worsen pain symptoms. These new neural connections also bypass existing pain pathways, helping to reduce how strongly pain signals are transmitted and leading to a reduction in pain.
These neurological effects underlie psilocybin’s emerging clinical efficacy in treating mental health conditions like depression and anxiety, which often accompany chronic pain.
Psilocybin can also induce states of mystical experience, profound introspection, and emotional healing. When held in a safe therapeutic container, these experiences can help patients process trauma and grief surrounding their condition and change their relationship to their pain.
Psilocybin for Fibromyalgia Research: Current Studies and Early Evidence
Early research points towards psilocybin’s ability to help treat fibromyalgia.
In this 2025 pilot study, participants experienced less severe pain and less interference with daily activities, and had better sleep quality after psilocybin therapy. Some participants also developed a better acceptance of their pain. The study found no serious adverse effects associated with psilocybin use in fibromyalgia patients, and any side effects, such as headaches or short-term changes in blood pressure, were generally mild and temporary.
Another study from 2024 looked at how psilocybin changes brain activity in fibromyalgia patients using tools like EEG and MRI, aiming to uncover essential data that will inform the design of a potential randomized controlled trial.
This ongoing study plans to test whether low doses of psilocybin improve pain tolerance and mood in a larger group of fibromyalgia patients.
These initial papers indicate that psilocybin therapy shows promise by targeting both the physical sensations of pain and the psychological factors that can make pain worse.
Lisa’s Story: From Daily Debilitating Pain to Symptom-Free
Early clinical findings suggest promising outcomes – but they’re only part of the story. Behind the data are real people exploring new approaches to managing their pain. Lisa is one of them.
“I was an avid tennis player. What would start happening is that the racket would fly out of my hand. My hands and muscles weren’t working properly,” explained Lisa, a former MycoMeditations retreat participant who suffered from debilitating fibromyalgia for 10 years.
“Then it got to the point where I was missing work, and it got worse and worse. On some days, I couldn’t physically get out of bed. There were times when I passed out on the bathroom floor because I was in so much pain.”
Lisa’s symptoms led to her leaving her job and ending her relationship. She describes spending all of her energy on basic tasks like cooking a meal and showering, while her prescription medications meant she would spend most of the day asleep. “There was no quality of life, no entertainment, no socializing with friends.”
She explored the potential cause of her fibromyalgia being the Epstein-Barr virus, and found relief after starting a course of anti-viral medications. Her flexibility returned and her mobility increased substantially. But there were still unresolved symptoms. She felt stuck mentally and physically. While the virus was no longer active, the damage it caused remained.
Depression was an ongoing battle. But doctors told Lisa there was no way out, that fibromyalgia is a lifetime chronic condition and she had to come to terms with her diagnosis. The prospect of living with this pain for the rest of her life only worsened her mental health.
Ultimately, seeking answers for her depression was what led her to explore the idea of psilocybin therapy. “If I could get the depression managed, maybe I could find a better way to deal with the fibromyalgia.”
At the time, most available research focused on psilocybin use in cases of treatment-resistant depression. She found no information indicating psilocybin could help with her chronic pain, so she didn’t anticipate the significant pain-related benefits she ultimately experienced.
“The most amazing, life-altering week of my life”
Lisa signed up for an eight-day retreat at MycoMeditations. “I was absolutely blown away by what happened when I got there.”
“For the first time in 10 years, I had people around me that actually listened to me,” she described.
Her intention for the first dosing session was to deal with her fibromyalgia. During the journey, she felt as if her body was encased in concrete, but she wasn’t scared. “[I thought] my body’s healing. It wants me to stay still. So I’m going to stay still.”
“But then at the end of that journey, the concrete cracked, and I burst out of it. Almost like Superman with his cape.”

After the journey, Lisa’s pain was entirely gone. Knowing that this may not be permanent, Lisa felt empowered to embrace her pain-free state for what it was in the moment and started to formulate her intention for the second dosing session. This time, she would address her inner emotional pain.
In the second journey, she confronted childhood trauma and processed the guilt she carried about not taking her mother to a better-equipped hospital on the day she died. She felt the warmth of her mother’s love and realized that the circumstances of her passing didn’t affect the love she felt for Lisa.
On dosing day three, Lisa went on a peaceful, mystical-type journey. She described it as a perfect way to close out the two prior powerful healing sessions.
By the end of the week, she was able to go on the group excursion to YS Falls. “I started the week barely being able to walk off the plane. I finished it ziplining and bungee jumping into the falls.”
“It was the most challenging, but also the most amazing, life-altering week of my life,” she said. Not only impacted by the psilocybin journeys, Lisa also described the profound importance of the support she received before, during, and after the retreat from facilitators and other guests.
“The guidance and direction they give – that’s life advice that I still follow today,” she professed.
“[Before the retreat] I wanted to give up. They saved my life and gave it back to me.”
A Lasting Impact
Once back home, Lisa felt renewed and reenergized. Today, Lisa reports having no fibromyalgia symptoms. Her depression has lifted. She’s back to full-time work and living her life. And she’s still in touch with her retreat group – six years later.
She encourages anyone suffering from fibromyalgia to take their healing into their own hands, as she did. “Don’t let doctors tell you that you’re condemned to this for life. You don’t have to be stuck in that cycle.”
Considerations if You Have Fibromyalgia: Accessibility, Safety, & Legality
If you are someone living with fibromyalgia and are considering psilocybin therapy, there are a few things you should take into account when deciding on where to go.
Remember that psilocybin is a scheduled substance in many jurisdictions. While underground practitioners exist, consider whether you would feel safer in a legal setting. In the US, you can access legal psilocybin through regulated psychedelic therapy programs in Oregon and Colorado. If you feel called to a psychedelic retreat, then going abroad to Jamaica, where psilocybin is legal, may be a great option for you.
It’s also crucial to ensure the center you choose caters to your physical needs. You should have a comfortable space to rest before and after your psilocybin session, and the journey space itself should be set up so you can lie or sit in positions that are most comfortable for you. The setting should be accessible for those with limited mobility, and support moving around should be available, should you need it.
Finally, safety is paramount when ingesting any kind of psychedelic. This means that the people who guide you must be properly trained in psychedelic facilitation and grounded in a practice of ethics and integrity. Make sure that they take you through a thorough screening process to rule out any medical or pharmaceutical contraindications, and willingly answer any questions you have for them. Your facilitators should also have an understanding of fibromyalgia, the way it takes shape in a person’s brain and body, and how psilocybin may help to treat the condition.
A New Direction in Fibromyalgia Treatment With Psilocybin Therapy
While there’s more clinical research to be done on psilocybin therapy for fibromyalgia, early studies and anecdotal accounts indicate its promise as a novel treatment.
By promoting neurological shifts, psychological insight, and emotional processing, psilocybin can help fibromyalgia patients not only experience reduced pain symptoms, but also fundamentally change their relationship to their condition – and life itself.
Looking ahead, we hope to see rigorous, randomized controlled trials that explore the mechanisms at play in fibromyalgia patients under the effects of psilocybin and establish foundational treatment protocols.
At MycoMeditations, we offer a safe and supportive environment for those living with chronic pain to explore the power of psilocybin therapy. We combine science-backed frameworks with heart-led therapeutic care at our retreat centers in Jamaica. Discover more about our approach.
Psilocybin for Fibromyalgia FAQs: Safety, Risks, and Looking Ahead
How does psilocybin affect fibromyalgia-related pain?
Psilocybin is a promising treatment for fibromyalgia thanks to both neurological and psychological mechanisms.
Psilocybin promotes neuroplasticity and interacts with serotonin receptors in the brain, which play a role in pain processing and perception, as well as mood and cognition. The compound can also elicit a profound experience of emotional release and psychological insight, which often helps individuals with fibromyalgia change the way they relate to their condition, process trauma and grief around their pain, and make positive behavioral changes in their day-to-day.
What does research show about psilocybin and chronic pain management?
Research on psilocybin for chronic pain relief indicates that it has a positive overall safety profile and may help in reducing pain symptoms as well as markers of depression and anxiety in chronic pain patients.
Why might psilocybin therapy work better than traditional medication?
Psilocybin therapy may work better than traditional medication because its neurological effects last long after the dosing session, potentially resulting in a lasting reduction in pain symptoms, while prescription medication is usually taken daily to have an effect. Psilocybin therapy differs in that it takes into account the mind-body connection and the role of psychological and emotional healing in pain management.
Patients also often experience a window of neuroplasticity following a journey with psilocybin, enabling them to more easily break free from maladaptive patterns and build more positive, healthy behaviors.
Is psilocybin therapy safe for pain management?
When individuals undergo thorough medical and psychological screening to rule out any contraindications, psilocybin therapy is a generally safe option for those seeking chronic pain relief. It’s crucial that people with chronic pain receive sign-off from a healthcare provider to safely undergo psilocybin therapy, and do so with trained therapists and/or facilitators.
How could psilocybin change the future of fibromyalgia treatment?
Psilocybin could be a new frontier for fibromyalgia treatment, helping individuals attack the root cause of their pain, rather than just numb or manage symptoms. In order for psilocybin to become more accessible for those living with fibromyalgia, we need to see considerably more randomized controlled trials and the establishment of treatment protocols that demonstrate the potential of psilocybin therapy.

Psilocybin for Fibromyalgia: Potential Paths to Pain Relief
A Guide to Understanding Psilocybin Therapy
There is no simple answer to the question of how psilocybin therapy works. With the continued publication of new psychedelic research, we keep learning more about how psilocybin therapy alleviates distress in such significant ways across a wide variety of conditions.
Based on the research available, we understand that psilocybin therapy works on multiple levels, including our brains and many aspects of our psychology, including our emotions, personality, degree of self-insight, sense of connection, and sense of self.
In this article, we will unpack how psilocybin therapy works on these multiple levels, which also helps explain why this approach to mental health is so promising.
What is Psilocybin Therapy? And How Does This Psychedelic Treatment Work?
Psilocybin therapy involves a client with a mental health condition or concerns taking psilocybin – in synthetic, extracted, or whole mushroom form – in the presence of a therapist (or sometimes two). Unlike traditional talk therapy, clients aren’t encouraged to talk about their experiences during these psilocybin dosing sessions. Instead, the client will have preparatory sessions to discuss what they are struggling with currently, to help form their intentions for psilocybin therapy. Then, following the psychedelic session, integration takes place to glean the experience for meaningful shifts.
The Structure of Psilocybin-Assisted Therapy
The structure of psilocybin therapy has been constructed in a way to maximize psilocybin’s benefits and reduce its risks.
Preparation Sessions in Psilocybin Therapy and Why They Matter
Psilocybin therapy begins with a thorough screening process to ensure the client is safe and well-suited for this therapy. Screening involves assessing their current state of mental health, medication usage, learning their personal and familial mental health background, as well as reviewing their cardiovascular and physical health history.
Following the screening process, a client will have at least a few preparatory sessions with one of the therapists who will be supervising and supporting them during their dosing sessions. Setting intentions during the preparatory sessions can encourage valuable psychological material to arise when someone enters an altered state of consciousness. These preparatory sessions are also essential for giving clients the tools necessary for navigating altered states, which, at times, might feel intense, confusing, overwhelming, or challenging. A psychedelic therapist will often recommend that a client adopt an attitude of letting go, surrendering, trusting, and being open to whatever the experience has to offer.
Psilocybin Dosing Sessions and What Happens During Treatment
Psilocybin-assisted therapy tends to involve one or two dosing sessions. While many clinical trials studying psychedelic therapy, or psychedelic therapy when done in practice, involve two dosing sessions, more than one isn’t always necessary. A single session can be sufficient for the client to receive clinically significant improvements in their condition.
That said, psychological or transpersonal material that arises in the first experience naturally feeds into subsequent psilocybin sessions. In our experience as a psilocybin therapy retreat center, psilocybin sessions will have a compounding effect when done effectively. Healing often happens in layers, and earlier sessions set the stage for future sessions to deepen and expand the potential growth offered through psilocybin.
Psilocybin Therapy Integration and How It Leads to Lasting Change
After the dosing sessions, there will be several integration sessions with one of the psychedelic therapists. There tends to be an equal number of preparatory and integration sessions (e.g., three for each is pretty standard), but sometimes there might be more integration sessions than preparatory ones, and vice versa. The psilocybin therapy integration sessions are opportunities to explore various aspects of the experience, such as resurfaced memories, visions, positive or negative emotions, periods of introspection and insight, and existential and metaphysical themes that arose.
How Psilocybin Affects the Brain and Supports Therapeutic Change
When psilocybin is ingested, in any form, it converts to psilocin in the body. It is psilocin that causes psychedelic effects. Psilocybin is a pro-drug; it converts to an active psychoactive compound but is not itself psychoactive. Psilocin then binds to several receptors in the brain, most notably serotonin 5-HT2A receptors. It is this latter binding that results in psychedelic effects.
Separate from the potentially therapeutic psychoactive effects of psilocin, its action in the brain is also responsible for mental health benefits. It’s through its activity at 5-HT2A receptors that it’s able to promote neuroplasticity, which is the brain’s ability to reorganize its structure, functions, and connections. In several mental health conditions, including depression, brain regions linked to mood and cognition are smaller. There are also fewer neuronal synapses (junctions where neurons communicate) and smaller and fewer dendritic spines (small protrusions on neurons that receive synaptic inputs) in these regions.
Psilocybin, however, promotes neuronal growth, synaptic density, and dendritic spine density. It can rapidly increase the number and size of dendritic spines, leading to a greater overall density of synaptic connections. This enhanced neuroplasticity, crucially, also remains after the dosing sessions. Through these brain changes, as the normal structure and function of key brain regions are restored, people often experience an alleviation of their psychological distress.
The Therapist’s Role in Psilocybin Therapy and Client Support
In psychedelic-assisted therapy, the role of the therapists is usually to adopt a non-directive approach, including during the dosing sessions. This means they don’t encourage a client to explore any issue in particular or to guide the psychedelic experience in a specific direction. Their role, instead, is to let a person’s altered state of consciousness unfold naturally while encouraging them to embrace, rather than resist, whatever emotions, feelings, thoughts, or psilocybin effects arise.
This non-directive approach is client-centered. The client is viewed as having the solutions to their problems and the ability to arrive at them. This approach involves attentive and empathic listening, patience, guidance, and support – but, crucially, not interpretation. The client is encouraged to find their own sense, meaning, and insight in the experience. Psychedelic therapists, therefore, are best to avoid imposing their own thoughts and beliefs onto people’s experiences.
Psilocybin therapy can be a challenging experience for the client. There are times when gentle guidance and instruction are necessary to help the client work through a psychological block or to soften towards resistance.
The psychedelic therapist is there to utilize their experience with altered states of consciousness to help the client navigate these new, complex inner landscapes that psilocybin reveals.
What People Experience During Psilocybin Therapy
Psilocybin therapy works, in large part, due to what people experience during a psilocybin therapy dosing session:
- Emotional breakthroughs: The experience of emotional catharsis, insight into one’s emotions, experiencing painful emotions fully, or feeling a sense of closure about an emotionally distressing event or relationship.
- Psychological insight: These insights involve a more complete understanding of one’s past (especially one’s childhood and upbringing), family, relationships, values, goals, and authentic self.
- Positive emotions: Self-compassion, kindness, warmth, forgiveness, joy, and peacefulness.
- Addressing the root cause of emotional distress: Many of psilocybin’s benefits result from people confronting what causes them severe and prolonged distress, such as childhood or adult trauma, abuse or bullying, low self-esteem or feelings of unworthiness, grief, a sense of meaninglessness, or fear of death.
- Alternative models of self: Unhealthy beliefs about self can be replaced with a realistic, kind sense of self that takes into account one’s strengths and positive attributes.
- Spiritual encounters: Ego dissolution, a sense of unity, connection to something bigger than oneself (e.g., ‘the divine’, humanity, nature, the cosmos), transcendence of space and time, ineffability, sacredness, encounters with entities.
Evidence-Based Benefits of Psilocybin Therapy
We now have evidence (and several studies arriving at the same conclusion) that psilocybin therapy can:
- Alleviate major depression, treatment-resistant depression, generalized anxiety, end-of-life anxiety, social anxiety, PTSD, addiction, OCD, and anorexia.
- Lead to sustained personality changes, including increases in trait openness and reductions in trait neuroticism (both of which are associated with positive mental health outcomes).
- Increase one’s connection to nature, which is also associated with improved mental well-being.
- Enhance one’s connection to self, others, and the world, as well as encourage acceptance (instead of avoidance) of one’s emotions.
- Lead to lasting increases in trait mindfulness, which can be an important marker in positive well-being.
- Encourage healthy behaviour changes, such as taking up contemplative practices, spending more time in nature, and eating healthier.
How Psilocybin Therapy Used in Retreat Settings Differs from Clinical Trials
Many psilocybin retreats, including those organized by MycoMeditations, draw on the lessons and insights gained from psychedelic therapy clinical trials. This includes the use of a therapeutic dose of psilocybin, a carefully curated playlist, eye shades, a non-directive approach, and dedicated preparatory and integration sessions. The journey of the participant is often similar, where people have deeply personal and meaningful psychedelic experiences that lead to positive ripple effects long after the experience is over.
However, there are some key differences between psilocybin retreats and psychedelic-assisted therapy as done in the clinical trials.
First, psilocybin retreats tend to take place in group settings (although private retreats are often available, too). Second, psychedelic retreats take place in a natural, villa-type setting, not a clinical space. Third, psilocybin retreats often utilize more of an all-encompassing method in terms of approach, emphasis, structure, and facilitators’ backgrounds (some are trained therapists, but not all are). Fourth, all participants in psychedelic-assisted therapy, such as in a clinical trial, have a specific mental health condition, whereas psilocybin retreats are also open to those without such conditions, or to people with comorbidities (people with more than one mental health condition).
Who is a Good Candidate for Psilocybin Therapy?
A good candidate for psilocybin therapy is someone who:
- Has tried other approaches to mental health (e.g., talk therapy, medication, lifestyle changes, support groups) and experienced inadequate benefit.
- Feels ready for psychedelic therapy and is open to altered states of consciousness, which can involve unexpected or unpredictable effects, recalling painful memories, challenging emotions, and potentially mystical effects like ego dissolution.
- Does not have a personal or family history of a psychotic disorder or mania.
- Feels comfortable tapering off any current psychiatric medication with the guidance of their prescribing provider (this is typically a requirement before undergoing psilocybin therapy).
- Is not pregnant, has a history of seizures, or cardiovascular issues.
Conclusion: Psilocybin Therapy is a Powerful Tool When Practiced Safely and Intentionally
Psilocybin therapy can work if it’s approached in an intentional way and with adequate safeguards in place. This means treating psychedelic therapy with trust and openness. And for psychedelic therapy to be done safely, the therapists need to have high ethical standards and a commitment to supporting clients before, during, and after their psychedelic experiences.
When approached in this way, psilocybin therapy can help free people from the shackles of negative thoughts and beliefs about themselves. It can offer new perspectives – alternative ways of relating to themselves, others, and the world. Within this opportunity to experience a radically altered reality lies the transformative power of psilocybin therapy.
Frequently Asked Questions About Psilocybin Therapy
What happens in the brain during psilocybin therapy?
During a psilocybin therapy dosing session, psilocin binds to serotonin 5-HT2A receptors, which creates a cascade of brain effects, including increased communication between brain regions (that don’t normally ‘talk’ to each other). In other words, the typically segregated nature of the brain’s network structure breaks down, leading to greater global integration. The default mode network (DMN) – which is involved in self-reflection, sense of self, remembering the past, and imagining the future – is also weakened. There is also an increase in ‘brain entropy’ (randomness of activity). These effects together can lead to psilocybin’s effects, such as altered perceptions, an altered sense of self, healthier thought patterns, and mystical experiences.
How is psilocybin administered in a therapeutic setting?
In psychedelic-assisted therapy, psilocybin is usually administered in synthetic form, in a pill (although it can also be administered as a psilocybin mushroom extract or as whole psilocybin mushrooms). Synthetic psilocybin allows for the most accurate form of dosing, however. Psilocybin is also administered in high doses (i.e., high enough to induce mystical experiences). These doses would typically be 25 mg of psilocybin or 3–6 g of psilocybin mushrooms (depending on strain). The participant consumes the dose, then they are encouraged to lie down, put on eye shades, listen to music, and have a deeply internal experience.
Why is integration essential for positive results in psilocybin therapy?
Integration is essential for long-lasting benefits. This is because, while psychedelics rapidly increase neuroplasticity, this doesn’t mean that new brain connections (and healthier thought patterns) will be permanent. Integration sessions help to strengthen the positive insights, perspectives, and self-perception one gained during the dosing sessions. In addition, they not only help to strengthen and maintain positive thought patterns, but they are also opportunities to process and make sense of any psilocybin effects that were confusing or challenging. And this, too, can lead to self-insight and self-growth.
What does the research say about psilocybin therapy’s effectiveness?
The research so far indicates that psilocybin therapy is effective at alleviating a wide range of mental health conditions and emotional distress, as well as enhancing the well-being, sense of meaning, life satisfaction, mindfulness, and nature connectedness of participants.
Who should and should not consider psilocybin therapy?
Good candidates for psilocybin therapy are those who have tried other mental health approaches and experienced little to no relief. Additionally, it is best that psilocybin therapy candidates have actually tried other therapies. It is important to have a foundation of psychological work established for psilocybin therapy, as this is an intensive therapeutic approach. Those who would not be suitable would be those prone to psychosis or mania (and who may have used psychedelics in the past, leading to a triggering or worsening of psychotic or manic symptoms). Individuals with a history of seizures or heart problems may also not be a good fit. Further, people who have never engaged in a therapeutic process are better off starting talk therapy to first learn about how their past has impacted them, recognizing negative thoughts and beliefs, working with emotions in healthier ways, and other foundational understandings.

How Does Psilocybin Therapy Work?
Everything To Know When Booking Your Psychedelic Retreat
Once you’ve decided you want to have a psychedelic experience in a retreat setting, the question remains of how to book a psychedelic retreat safely and confidently. This means booking a retreat that prioritizes your physical and psychological safety, and which you feel confident about in terms of the psychedelic retreat’s standards and professionalism.
In this article, we’ll be looking at tips on how to book a psilocybin retreat confidently, which will take into account retreat safety, retreat preparation, what a safe guided psychedelic experience looks like, and integration support available.
Why Booking a Psychedelic Retreat Requires Careful Research and Safety Planning
If you want to book a psychedelic retreat, this isn’t something that should be rushed. It requires time and careful consideration of the options available to you. For example, there are many psilocybin retreats, and they’re not all the same. Some emphasize certain elements over others (e.g., the therapeutic over the spiritual). Some involve larger groups than others; some cost more than others, and so on.
If you don’t weigh up the personal benefits and costs of each retreat, you could end up attending a psychedelic retreat that doesn’t align with your preferences and needs. Moreover, not spending the time researching retreat safety, retreat preparation, and integration support might lead you to book a psychedelic retreat that doesn’t adequately pay attention to these elements.
Psilocybin retreats often involve having intense and highly personal psychedelic experiences. This is why you need to ensure a psilocybin retreat will look after your safety, so that you feel comfortable letting go, and that you’re supported before, during, and after the experience.
Understand the Legal Landscape Before You Book a Psychedelic or Psilocybin Retreat
Psychedelics are only legal in a few countries and several states within the US. Psychedelic retreats typically operate in these countries and jurisdictions; however, they also exist in countries where the compounds used are illegal.
If you want to book a psychedelic retreat safely, it’s crucial to understand the legal landscape first. If booking a psilocybin retreat, for example, you need to know the legal status of psilocybin in the state or country.
Is it fully legal, or only under certain circumstances (e.g., for particular mental health conditions or because of religious exemptions)? Is it decriminalized? Is it prohibited, and what are the legal penalties faced if one is found purchasing, possessing, or consuming psilocybin mushrooms?
To feel comfortable when you book a psychedelic retreat, ensure that the retreat is legal and not considered to be engaged in criminal activity by the law. Otherwise, the psychedelic retreat will be in an underground setting, where its operations are secretive and hidden. This will likely mean the organizers are less public about their safety standards and protocols.
If you want to book a psychedelic retreat, and not have to worry about legal consequences, you can find legal ones in Jamaica, the Netherlands, Oregon, and Colorado.
How to Evaluate a Psychedelic Retreat’s Facilitation Team and Credentials
To feel confident when you book a psychedelic retreat, it’s also important to research the facilitation team. First, a safe psychedelic retreat will have a facilitation team page on its website. If it doesn’t, that’s a red flag. We don’t recommend booking a psychedelic retreat if it’s difficult to find much information on the facilitators.
When reviewing the ‘Team’ or ‘About Us’ section on a retreat website, make sure that information about each member’s role, background, years of experience, and qualifications is included. You want to feel that the person who will be looking after your well-being before, during, and after your psychedelic retreat is equipped to do so. This means they have plenty of experience supporting people on their psychedelic journeys, and their role as a psychedelic facilitator is backed up by relevant personal experience, qualifications, and education as well.
In addition, before you book a psychedelic retreat, you can expand your research beyond the retreat website. Look up the members of the facilitation team who will be looking after you. You might find personal websites, social media pages, interviews, podcast appearances, and articles they’ve written – all of which can give you a sense of whether their approach works for you.
Assessing Safety Protocols: What to Look for Before You Book a Psychedelic Retreat
Next, you want to pay attention to factors related to physical and psychological safety. There are key indications that a psilocybin retreat prioritizes safety (and a lack of mention of these factors should be a red flag):
- Information on how to prepare for a psilocybin retreat, such as prioritizing physical and mental well-being, the importance of intention-setting, and tips on how to navigate psychedelic experiences.
- What retreat preparation looks like when you arrive at a psilocybin retreat, such as intention-setting during group discussions. Before you book a psychedelic retreat, you want to feel assured that retreat preparation is given ample time and consideration.
- Check whether or not the psychedelic retreat is informed by evidence-based best practices gained from psychedelic research. This might include information on the factors that predict transformative experiences and how to minimize the chances of highly distressing experiences from occurring.
- Adequate screening protocols: a psilocybin retreat should assess each participant for underlying medical conditions and mental health issues, a family history of schizophrenia or bipolar disorder, current medication use, and physical health. All of these factors can influence whether a guided psychedelic experience is a wise decision or not.
- The kind of support given during a guided psychedelic experience. Do you get a sense that the facilitators understand how to help attendees during intense, emotional, or turbulent psychedelic experiences?
- Adequate integration support: pay attention to how many integration sessions are included at a psilocybin retreat and what the integration consists of. Will there only be a short group discussion, or is there space and time for longer discussions and time to reflect? Are other activities offered that can aid integration, such as time for meditation, journaling, breathwork, creative expression, and walks in nature? A psilocybin retreat that prioritizes integration support will also provide information on how to continue with integration after the support, such as where to find integration therapists and integration circles.
Research the Location and Accommodation Options at the Psychedelic Retreat
To feel confident when booking a psychedelic retreat, the retreat location and accommodation will likely be important factors, too. Think about the precise location of the retreat. As well as potentially traveling to a different country or city, you may need to organize your own transport to the retreat, as often they’re in secluded settings. A legitimate psychedelic retreat should provide clear information on transport options and whether private transport is included in the cost of the retreat.
In addition, before you book a psychedelic retreat, think about whether the location feels comfortable for you. How would you feel about traveling on your own to a particular country or staying in a secluded, hard-to-reach setting?
A reputable psilocybin retreat should provide detailed information on the available accommodations, including whether it’s private or shared, the number of people per shared room, what the rooms include, and the cost of different accommodation options. Images should also be included. Psilocybin retreat attendees want to feel assured that they will feel comfortable and relaxed during their stay and not get any unwelcome surprises about their accommodations when they arrive.
Read Reviews and Participant Stories Before Booking a Psilocybin or Psychedelic Retreat
A reputable psilocybin retreat will have reviews and participant stories on its website. If a psilocybin retreat doesn’t have these, you need to ask why this is the case. Perhaps it’s a relatively new psychedelic retreat, in which case reviews and participant stories are scant. That’s a legitimate reason and not necessarily a cause for concern. However, a long-standing psilocybin retreat, which has published plenty of reviews and participant stories, is more likely to encourage a feeling of trust and confidence in newcomers.
But it’s not just the existence or number of reviews and participant stories that matter; what the testimonials say matters, too. A short review with surface-level praise doesn’t tell you much. Before you book a psychedelic retreat, check for mentions of the safety factors outlined above, as well as mentions of the kinds of psychedelic experiences people had and the benefits they gained from them. These benefits might include personal insights, catharsis, therapeutic effects, or spiritual experiences.
An even more encouraging sign for potential psychedelic retreat attendees is independent reviews, published on TripAdvisor or Retreat Guru. These give potential attendees further assurance that participants are generally happy with their experiences.
Conclusion: A Safe Psychedelic Retreat Begins with Readiness and Informed Decisions
We have considered many of the factors that help people make an informed decision when they book a psychedelic retreat. Another factor, unrelated to the retreat itself, is personal readiness. You need to feel physically and mentally ready for altered states of consciousness with psychedelics. These experiences can be intense, unpredictable, and emotionally charged. Due to the immensity of these experiences, we recommend that you only book a psychedelic retreat when you have a clear and wise intention for participating in this type of retreat.
Once someone has considered their level of readiness, then they can begin researching a psychedelic retreat, including all the relevant information available on the retreat’s website, as well as information about the retreat and its team that exists elsewhere. After doing this for several retreats (the time spent doing it is truly worth it), you can then book a psychedelic retreat with a high level of confidence.
Psychedelic Retreat Booking FAQs
How can someone safely book a psychedelic retreat?
Someone can book a psychedelic retreat safely by reading the relevant sections of several psychedelic retreat websites, reading independent reviews, and sending queries to any retreats if anything isn’t clear or mentioned.
What legal and safety considerations matter most?
The legal consideration that matters the most is the legal status of the psychedelics used, while the most important safety considerations are retreat preparation, how a guided psychedelic experience is conducted, and the level of integration support offered.
What questions should you ask retreat facilitators?
You should ask retreat facilitators about their level of facilitation experience, training, and approach to retreat preparation, guided psychedelic experiences, and integration support. You may also want to ask questions about dosing, as psilocybin retreats differ in their approach (e.g., the upper limit of doses, whether flexible dosing is offered on an individual basis, and if dosing tends to change between the first psychedelic session and subsequent sessions).
How do preparation and integration influence retreat outcomes?
Retreat preparation can affect the quality of a guided psychedelic experience, such as its psychological content and emotional quality. This is because users’ mindsets affect the nature of a psychedelic journey (e.g., whether it is insightful, therapeutic, spiritual, positive, or distressing). Meanwhile, retreat integration can affect whether (or to what extent) someone can process, make sense of, and meaningfully apply their psychedelic experiences.
What red flags signal an unsafe or unqualified retreat operator?
Red flags that signal an unscrupulous psychedelic retreat include a lack of relevant information on its website (or a lack of clear information), no team facilitation page (or inadequate information about facilitators), exaggerated or misleading claims or promises on the website, few or no reviews or testimonials, many negative reviews, and several accounts of negative experiences shared by word-of-mouth.

How to Book a Psychedelic Retreat Safely and Confidently
A Complete Comparison of Psychedelic-Assisted Therapy and Traditional Talk Therapy
Psychedelic-assisted therapy is the combination of one or more psychedelic sessions and talk therapy. However, even though psychedelic therapy involves talk therapy, this doesn’t mean it looks the same as traditional talk therapy.
Many people will have tried talk therapy before showing an interest in psychedelic-assisted therapy. Traditional talk therapy can offer varying levels of success for people: some find that six weeks of cognitive behavioral therapy (CBT) sets them on the right track, whereas others may try other modalities for years without getting the relief they need.
Psychedelic-assisted therapy can be the catalyst that addresses the root causes of various mental health conditions in a much shorter timeframe than traditional talk therapy. Nonetheless, it’s also important to recognize that psychedelic therapy is not necessarily ‘superior’ to traditional talk therapy, or vice versa. What works for one person may not feel suitable for someone else. But where traditional talk therapy fails, psychedelic-assisted therapy offers unique benefits that can help those with deep-rooted and hard-to-treat psychological distress.
This article looks at the differences between psychedelic-assisted therapy and traditional talk therapy, so you know what to expect from both, including their benefits and disadvantages.
What is Psychedelic-Assisted Therapy?
Psychedelic-assisted therapy involves supervised psychedelic sessions. During these sessions, participants take a moderate-to-high dose of a psychedelic, such as psilocybin, LSD, DMT, or mescaline. Participants then lie down, put on eyeshades, and listen to a curated playlist, featuring music designed to match the arc of the psychedelic journey and facilitate greater emotional depth and transcendent experiences.
Psychedelic therapy typically takes place in a thoughtfully designed therapy room or in comfortable outdoor areas when done in a retreat setting. Whether taking place in a hospital for research purposes or at a licensed psychedelic therapy clinic, the room tends to include aesthetically pleasing art (such as nature-based art), ambient light, and plants. Participants typically lie down on a bed or couch for the duration of the session.

Under most clinical research protocols, two therapists (one male and one female) are present with the participants during their psychedelic experiences. They are there to provide psychological support or comforting touch if requested. The presence of therapists helps participants feel supported and safe as they experience altered states of consciousness.
Participants will also have preparatory sessions with the therapist, where they discuss intentions for the experience and how best to navigate altered states. Integration sessions with the therapist, which follow the dosing sessions, are also essential. These are opportunities for participants to process and make sense of what they experienced with professional help. This allows them to more effectively apply the insights and lessons they have gained to their lives going forward.
What is Traditional Talk Therapy?
Traditional talk therapy is much older than psychedelic-assisted therapy. The latter first emerged in the 1950s, with psychiatrists and therapists supervising people’s mescaline and LSD experiences in a clinical setting. Traditional talk therapy, on the other hand, originated in the late 19th century, with Sigmund Freud using it with patients in the 1890s.
Freud developed the psychoanalytic approach, the original talk therapy. The term ‘psychotherapy’ also came into use in the late 19th century, referring to treatments that involved ‘talking’ to the mind. ‘Talk therapy’ is the same as ‘psychotherapy’: the two terms are interchangeable. They both refer to the process of talking with a trained therapist to identify and change troubling thoughts, emotions, and behaviours.

Since Freud first developed talk therapy, many other therapy modalities have emerged. These therapy modalities differ in their approach – what aspects of the person’s life are prioritized, as well as how the therapist relates to the client. For example, psychoanalytic therapy and psychodynamic therapy (the latter evolved from the former) explore the unconscious, helping individuals address present-day problems by connecting them to past experiences, especially from childhood. Psychoanalytic therapy, however, is typically much more long-term than psychodynamic therapy.
Popular Psychotherapy Modalities and Approaches
- Cognitive-behavioral therapy (CBT): Changing unhelpful thought and behavior patterns.
- Mindfulness-based cognitive therapy: Becoming aware of present thoughts and feelings without judgment (this combines mindfulness with CBT).
- Acceptance and commitment therapy: Accepting difficult thoughts and feelings, rather than fighting them (this combines mindfulness with acceptance).
- Dialectical behavior therapy: This is based on CBT and teaches skills to manage intense emotions.
- Person-centered therapy: The focus is on self-actualization – where clients realize their potential – but the clients are encouraged to lead the sessions in this non-directive approach, which is different from a more therapist-directed approach like psychodynamic therapy.
- Existential therapy: The focus is on fundamental human concerns, which existentialist philosophers have focused on, such as meaning, freedom, responsibility, isolation, authenticity, and death.
- Somatic therapy: A body-centered approach that focuses on the connection between the mind and body. It is often considered a form of trauma therapy, using somatic approaches to release the trauma and stress believed to be stored in the body.
- Art therapy: Using creative practices – such as drawing and painting – to explore feelings, generate insights, and improve well-being.
- Internal Family Systems (IFS) therapy: Viewing the mind as an inner family, made up of ‘parts’ or subpersonalities, with some parts seen as ‘wounded’ and a core ‘Self’ that is compassionate and wise, and able to heal wounded parts.
- Transpersonal therapy: Helping people to realize their full potential by recognizing the spiritual dimension of life, such as transcendent experiences.
- Integrative therapy: This combines elements from other therapy modalities. It’s a flexible psychotherapeutic approach that adjusts which elements from therapy modalities are used and when they are used, based on the issues, goals, and needs that clients bring to sessions.
How Psychedelic-Assisted Therapy Works: Mechanisms, Brain Effects & Therapeutic Process
Psychedelic-assisted therapy works by offering clients meaningful experiences of altered states of consciousness to address the roots of their psychological distress. Research on psychedelic therapy suggests that this modality works through different possible facets of the experiences:
- Psychological insights
- Mystical experiences
- Emotional breakthroughs
- Alterations to the sense of self
- Increased connection to nature
- Entity encounters
However, it’s not just the acute subjective effects that predict the enduring mental health benefits of psychedelics. Personality changes, such as reductions in neuroticism, also predict these benefits, as do alterations to metaphysical beliefs. In addition, moderate-to-high doses of psychedelics, as used in psychedelic therapy, are believed to help address severe emotional distress by enhancing neurogenesis (the growth of new neurons) and neuroplasticity (the formation and reorganization of neural connections).
In several mental health conditions, such as depression, emotional distress is (partly) linked to the atrophy of neurons in certain brain regions. By generating the growth of neurons and connections in these brain areas, psychedelics can help restore them to their normal functioning.
Psychedelic-assisted therapy also works through its emphasis on integration therapy. Integration sessions occur soon after dosing sessions, which are thought to reopen critical learning periods. This is when the brain is in a malleable and open state, which helps enhance the benefits of integration therapy. By discussing insights and lessons from psychedelic experiences and continuing to develop a positive relationship with the therapist, a participant has a better chance of turning altered states into lasting positive changes.
Comparing the Benefits of Psychedelic-Assisted Therapy and Traditional Talk Therapy
While both psychedelic therapy and traditional talk therapy can help resolve some of the same mental health conditions, they differ in their advantages.
The Advantages of Psychedelic-Assisted Therapy
Psychedelic therapy offers benefits not seen in traditional talk therapy, including:
- Generally, a shorter time commitment: patients typically have two dosing sessions, plus a few preparatory sessions and several integration therapy sessions. Traditional talk therapy, in contrast, can involve one or more sessions a week, lasting for years (or even decades) depending on the therapeutic approach.
- Highly meaningful and spiritually significant experiences that have a lasting impact on people.
- Significant and enduring changes in the brain which are associated with improved mental health.
- Exploring deep layers of the unconscious and getting to the roots of emotional distress in a single session, which could take years with traditional talk therapy.
- The experience of emotional catharsis, which can insitigate large internal shifts to take place.
- Reliably enhancing people’s connection to nature, which is also associated with improved well-being.
The Advantages of Traditional Talk Therapy
Traditional talk therapy may be preferable to psychedelic therapy for the following reasons:
- It doesn’t involve intense altered states of consciousness, which may lead to acute distress or extended difficulties for some people.
- Many evidence-based talk therapies are safe and effective for specific conditions and concerns, whereas psychedelic therapy may not be safe for those prone to psychosis or mania.
- In most cases, psychiatric medication may not interfere with traditional talk therapy. But medication side effects, like‘emotional blunting’, can make it difficult to fully engage in therapy. Antidepressants can blunt some psychedelic effects. The interaction between antidepressants and psychedelics may also increase the risk of serotonin syndrome in some instances. This refers to a potentially life-threatening drug reaction that causes excessive levels of serotonin in the body. Traditional talk therapy avoids this risk.
- Even if traditional talk therapy is long-term (lasting a year or longer), it might still work out cheaper than psychedelic-assisted therapy, which could cost up to $10,000.
Who Might Benefit Most from Psychedelic-Assisted Therapy?
Psychedelic therapy is most likely to benefit people with deep-rooted trauma, hard-to-beat addictions, treatment-resistant depression, or end-of-life anxiety. This is because many people with these conditions find little to no psychological relief from psychiatric medications and various talk therapy modalities.
Psychedelic-assisted therapy, in contrast, may be a more effective form of trauma therapy. It can help offer people transformative and life-changing experiences, allowing people to address their addiction patterns, chronic depressive symptoms, and death anxiety. People who have struggled to get
This novel therapy can also be highly effective for people facing life challenges that are not necessarily rooted in trauma. Just as people engage in talk therapy when they don’t have mental health concerns, psychedelic-assisted therapy can be highly beneficial for people not seeking to tackle psychological issues. Regardless of the cause of emotional distress, psychedelics can unstick people from habitual thought patterns and offer new perspectives.
Who Might Benefit Most from Traditional Talk Therapy?
Traditional talk therapy would likely most benefit those who feel that using psychedelics would be especially daunting. It would also be suitable for those who already benefit significantly from psychiatric medication and don’t want to (or are advised not to) taper off them to participate in psychedelic therapy.
In addition, talk therapy may be best for people who want to explore and focus on a specific stressor, diagnosis, or type of talk therapy modality. For example, while a psychedelic experience may have existential themes, most psychedelic therapists aren’t existential therapists. Additionally, many psychedelic therapists have training in IFS therapy, and it may be utilized during psychedelic therapy, but somebody may want to focus exclusively on IFS without psychedelic medicine being involved.
Furthermore, traditional talk therapy may be best suited for those who’ve already experienced psychedelic therapy but who want additional integration therapy. Continuing talk therapy may help someone to enhance and maintain the benefits they gained through their psychedelic experiences.
Conclusion: Two Approaches with One Goal of Healing and Growth
Both psychedelic-assisted therapy and traditional talk therapy are mental health treatments with the same goal: healing from emotional distress and personal growth.
They might differ in how they achieve that goal (this applies to different therapeutic modalities as well), but the aim is still to address the root cause of distress and to live a life with improved well-being and relationships.
Finally, psychedelic therapy and traditional talk therapy are not opposed to each other; often one helps to enhance the other. Psychedelic therapy still involves talk therapy, and traditional talk therapy may involve therapy modalities (e.g., transpersonal therapy) that can be helpful for processing past psychedelic experiences.
As always, it’s important that people find the modality that works best for them in terms of their worldview, personality, and mental health needs. Whether someone opts for psychedelic-assisted therapy or traditional talk therapy, it’s also crucial that they find a therapist they trust and feel connected to, as this is another factor involved in both healing and growth.
Frequently Asked Questions About Psychedelic-Assisted Therapy vs. Traditional Talk Therapy
How does psychedelic-assisted therapy differ from talk therapy?
Psychedelic-assisted therapy involves the use of psychedelic compounds, combined with psychological support and integration therapy, provided by therapists. Talk therapy doesn’t involve psychedelics; the focus is just on talking with a therapist.
What types of mental health conditions respond well to psychedelic therapy?
Research shows that psychedelic therapy can be helpful for depression, generalized anxiety, end-of-life anxiety, addiction, PTSD, and OCD.
How important is integration after a psychedelic session?
Integration therapy, which often involves talk therapy, is critical after a psychedelic session. Integration helps people make sense of what they experienced and increases the chances of lasting positive changes in their lives.
When is talk therapy a better fit than psychedelic treatment?
Talk therapy may be a better fit for those seeking ongoing support or a more structured approach for specific mental health conditions. It may also be better-suited for people who have psychiatric contraindications or those for whom psychedelic treatment could cause a safety issue, like people living with schizophrenia or bipolar disorder.
What safety protocols exist for psychedelic-assisted therapy?
Safety protocols for psychedelic-assisted therapy include screening for mental health conditions and medications that can interact negatively with psychedelics; preparatory sessions that teach people how to handle challenging experiences; psychological support during difficult dosing sessions; and integration sessions that can help people make sense of the challenging or confusing emotions, thoughts, or visions that they experienced during the dosing session.